Vitals show P 65, RR 24, sat 93% RA, BP 145/68, Temp 37.3 C. He has a history of coronary angioplasty, and is taking metoprolol 50mg daily.You round up the usual suspects: possible pneumonia or PE, rule out cardiac ischemia or CHF. ABG shows a PaO2 of 62 mmHg. Labs are pending, and a chest X-ray is shown below. You request admission from the hospitalist, who in turn requests a CT scan to “rule out PE.”
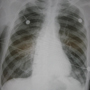
This chest X-ray is easy to misread if you’re in a hurry. If you step back, there is a hint of volume loss on the left side, particularly at the base. Homing in on this finding, you see that the L diaphragm is obscured, suggesting an isodense process in the lung – potentially either a pneumonia or pulmonary infarct from a PE.
 Note the lack of tachycardia in this patient on beta blockers. Even in the presence of dehydration and infection, beta blockers will do their pharmacologic duty and keep the heart rate from increasing (thereby blocking the appropriate physiologic response). Otherwise, one might tend to under-estimate the detrimental effect of (in this case) the pneumonia on the patient.
Note the lack of tachycardia in this patient on beta blockers. Even in the presence of dehydration and infection, beta blockers will do their pharmacologic duty and keep the heart rate from increasing (thereby blocking the appropriate physiologic response). Otherwise, one might tend to under-estimate the detrimental effect of (in this case) the pneumonia on the patient.
Also, consider the work-up of acute delirium (“dad is a little confused”). A strong argument can be made for admission in this case. The consequences of unrecognized delirium if the patient is discharged from the ED include increased ED recidivism (~80% return within 5-days for admission) and increased mortality at 3 months.
Finally, every patient with S.O.B. gets both blood cultures and IV antibiotics up front, lest we fall out of the 6-hour “quality” window for an atypical presentation of pneumonia. Forget the fact that many of these patients don’t end up having pneumonia, and that such practice runs up the cost of medical care and increases antibiotic resistance.



1 Comment
i just wanna know the treatment for [u][b]paracardiac pneumonia[/b][/u]