“There is no such thing as a ‘black cloud’,” your colleague jokingly retorts. “We all get the same chances to make the diagnosis and to do what’s right.” You give him your best pseudo-evil-eye as you continue to recount the number of unfortunate cases you’ve seen with the residents this evening already. An aortic dissection in an otherwise “healthy” 40 year-old, an intracranial hemorrhage in a 23-year-old following a cocaine binge, a cervical spine fracture in a patient who drove himself to the ED two days after his car accident, and an epidural abscess in one of your department’s frequent fliers. Black cloud or not, you’ve had one heck of an interesting evening, and you don’t anticipate it becoming mundane any time soon.
You wonder if you’ve spoken too soon when your intern comes up to discuss his next case. It’s an otherwise healthy 43-year-old female who comes to the ED tonight because she is having increased right upper quadrant pain. Your intern notes that she has had intermittent pain for the past few months, but tonight it became unbearable. She thinks the pain was worse after she ate dinner, and notes that she has had fevers and chills, but never took her temperature. She denies any nausea, vomiting, or changes in her appetite, skin or urine color. Her bowel movements have been normal as well. Her exam is only remarkable for right upper quadrant tenderness to palpation, and your intern thought she had a positive Murphy’s sign. Given the story, it is no surprise to you that your rock star first-year resident has committed to a differential that includes cholelithiasis, cholecystitis, pancreatitis, gastritis, or an atypical appendicitis.
Before you let him off the hook so easily, you throw out a few critical questions:
- “Is she pregnant?”
- “Nope, she’s had a hysterectomy.”
- “Does she have an acute abdomen?”
- “Nope, it’s otherwise soft, without rebound or guarding.”
- “What did her bedside ultrasound show?”
- “I was just about to go do it…”
You smile as your intern grabs the ED ultrasound machine and heads towards the patient’s room.
A short while later, your intern returns with the ultrasound machine in tow. “Can you take a look at these images with me?” he asks with a confused look on his face. “Something just doesn’t look right.”


What did he see on his bedside scan? What do you do now? Conclusion in the following
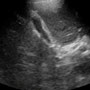
Your intern has captured multiple views of the gallbladder, which appears to be contracted with a thickened wall. Since wall thickness measurements are only useful for a dilated gallbladder, you move on. You note a faint acoustic shadow coming off the middle of the gallbladder; likely from a small intraluminal gallstone or dense collection of sludge (Image 1). As you scroll through the rest of his images, you pause to evaluate his images of the surrounding liver parenchyma. You note that the parenchyma doesn’t have the normal homogeneous appearance that you are used to seeing on your bedside scans. In fact, you think you make out three very distinct masses near one of the hepatic veins.

You confirm your intern’s suspicions that “something just ain’t right” and go with him to explain to the patient that more comprehensive imaging is warranted during her evaluation tonight. On further review, the patient states that she has unintentionally lost weight in the past few months, and that the pain may have been there longer than she was willing to acknowledge. She has been putting off her family’s recommendations to see a doctor because she was afraid of what it could be. After a lengthy conversation with her, she thanks you both for your comprehensive care and for helping to expedite her diagnosis and work-up.

You walk back to your computer with your head hung low to catch up on your dictations about all of the sad cases you’ve seen today, and you notice a piece of paper resting on top of your keyboard. Your colleague has left you a drawing of a single black cloud with a silver lining etched through the middle with the words “Dear Dr. Black Cloud…remember you are making a difference…” With a small smile, you pin the picture next to your desk and then move on to the next chart.

Pearls & pitfalls for Biliary Ultrasonography
1. Bedside ultrasound can provide you with valuable data to help you make critical diagnoses and expedite patient care. Always approach each scan with an open and inquisitive mind. You may be surprised by what you may find.
2. Always visualize the adjacent structures surrounding your target organ of interest. For example, when you seek out to evaluate the biliary system, scan through the surrounding liver parenchyma, too. Changes in the surrounding organs can alter the appearance of your target structure.
3. The gallbladder is normally dilated in disease or in the fasting state, but can be contracted soon after a meal. When the gallbladder is contracted, the walls naturally appear thicker so other sonographic signs are utilized to help make the diagnosis of cholecystitis (e.g. pericholecystic fluid, sonographic Murphy’s sign, etc.)
4. Studies have shown that systemic diseases, such as liver dysfunction or inflammation, cancer, heart failure, and renal disease can all lead to a more prominent and thickened gallbladder wall. This patient may not have acute cholecystitis, but may instead have gallbladder wall thickening secondary to the adjacent liver masses seen on bedside ultrasound.
5. When scanning through a target organ, obtain at least 4 different views of the area of interest. Use the body’s natural acoustic windows to improve your views.
6. Most right upper quadrant scans are performed with a low frequency curvilinear or phased array transducer. Become comfortable scanning with both types of probes, as each transducer has it’s own benefits and disadvantages. The curvilinear probe gives you a broader view with better resolution, whereas the phased array transducer allows you to slide the face in between rib spaces.
7. Be comprehensive with your scans. Don’t stop scanning just because you have found the answer you were looking for. Often times, interesting pathology can be discovered in the periphery of a focused scan. You may not always know exactly what you ar
e looking at, but at least you can provide the patient with the data and knowledge to take the next best step towards improving their care.
8. Practice Makes Perfect: With bedside ultrasound, there is no substitute for experience. The more scans you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is.









2 Comments
I could spend days to read these,
Thanks
Doc (M. Laperriere MD)
Interesting article – thanks