It’s one of those average days in the ED where you work. It’s not too busy, but it’s not exactly what you would call slow either. Your shift has been a little bit on the boring side: lots of URIs, non-specific abdominal pain, low-risk chest pain, ankle sprains, and the occasional mild CHF or COPD flare. Also, too many people with the dreaded “multiple complaints” presentation.
You’re actually hoping for a trauma, a STEMI, appendicitis or something you can fix or at least treat. The next chart you pick up says “Right flank pain”. The differential diagnosis region of the right lobe of your brain immediately starts churning– pyelonephritis, nephrolithiasis, muscle strain – less likely, but not to be forgotten, are renal infarct, cancer, pulmonary embolism, shingles, pneumonia, gallstones, appendicitis – you stop there as you are about to enter the patient’s room.
Sitting in front of you is a Spanish-speaking female who states that she has been having pain on her right side for about 5 months. It is getting much worse, and tonight she thinks she saw blood in her urine. She’s been to a clinic doctor three times for this and each time they give her antibiotics for a “kidney infection”, but the pain is not going away. She denies any fever, nausea, vomiting, trouble breathing, radiation of the pain, change in appetite, or any other associated symptoms. She got scared when she saw the blood in her urine, so she got a friend to drive her in. Except for hypertension and asthma she is otherwise healthy. Her only prior surgical history is two C-sections. She’s never had a kidney stone or kidney infection and she has no family history of any significant diseases.
On physical exam, she appears to be fairly comfortable with normal vital signs except for her blood pressure, which is 180/122 mmHg. Her head and neck are normal to inspection. Her heart is regular and lungs are clear. She has symmetric pulses, bilaterally, throughout. Her abdominal exam shows mild diffuse right sided tenderness, both in the upper and lower quadrants, but more so at the level of the umbilicus. She does have right CVA tenderness as well, which seems to be more severe than her abdominal tenderness. Her urine is at the bedside and appears clear and yellow.
In terms of your initial differential diagnosis, you feel pretty confident that this is not pulmonary. If there is truly blood in the urine, it strongly suggests a renal process, but the “blood” could be a red herring. Perhaps she is menstruating or she ate beets or it was never really there. Although the differential is still broad, you doubt that she’s going to have appendicitis or gallstones. You decide to perform a quick bedside scan of her abdomen to determine how to proceed. If you see emergent pathology on her bedside renal and biliary scan, you can follow-up by ordering a comprehensive scan through radiology. If her kidneys and biliary system look pristine, you will proceed with a CT scan of her abdomen and pelvis to rule out the other etiologies you were considering.


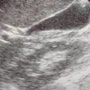
Here are two of the images you obtain. What do you see? In addition to a UA, CBC and BMP, what type of imaging should you order? Conclusion in the following
Dx: The Abnormal-Appearing Kidney


Your biliary scan demonstrates a normal gallbladder and normal portal triad with no gallstones, sludge, wall thickening, pericholecystic fluid, or other abnormal findings. The other ultrasound image shows a very abnormal appearing right kidney. On the scan, you can see the superior two-thirds of the right kidney and the bottom portion of the liver. The whiter (hyperechoic) area between them is perinephric fat. Bedside emergency renal ultrasounds are typically performed to evaluate for hydronephrosis. On this patient’s scan, you don’t see any evidence of hydronephrosis. However, the normal distinction between the hyperechoic renal pelvis and the more hypoechoic medulla and cortex is not visible either. The whole kidney looks abnormally homogenous. The discerning eye will also note that it appears both enlarged and “lumpier” than normal. Compare the abnormal kidney to the ultrasound image of a normal kidney below.
Unfortunately your patient ends up being diagnosed with renal cell carcinoma with metastases. This was not the type of break in the monotony that you were hoping for. As you explain the test results to her, the patient thanks you for your help. Although she is saddened by the test results, at least now she has a diagnosis and she can move forward with treatment options.
Pearls & Pitfalls for Evaluating the Kidneys
1. Getting Started: Use the low frequency (5 to 1 MHz) phased array or curvilinear transducer. Remember that lower frequency transducers enable better visualization of deeper structures. Start with the right kidney, which is easier to find, by placing your probe in the coronal plane at the right flank. Use the liver as a window and obtain a view of the kidney in the long axis. You may need to tilt your probe in an oblique angle to get in between the ribs.
2. Be Thorough: Image the entire organ using a fanning motion. Don’t just go for one pretty static shot through the middle. If you have a difficult time viewing either kidney, have the patient take a deep breath and then halt their inspiration. This brings both kidneys inferiorly. Obtain both long-axis and short-axis views of both kidneys. Any abnormal findings should be confirmed with comprehensive imaging either during that same ED visit or as an outpatient if the patient is stable for discharge.
3. Look for the Hydro: Hydronephrosis is seen as a black or anechoic area in the center of the kidney and usually represents downstream obstruction.
4. Compare Sides: Because most people have two kidneys, any questionable findings on one side may benefit from a comparison view of the other kidney.
5. Don’t Forget the Aorta: An aortic aneurysm often mimics renal colic, so always take a look at the aorta, even if your suspicion is low. It’s essential to practice looking a normal anatomy and even more essential to pick up an aneurysm before it ruptures.
6. Don’t Worry about Details: During an emergency bedside ultrasound you don’t need to visualize the actual kidney stone or determine if there are ureteral jets into the bladder. The main focus of a bedside renal ultrasound is to determine if hydro
nephrosis is present. However, if there is a major abnormal finding, like it this case, take your time and get a good look at the sonographic abnormalities so that you are more likely to recognize abnormal scans when you see them.
7. Avoid Pitfalls: The best way to minimize errors is through experience, so scan lots of normal kidneys, even when you are using the machine for other indications.









1 Comment
Flank pain tends to be localized on one side, beneath the ribs but above the pelvis, and sometimes in the small of the back.
Keep in mind that flank pain is a symptom, not a condition. Depending on the trigger, flank pain will present itself in different forms along with other accompanying signs showing kidney problems and different health issues.
http://www.doctorshealthpress.com/pain-articles/what-to-do-about-flank-pain