 The resident comes to tell you that you have a transfer request holding on the phone. An outside ED physician has a child with left arm weakness. He feels that the child needs to see the Pediatric Neurologist at your institution. You agree to the transfer and await events.
The resident comes to tell you that you have a transfer request holding on the phone. An outside ED physician has a child with left arm weakness. He feels that the child needs to see the Pediatric Neurologist at your institution. You agree to the transfer and await events.

A rare complication of chronic sinusitis to watch for in the ED
It has been business as usual in the Pediatric ED. The volume has been steady but not overwhelming. The resident comes to tell you that you have a transfer request holding on the phone. An outside ED physician has a child with left arm weakness. He feels that the child needs to see the Pediatric Neurologist at your institution. You agree to the transfer and await events.
Soon the child has arrived. The resident has seen him and gives you her report. The patient is a 12 year-old boy. He has had about two weeks of URI symptoms. About five days ago the family noticed some swelling around his right eye. He also had some swelling on his right forehead that he thought was from bumping into a door. He went to see his Pediatrician who felt he had sinusitis and prescribed amoxicillin. He has had some fevers, which have continued despite the antibiotic. This morning when he woke up, his right eyelid was drooping. His left arm was weak and he was having trouble moving it. He went to the outside ED where he got a work-up and imaging. The Radiologist at the outside hospital read his CT as showing sinusitis and Potts puffy tumor. “So what is Potts puffy tumor and what needs to be done”, the resident wants to know. “Do we need to call Neurology?”
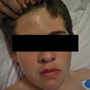
You go in to see the patient. He is awake and alert and fully cooperative. His vital signs and normal for age and he has no fever at this time although his mother reports that he had one this morning. He has a soft, tender swelling on his right-to-mid forehead and right ptosis with normal pupils and extra-ocular movements. He has tenderness over his frontal sinuses bilaterally and his maxillary sinus on the left. His nose has red and swollen turbinates with some thick rhinnorhea. The rest of his exam is unremarkable until you get to his extremities. His left arm is quite weak, extensors more than flexors. His grip strength is diminished. His sensation appears intact. The rest of his neurologic exam is normal.
You review his labs. The white count is elevated at 16.2 with a left shift. His CRP is elevated at 4.6 and his ESR is likewise elevated at 75. You request that the outside CT scan be submitted for review as you turn to answer the resident. Do you need a Neurology consult? No. Do you need a consult? Yes. Not Neurology, Neurosurgery.
So what is Potts puffy tumor? It is a subperiosteal abscess of the frontal bone that presents as frontal swelling. It is an uncommon complication of frontal sinusitis. It can also be seen after head trauma. It is usually but not invariably associated with frontal bone osteomyelitis. It was first described by Percivall Pott in 1768.
Potts puffy tumor is usually seen in late childhood and adolescence. It is rare before the age of 6 because the frontal sinuses do not pneumatize above the orbital ridges until that age and do not fully develop until late adolescence. It is much more common in teens than in adults, perhaps because children and adolescents get more frequent URIs, leading to more frequent frontal sinus disease.
Complications of Potts puffy tumor include preseptal and orbital cellulitis due to downward spread of infection and intracranial infection from posterior extention of infection. Organisms include streptococci, h. influenzae, anaerobes, staph aureus and enterocci.
Patients with Potts puffy tumor start with frontal sinusitis. They then develop scalp or periorbital swelling. It is typical to see red, tender, fluctuant swelling in the mid-forehead, as in our patient. They can have headache, fever and rhinnorrhea. With intra-cranial abscesses headache, focal neurologic deficits and signs of elevated intra-cranial pressure may be present. Intracranial abscesses have been observed in about 60% of patients with Potts puffy tumor.
A CT scan with contrast will show the sinusitis and is useful for planning surgery. MRI is helpful for identifying intracranial complications. The management is primarily surgery to drain abscesses and remove osteomyelitic bone. Broad spectrum antibiotics should also be administered.

This child’s CT shows opacification of both frontal sinuses, the left maxillary and ethmoid sinuses as well as swelling of the frontal subcutaneous tissue. He is admitted to Neurosurgery for antibiotics and operative management. His neurologic deficits improved during his hospitalization and in follow-up had almost completely resolved.

URIs are frequent causes of ED visits in children. Only about 0.5-2% of viral URIs in children will lead to bacterial sinusitis. Acute bacterial sinusitis can present at any age. Both the ethmoid and maxillary sinuses are present at birth. The sphenoids develop at age 5 and the frontal sinuses begin to develop at age 6-8 as described above. There are many conditions that predispose a child to acute bacterial sinusitis. These include URIs, allergic rhinitis, exposure to second hand smoke, immune deficiencies, cystic fibrosis, ciliary dysfunction, GE reflux, cleft palate, nasal polyps and nasal foreign bodies. The most common symptoms of sinusitis in children are nasal congestion with prurulent drainage, fever and cough. Less frequent symptoms include headache, facial pain, peri-orbital swelling, decreased smell, maxillary tooth pain and pain with bending forward. Acute bacterial sinusitis in the pediatric population is diagnosed by history. Patients either present with persistent cough and nasal discharge without improvement for more than 10-14 days or with high fever (39 or greater) and prurulent nasal drainage for 3-4 days in a row. Most acute sinus involvement from a URI is viral. It begins to improve in a few days and will resolve with no antibiotics. Chronic sinusitis is difficult to treat and controversial. The typical child will have 6-8 URIs per year and antibiotic therapy for the usually brief and self-limited associated sinus infection is discouraged in this era of increasing antibiotic resistance. There are no reliable incidence figures for Potts puffy tumor which is a rare complication of acute frontal sinusitis as well as head trauma. Just be aware of Potts puffy tumor as a rare but possible complication of acute bacterial sinusitis so that you can recognize it promptly and refer appropriately.
References:
- Kombogiorgas, D.,Solanki, G. The Pott puffy tumor revisited: neurosurgical implications of this unforgotten entity. J of Neurosurg:Peds 105(2):143-146, 2006.
- Durur-Subasi, I. et al. Potts Puffy Tumor: Multidetector Computed Tomography Findings. J of Craniofac Surg 19(6):1697-1699, 2008.
- Tsai, B. et al. Potts puffy tumor in children. Childs Nerv Syst 26:53-60, 2009.
- Karaman, E. et al. Potts Puffy Tumor. J of Craniofac Surg 19(6):1694-1697, 2008.
- Shehu, B., Mahmud, M. Potts puffy tumour: A case
report. Ann of Afr Med 7(3):138-140, 2008.
Amy Levine, MD, is an associate professor of pediatric emergency medicine at UNC Chapel Hill.




4 Comments
Im the person in the picture I’m glad to know really What happened, thank you
What is the connection with weakness in the left arm please?
My 3 yr old daughter’s forehead will swell from the ridge of her nose between her eyes up her forehead, if, I don’t continually give her allergy medicine during the winter season. It is very strange looking. I’m wondering if this is the same thing?
I have a problem like this . What i can do