It’s been a busy afternoon. You are working on admissions with one patient chart in each hand and a cappuccino in your third hand. Triage walks back a haggard-appearing twenty-something with chest pain. “Can’t that go to fast-track?” you suggest hopefully. No luck.
“This guy was seen yesterday for the same thing,” answers the triage nurse. “You’re up,” he smiles, handing you a third chart. “Think of it as a few more RVUs.” You grunt something unintelligible, smile, and clamp the offered chart between your front teeth (figuratively, of course) like the trained gun-dog that you are.
The story is simple. “My chest is killing me, and that Motrin stuff is not cutting it,” the patient says. “It really hurts to breathe.” He woke the other morning with this upper sternal, pleuritic chest pain. There are no other exacerbating features, no fever or cough. The pain does not sound cardiac in nature. Vitals are normal, including an O2 sat of 98% on RA. The exam is normal, except for poor air movement on both sides due to severe pleuritic chest pain. Although the symptoms are low risk, you order pain meds and a screening evaluation including cardiac enzymes, an EKG and a D-dimer. There are no PE risk factors, and you are considering a chest CT – but you decide to look at yesterday’s chest X-ray first.
Which turns out to be a very productive use of your time. Radiology reading on this film from yesterday is “no acute findings.” But by this time, you are looking for something very specific.

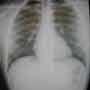
Dx: Missed Non-Traumatic Pneumothorax

Although the findings on the radiograph are subtle, the lack of apical aeration, compared to the left side, in the context of explained pleuritic chest pain, should prompt the wise EP to consider the diagnosis of pneumothorax.
Common errors in the ED often fall into several broad categories. First, there are errors of omission, where we fail to consider a diagnosis (like ischemic heart disease) or fail to order a relevant test (such as cardiac enzymes). Next, there are decision-making errors. In this type, we get the data, but fail to act in a clinically prudent fashion (e.g. elderly patient with hypoxic pneumonia, sent home). There are also errors of commission, where we order a medication on the wrong patient OR use an improper dose of medication (especially in pediatrics).
This case illustrates another type of error, namely the misreading of a diagnostic test. For EPs, some of the most challenging reads we face are interpreting EKGs and plain X-rays. Even though cardiology and radiology over-read these studies in nearly all hospitals, many facilities lack real-time readings. And the specialists are human just like us. They will miss things too.
The treating clinician, though not a specialist in radiology, has a distinct advantage over the radiologist, namely that he or she has examined the patient, formulated a provisional diagnosis, and approaches the X-ray with this diagnosis in mind. It is the outstanding radiologist who phones the ordering clinician and asks a question, and the exceptional one who will go and examine a patient themselves. I have met a few who have done this. So, in the case of a young patient with chest pain, the clinician specifically looking for a pneumothroax has an advantage over his/her colleague who does not have a pre-conceived diagnosis in-hand.
Disposition and treatment are easy in this case. How about some pain meds, a small chest tube, thoracic catheter or needle aspiration. Whether admitted or discharged, providing the right diagnosis is so much better than saying, “go home, there is nothing serious wrong with you,” only to have them return the next day with a larger, potentially more serious pneumothorax. In this case, the doctor’s brain scores the shot-on-goal, with a well-deserved assist from the doctor’s eyes.
Dr. Dallara practices Emergency Medicine in Virginia and North Carolina, and directs the Emergency Medicine PREP Course. www.emprepcourse.com
Editor’s Note
The management of these first-time spontaneous pneumothorax cases isn’t always straight-forward. What about simple needle aspiration of the pneumothorax, or even better yet, watchful waiting with repeat CXR after 6-hours? Go to http://tinyurl.com/6allbbs (October 2009 Journal Club) to find an extensive discussion on how using these less invasive strategies might safely avoid admission (and the painful chest tube!) for 74% of these cases.
-Christopher Carpenter, MD, MSc








1 Comment
This patient went to the ED initially. If this patient would have waited and went to a clinic for follow-up, as opposed to going to the ED again, would the results have been worse? What are the implications of this example for patients with unresolved chest pain after an initial ED visit?