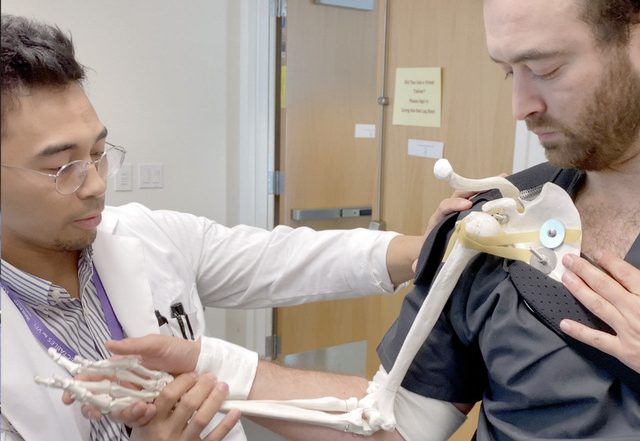
An inexpensive reduction trainer and demonstration model.
Shoulders are the most common large joint dislocations seen in the emergency department.[1,2] Multiple effective shoulder reduction techniques have been described.[3] There is no general consensus regarding the preferred approach, and the choice is largely left to clinician preference.
Techniques are typically learned by reading or watching videos, with little opportunity for clinicians to practice in a hands-on setting outside of clinical practice. This includes advanced practice providers, who are more frequently performing ED joint reductions.[4] When new techniques are developed, experienced clinicians usually must learn these techniques on live patients. Commercial trainers are scarce, expensive and limited.[5]
In our experience, an understanding of relevant anatomy is crucial for dislocation reduction success. We find it challenging to demonstrate the anatomic changes that occur during a shoulder dislocation and reduction through textbooks or media. Commercial trainers do not typically offer anatomic visualization.

We created an economical and easily reproducible model that allows clinicians to practice shoulder reduction techniques prior to performing them on live patients. The trainer also facilitates understanding of relevant anatomy by allowing visualization of important structures.
The base of the trainer is a right upper extremity skeletal model extending from the scapula to the hand. We drilled holes in the scapula, glenoid fossa and humeral head. We then attached bands from the scapular body to the humeral head with 3/16 inch bolts of varying lengths in the approximate positions of the supraspinatus, infraspinatus, and subscapularis muscles. The initial model used slingshot rubber bands.
Later, we exchanged them for penrose drains to make the model more reproducible. We secured the skeletal frame to a shoulder brace and added velcro straps taken from a shoulder immobilizer to the humerus and wrist in order to attach the trainer to a model patient. The dislocation maneuvers could then be attempted in conjunction with the model patient’s natural anatomy to help simulate a more realistic approach and feel.
An early problem was having enough force for the humeral head to reduce. In order to create the traditional “clunk,” the supraspinatus was split in two, with the additional band attached directly to the medial humerus. Repeated stretching of this supraspinatus band eventually resulted in the band breaking, but multiple reduction maneuvers were successfully completed prior to requiring replacement.
We also found that folding back the larger bands over the screws made them more durable to repeated stretching. Penrose drains have proven to be sturdy, but also begin to stretch with time. The clavicle from the skeletal model became malpositioned and we did not feel it was essential to the demonstration, so we removed it from the trainer.
We initially made the trainer to practice the external rotation technique. We have also found it suitable for practicing the Milch, Spaso, traction/countertraction and scapular manipulation techniques. Although it must be performed from the anterior instead of real-life posterior approach, the model is particularly useful for scapular manipulation because of the ability to directly visualize the movement of the scapula around the humerus.
The model is currently not a good option for demonstrating the Stimson or FARES (Fast, Reliable and Safe) techniques. The Stimson technique has proven difficult because the trainer is unable to grasp a weight for downward traction and lacks the sufficient structure to support a heavy weight. When attempting FARES, the humeral head will immediately snap back into place, making practicing the technique unrealistic.
Our experience sharing our model online has been incredibly positive. Brief videos demonstrating the trainer in use have had 99,000 and 28,500 views on Twitter and Instagram to date, respectively. Multiple commenters requested instructions regarding how to make the model and demonstrations of additional techniques. We created a YouTube video to show techniques that the trainer can demonstrate
The model is feasible for reproduction due to the low cost of supplies and equipment needed for assembly. We dismantled and put it back together multiple times to learn the instructions necessary for proper reproduction. We believe the trainer offers a means for new and experienced clinicians to practice proper shoulder reduction techniques in a low-stress simulation environment.
Special thanks to the Laboratory for Innovations in Medical Education (LIME) at Loma Linda University School of Medicine.

References:
- Zacchilli MA, Owens BD. Epidemiology of shoulder dislocations presenting to emergency departments in the United States. J Bone Joint Surg Am. 2010;92(3):542-549.
- Benjamin HJ, Hang BT. Common Acute Upper Extremity Injuries In Sports. Clin Pediatr Emerg Med. 2007;8(1):15-30.
- 3. Gottlieb M. Shoulder Dislocations in the Emergency Department: A Comprehensive Review of Reduction Techniques. J Emerg Med. Published online January 6, 2020. doi:1016/j.jemermed.2019.11.031
- 4. Clinical Practice Data. Accessed January 30, 2021. https://www.sempa.org/practice-management/clinical-practice-data/
- 5. M N Medical. Shoulder dislocation simulator. Accessed May 28, 2020. http://ismodel.info/home.html