Visualize, visualize, visualize. The decision to resort to surgery is multifaceted, based on location of injury, amount of damage and patient co-morbidities.
It is Monday morning, and as you’re preparing for another barrage of patients who waited through the weekend to seek medical care, the first of your patients appears on the board as “Lac.” Since you’re just coming on, you grab your lidocaine, laceration tray, and irrigation materials to complete your history, physical, and laceration repair before you leave the room. Unfortunately, your left-handed patient has suffered a deep laceration to the palmar surface of his left hand with a piece of glass. He is neurologically intact and has pain with use of his long finger. Isolation of his flexor digitorum profundus (FDP) and flexor digitorum superficialis (FDS) shows normal strength and range of motion (ROM). Now, you change your plan: Anesthetize, obtain radiograph, irrigate, explore, suture, splint, and of course write for the life-saving tetanus vaccine. Your x-ray is negative for fracture or foreign body. Your patient is comfortable with local anesthesia, and you begin irrigating the wound to explore for the dreaded flexor tendon laceration. Of course, at this moment, the hand is edematous and bloody, limiting your visualization considerably.
So, at this point, what are the critical questions you should be asking?
- First, has the entire tendon been visualized?
- Second, is the surgical view sufficient?
- Third, doe the presence of full strength and ROM to the FDS/FDP rule out a flexor tendon injury?
Scope of the Problem
Let’s get to the answers by initially analyzing the scope of the problem.
Open injuries to the flexor compartment of the fingers and hand pose specific challenges to the EP both in terms of diagnosis and management. Unlike the extensor tendons, which are relatively close to the skin surface, the flexor tendons are buried deep in the palmar hand and surrounded by layers of muscle, fascia, nerves and arteries. There exists a complex pulley and synovial sheath system that is highly advanced to allow for proper dexterity and fine motor control. The amount of tension placed upon the flexor tendon system demands smooth gliding and unimpeded movement such that a relatively small flexor tendon injury can have long-term disabling effects on hand use whereas a similar extensor tendon injury would heal without issue.
While hand surgeons exclusively perform operative repair of flexor (and most extensor tendon) injuries, the diagnosis remains largely in the realm of the EP. Examination is often difficult and limited by the presence of small wound openings (punctures), bleeding, or patient cooperation.
In addition, while a complete tendon laceration is usually clinically evident, partial tendon lacerations are notoriously under diagnosed because the clinical examination is normal [1,2]. In one trial, 30% of flexor tendon injuries were missed by both EPs and surgical hand residents when explored outside of the operating room [1]. This suggests that limited visualization due to a variety of factors (inadequate time, light, instruments, and/or anesthesia) is a large factor resulting in missed injuries. Accurate diagnosis of these injuries depends almost entirely on the bedside examination and clinical suspicion, as imaging modalities such as MRI are not feasible in most settings.
Left untreated, partial tendon lacerations may progress to complete tendon disruption days or weeks later with subsequent tendon retraction or scar formation [3]. Once an injury is identified, most authors recommend operative repair of lacerations greater than 50% of the tendon width to prevent tendon rupture and debridement of the edges for lacerations less than 50% to prevent adhesion formation [4]. Therefore, a well-performed, exceedingly thorough, and even “neurotic” examination of the wound is obligatory for any EP who prefers spending days off with their friends and family rather than with a doctor of jurisprudence.
Review of Anatomy
Each digit in the hand (excluding the thumb) has two flexor tendons: the FDS and the FDP (the thumb only one flexor tendon — the flexor pollicis longus — FPL). The FDP penetrates the FDS at the base of the proximal phalanx as the FDS splits into two lateral slips. The FDS inserts on the proximal portion of the middle phalanx, while the FDP inserts at the base of the distal phalanx (figure 1).

Figure 1: Illustration of flexor tendon system in the finger.
(© AO Foundation, Switzerland. www. AOFoundation.org)
The FPL has its own synovial sheath that is located from the flexor retinaculum to the distal insertion site. The remaining digits have a common synovial sheath from the flexor retinaculum (located at the wrist crease) to the mid-palm. Then, distal to the metacarpophalangeal joint, each digit’s FDS and FDP are enclosed in one synovial sheath to the level of distal insertion. Biomechanical disadvantage is accepted in the fingers to reduce bowstringing, as pulley systems keep the tendons close to the bones and joints facilitating smooth flexion.
Assessing function is extremely important. The examiner should immobilize the other digits in forced extension, and ask the patient to flex the non-immobilized digit. Assessing the FDP involves placing the PIP in forced extension and asking the patient to flex the DIP joint, which may be the only way to assess an isolated FDP injury.
Visualize, Visualize, Visualize!
The key component to visualization of any suspected tendon injury involves exploring the tendon throughout a full ROM, as often an injury occurs during full flexion/extension of a digit, only to have the injured portion of the tendon disappear from view as the patient holds the hand in the position of maximal comfort. Doing so requires having the patient adequately anesthetized and ensuring that the surgical field is bloodless and sufficiently exposed. A simple exsanguination and tourniquet technique will provide a temporary bloodless field. Depending on EP experience and practice setting, a regional nerve block can provide outstanding anesthesia depending on the location of the injury [5]. Once the patient is anesthetized and the field made bloodless, exploring the tendon is now top priority. Don’t have a fancy plastics or hand tray with various retractors available? No problem, because a 21 or 23-gauge needle and a laceration tray at the bedside are all of the materials required.
Attach a 21 or 23-gauge 1.5-inch needle to a 3 mL syringe. Twist off the protective mechanism with either your hand or a hemostat (Figures 2-3).

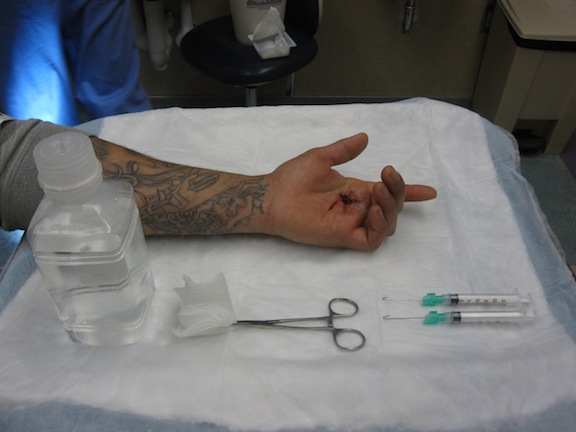
Figure 2: Mayo stand with materials required for wound exploration

Figure 3: Two 21-guage needles that have been modified into small soft tissue retractors
Apply a curve to the end of the needle with the hemostat, effectively making two tissue retractors (Figure 3). Place the retractors into the laceration/wound and retract gently, being careful not to damage nearby structures. At this point, have an assistant hold the hooks in place while exploring the wound thoroughly (Figure 4).

Maintain an extraordinarily high level of suspicion for tendon injury and prove beyond doubt that the injured area has been fully examined. Use gauze or a Q-tip along the tendon or tendon sheath to visualize any defects in the integrity of these structures. Passively move the affected digit through complete flexion and extension to assess for a concealed injury. Do not enlarge the field of view by incising the tissue further, as doing so may inadvertently damage adjacent neurovascular structures.
ED Management
Comprehensive management of flexor tendon injuries is beyond the scope of this article, but EPs would do well to keep several things in mind:
- Immediate hand surgery consultation is warranted in cases of poorly controlled bleeding, gross contamination, open fracture, or severe crush injury. Delayed consultation (prompt, 1-3 day follow-up can be afforded in cases of flexor tendon laceration < 50% or closed FDP rupture.
- Regardless of whether repair is attempted in the ED, flexor tendon lacerations should receive a dorsal splint (keeping the wrist somewhat flexed and MCPs flexed to about 70 degrees) and instructions to keep that splint on until hand surgery follow-up.
- Surgery will depend on several factors, including location of injury, amount of damage and patient co-morbidities.
Case Outcome
The patient had his hand explored in the emergency department and was found to have a 50% tear in the FDS in zone II. He was evaluated by a hand surgeon and was taken to the OR within hours and had operative repair of his FDS. The wound was closed primarily and he was placed in a dorsal slab splint with 30° wrist flexion, 70° MCP flexion and full extension of the phalanges. He was seen in clinic three days later and was doing well.
Flexor Tendons: Three Pearls of Widsom
- The flexor tendons are injured until proven otherwise in open/penetrating hand injuries.
- Up to 30% of wounds explored outside of a surgical suite have missed flexor tendon injuries, regardless of the provider performing the exploration.
- Provide the best surgical field by using a tourniquet and tissue retractors; do not extend incisions in the palmar region to improve the surgical view.
David Bosch, DO is a fourth year resident at the Denver Health Residency in Emergency Medicine.
Matthew Taecker, MD is a fourth year resident at the Denver Health Residency in Emergency Medicine.
Kerry Ann Broderick, MD is an associate professor of emergency medicine at Denver Health Medical Residency Program.
Michael Breyer, MD is an Associate Program Director at the Denver Health Emergency Medical Residency Program.
REFERENCES
1. Nassab R, Kok K, Constantinides J, et al. The diagnostic accuracy of clinical examination in hand lacerations. Int J Surg. 2007 Apr;5(2):105-8. Epub 2006 Jul 7.
2. Harrison B, Holland P. Diagnosis and management of hand injuries in the ED. Emergency Medicine Practice. [Online publication] 2005;7(2):1-28 (Evidence-based review)
3. Roberts, James R., Catherine B. Custalow, Todd W. Thomsen, and Jerris R. Hedges. 2014. Roberts and Hedges’ clinical procedures in emergency medicine.
4. Strickland JW. Flexor tendon injuries: I. Foundations for treatment. J Am Acad Orthop Surg. 1995;3(1):44–54.
5. Liebmann O, Price D, Mills C, et al. Feasibility of forearm ultrasound-guided nerve blocks of the radial, ulnar and median nerves for hand procedures in the emergency department. Ann Emerg Med. 2006;48(5):558-62.









1 Comment
While this is a great review, I call the hand surgeon for these. It is far too easy to miss something despite good visualization, and I don’t have the time to dig up a forearm for a stray ruptured tendon. This is not simply a malpractice issue, but a patient safety issue. They must have follow-up as a compartment syndrome is limb threatening.