It’s midnight on a Friday and your next patient just happens to have been on the wrong end of a left hook. He is a 62 year old man who states he was assaulted with a fist to the face while walking home. He denies loss of consciousness and has been drinking. His only complaints at this time are right ear pain and some lateral neck pain. He has no other past medical history. His vitals are unremarkable. His exam is notable for some peculiar swelling of his right ear and alcohol intoxication. His tympanic membrane is unremarkable and the rest of a thorough trauma evaluation yields nothing. The good news is that you’re his doctor and his ear will soon be returned to its prior state, ready to face another day.
Auricular hematoma occurs when blunt shearing force is sustained to the ear, often times in cases of facial trauma or in sports like boxing, wrestling, and mixed martial arts. These forces separate the underlying perichondrium from the cartilage itself. This area is highly vascularized and bleeding between this space results in the formation of hematoma. The disruption of the blood flow to the cartilage from this injury subsequently leads to necrosis1.

Auricular hematoma occurs when blood accumulates between the perichondrium and cartilage of the ear
Our job in the emergency department is three fold: early identification, early drainage, and using various splints and bandaging techniques to prevent the re-accumulation of blood.
Thorough traumatic evaluation of the ear should be performed. This includes examination of the anterior and posterior aspect of the pinna and otoscopic evaluation as blunt trauma to the ear can often lead to tympanic membrane rupture. Early identification of auricular hematoma is paramount as the natural history of these injuries includes cartilage necrosis and subsequent fibrous deposition leading to a cauliflower ear deformity that later may require surgical excision. Spontaneous infection has also been described and if cartilage is exposed then antibiotics should be considered1.

An incision made to the top of the hematoma allows for better cosmetic healing as the scar will be concealed by the superior aspect of the helix
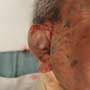
Drainage of auricular hematomas is the definitive treatment. Regional anesthesia is best achieved with a greater auricular nerve block. To obtain the best cosmetic result, an incision is made to the superior aspect of the helix as pictured above. Blood can then be expressed from ear with manual compression. Further clotted blood can be easily broken up and removed with curved hemostats.

Curved hemostats help evacuate clotted blood left behind
Several methods of dressing and splinting have been described in the literature to prevent the accumulation of blood after drainage. Buttressing the ear by sewing cotton pledgets was first used in the eighties. This idea was later modified to use buttons sewn to the anterior and posterior aspects of the ear1. These techniques however can be time consuming and cumbersome.
 Specialized thermoplastic splints were developed and can be formed to the ear. These do well in preventing re-accumulation, but can be expensive. In further researching this subject, we found that simply placing two to three absorbable mattress sutures along the involved portion of ear both prevents accumulation of blood and spares the patient buttresses that require future removal2,3. Finally a compressive dressing should be applied. This is best achieved by supporting the posterior aspect of the ear with gauze. Wrapping the head is a good way to keep the dressing in place.
Specialized thermoplastic splints were developed and can be formed to the ear. These do well in preventing re-accumulation, but can be expensive. In further researching this subject, we found that simply placing two to three absorbable mattress sutures along the involved portion of ear both prevents accumulation of blood and spares the patient buttresses that require future removal2,3. Finally a compressive dressing should be applied. This is best achieved by supporting the posterior aspect of the ear with gauze. Wrapping the head is a good way to keep the dressing in place.
So now you are set. By utilizing the three tenets described above, there is no longer reason to fear the ear.
Dressing should be placed both posterior and anterior to the ear as to maintain pressure
References
1. Greywoode J, Pribitkin E, Krein H. Management of Auricular Hematoma and the Cauliflower Ear. Facial Plast Surg. 2010;Vol 26;6:451-455.
2. Soham Roy, Lee P. Smith. A novel technique for treating auricular hematomas in mixed martial artists (ultimate fighters). Am J Otolaryngol. 2010 Jan-Feb;31(1):21-24.
3. Giles WC, Iverson KC, Kind JD, Hill FC, Woody EA, Bouknight AL. Incision and drainage followed by mattress suture repair of auricular hematoma. Laryngoscope. 2007 Dec;117(12):2097-9.
Drs. Christopher Johnston, Lina Tran and Erik Adler are 3rd and 4th year EM Residents at the Denver Health Emergency Medicine Residency Program. Dr. Peter Pryor is an Assistant Professor of EM at the University of Colorado School of Medicine.





5 Comments
I was born disabled. My in my life some doctor’s completed wrong surgeries on my body. The doctors never took responsibilities for their mistakes. The previous one was at a rehab home. I had an allergy to a pill and got a hematoma outside of my left ear. It took them forever to treat it and when they did they damaged my ear. Instead of drinig it they would use sharp tool and put gaz in it. I ended up having a plastic surgery.
Sadly, the hematoma is back. 🙁 Should I leave it alone or see my primary doctor?
Thanks in advance.
Hi, I also had my hematoma due to an infection not a traumatic blow to my head.
It was some of the worste pain ive ever experienced in my life . They also did what your the saying and it filled with blood 3x . Im sorrry I cant offer a better solution to treat this because like you they kept draining and finally they gave me stitches . I only wrote this because of the pain I went through and had to tell you to definitely go to the doctor. You can google good ENTs in your area . Im sorry for your pain and wish you the best.
I pray I did this correctly. Excuse me if you receive multiples.
I got this Ear Cauliflower on my right ear and i went to doctor after drainage he put pressure bandage on and gave me some medicines as well after 3 days i got again swelling on my ear but this time it is in small amount i have drained my ear 2 times from professional.
Kindly let me know either it is getting on a correct path or i need to change doctor or the pattern of medications.??
I’m a mother of wrestlers. We use flat magnets on either side of the ear to provide compression. You can buy various strength magnets at a craft store to find the right comfort/compression balance for you.
The other thing we have done is create custom molds of their ears before a hematoma occurs. One for the back of the ear and one for the front so that together they create a sort of clam shell compression splint. They can be secured with a headband and are comfortable enough to sleep in. The molds are made from dental impression putty comes in two canisters one is a base and the other is a catalyst. Check out EarSplintz on YouTube