Use ultrasound to diagnose – and quickly remedy – this acute urinary retention

An elderly man with a history of coronary artery disease, hypertension and benign prostatic hypertrophy on ticagralor (Brilinta), metoprolol (Toprol) and silodosin (Rapaflow) presents to the emergency department with an episode of acute urinary retention.
He is quite familiar with the symptoms and tells you he hasn’t been able to urinate since last night despite the urge to go. He complains of typical lower abdominal pain but denies fever, vomiting, weakness or other symptoms. On exam, he is in moderated distress and hypertensive. His temperature is normal, as is his pulse, but the latter you know might be partly because of the beta-blocker he normally takes. Other than suprapubic tenderness and fullness, the rest of the exam is normal.
You tell him you are going to get him feeling better by having your nurse place a Foley catheter attached to a leg bag, which he can drain at home. You also tell him that you’re have his urine analyzed and give him some intra-urethral lidocaine gel and pyridium by mouth in the hope of minimizing further discomfort by numbing things up without any of the side effects that stronger pain medications often cause. Your patient thanks you, and you tell him you’ll get back to him in about an hour when the test results are back. You enter the orders and ask him if he has any questions. “Nope,” he says, “I’ve been through this before more times than you’d care to know.”
A Turn for the Worse
You don’t expect to be engaged with this patient any further until it’s time for his dispo. However, about 15 minutes later his nurse finds you and says, “I placed the Foley and got 1500 mL of clear yellow urine back, but he doesn’t seem any more comfortable and his BP is still through the roof! He actually looks worse — can you come take a look at him?”
You figure the patient is probably fine, but you pay a visit to the bedside to be sure. Even though this is a new nurse, you agree with everything she said. The Foley bag is full, but the BP is still in the 190s, and he really does look uncomfortable. “How are you doing?” you inquire. “Doc, something must be wrong. I’ve had catheters a number of times. but it’s never been this uncomfortable. Can we take it out?”
“Let me take a look first.” you reply. “I’ll be right back.” You roll out the department’s bedside ultrasound machine. Searching for the bladder, you don’t find much, so you figure it must be decompressed.
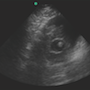
>>You do find the Foley balloon in its expected location, but something just doesn’t look right. What does the image above show? Scroll down for conclusions.


The image shows the Foley balloon apparently within a fairly large sized hypoechoic structure that does not look like the bladder. The balloon is actually inflated within the prostatic urethra – ouch! The labeled image on this page has the gain turned up a little bit to aid in distinguishing the enlarged prostate from urine remaining in the mostly decompressed bladder.
 Placement of the Foley
Placement of the Foley
The prostate is in the far field and is a bit hypoechoic in comparison to the white, hyperechoic surrounding bowel. The urine is in the near field and is hypoechoic. The Foley balloon has a hyperechoic rim and a hypoechoic center when it is filled with water. An internal echo may be seen from the tubing as it runs through the balloon. As it turns out the nurse was able to pass the catheter, but not quite all the way. The tip of the Foley catheter was actually in the bladder and was able to decompress it, but now there was a new source of pain – the Foley balloon blown up within the prostate gland. For comparison, we have included a correctly placed Foley in a decompressed bladder of another patient.
Given the size of the prostate, you decide that a regular Foley catheter just won’t do. You deflate the balloon and remove the existing catheter. Luckily, there is no blood at the urethral meatus, so you don’t think the prostatic urethra has ruptured. So, you place a Coude (French for “elbow) catheter in the bladder under ultrasound guidance. With the new catheter in place, the patient looks and feels much better. His UA was negative for signs of bacteria so he was sent home with a leg bag, instructions to increase his silodosin, and a follow-up appointment with urology in three days for reassessment.
As you can see, there are several takeaways from this case because, clearly, there are challenges whenever you perform a clinical ultrasound for imaging the prostate and bladder
Pearls & Pitfalls in Performing Prostate and Bladder Ultrasound
- Finding the Bladder: The urinary bladder is located in the pelvis, but with retention may protrude into the lower abdomen. Start with your probe just above the symphisis pubis and aim slightly inferiorly initially in case the bladder is decompressed. Urine in the bladder will appear as an area of dark black fluid (anechoic), and there will usually be some degree of hyperechoic posterior enhancement behind a fluid filled structure such as the bladder (see image). Measure the bladder size in three planes.
- Bladder Volume = [(A)(B)(C)]/2: Post-void residual bladder volume should be measured immediately after the patient completes a spontaneous void. Remember that the bladder is not a simple structure like a sphere or cube. To estimate the bladder volume, measure the bladder diameter in 3 planes (height, width, depth) and divide the product of these 3 measurements by 2. Bladder volume = [A x B x C]/2, or [A x B x C] x 0.5 where A, B and C are the height, width and depth. A normal post-void residual urine should be less than 50-100ml. Be aware that some experts recommend different formulas for estimating volume with values up to [A x B x C] x 0.75. Many ultrasound machines will have preset formulas and programs that estimate bladder volume for you. Simply enter the height, width, and depth measurements you obtained, and the computer will calculate the volume in mL’s for you.
- Finding the Prostate Gland: The normal prostate gland is hypoechoic (gray) and is located deep and inferior to the bladder (see image). It is usually round or apple-shaped and may have minor internal irregularities and occasionally calcifications that may produce an acoustic shadow.
- Prostate Size = [(A)(B)(C)]/2 or [(A)(A)(C)]/2: The normal prostate size in a young male is approximately 20 grams or 20cc which correlates to two finger-breadths or less. In an older male a normal prostate size is approximately 30 grams. Urinary retention is rare if the prostate is less than 40 grams and degree of urinary symptoms tends to correlate with size. However, this is not always true. If you assume the density of the prostate is similar to water then the size of this patient’s prostate is approximately [(6.6)(6.6)(5.4)]/2 =35.6g.
- Finding the Foley Balloon: The Foley balloon should be in the center of the bladder. Once the bladder has drained all you usually see is the balloon as the walls of a decompressed bladder can be difficult to distinguish from surrounding structures. The balloon has a hyperechoic rim and a hypoechoic center unless someone accidentally fills it with air. An internal echo within the balloon due to the tubing as it runs through can usually also be seen on ultrasound. Ultrasound can be used to watch inflation of the Foley balloon in real-time to make sure the balloon is not being inflated too proximally in the prostate or urethra.
Editor’s Note: Read one, do one, teach one
It was 11pm in early December. The patient was groaning with suprapubic pain. His Foley catheter output was grossly bloody. Quick, IV Dilaudid!
“What happened, Sir?”
“They put in my catheter in the ED this morning, I felt somewhat better, the catheter was draining well, but I still had pain. They said it was probably bladder spasm and sent me home. Then this afternoon the pain got really terrible, and my urine turned bloody. Please give me something for this pain!”
A few hours before my shift, I had proof-read Teresa and Brady’s Soundings – find the Foley. And then it hit me: That’s what this is! I grabbed the ultrasound machine and there it was, the Foley balloon within the prostatic urethra! Deflated the balloon; brought immediate relief. We replaced the Foley and the patient was smiling.
I gathered every resident and student to see the ultrasound image. Nobody had seen or heard of this before. But you can be sure none of them will ever make the same procedural error. Thanks Teresa and Brady!
Judith Tintinalli, MD, MS is the Editor-in-Chief of Emergency Physicians Monthly









1 Comment
Ouch! Yeah, inflating the balloon in the prostate happens, but usually the praxis is inflating slowly, checking for resistance, asking the patients if he experience pain and discomfort, if he does it’s immediately deflated and the catheter further advanced in the urethra to make sure the balloon is inside the bladder :).