A 21-year-old male bicyclist is brought to the ED, fully immobilized by EMS, after being struck by a car at moderate speed. The patient was found on the ground a few feet from the road with an obvious deformity to his right lower extremity (RLE). He reports that he was struck on the right side, which caused him to go over the handlebars. He was not wearing a helmet but he denies any headache or loss of consciousness. He states that his only significant pain is to his right leg. He has no significant past medical history except for the fact that he was assaulted two weeks prior and had jaw wiring at that time for a mandibular fracture.
Physical examination reveals a young adult male in moderate distress secondary to leg pain, with obvious shortening and deformity to the right femur. There is no evidence of trauma to the head, neck, chest, abdomen or upper back. The jaw is wired shut. Breath sounds are equal bilaterally and the cardiac exam is also normal. The abdomen is non-distended, non-tender and normal bowel sounds are heard. The pelvis is stable, but pain is elicited with gentle pelvic manipulation. The right leg has a notable deformity at the mid-thigh, with shortening and swelling, but no laceration. There are palpable dorsalis pedis and posterior tibial pulses, which are symmetric with the uninjured contralateral leg. The motor and sensory exam distal to the injury is normal bilaterally except as limited by pain. The GU exam is also normal.

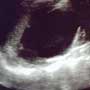
A FAST (Focused Assessment with Sonography in Trauma) exam is done during the initial evaluation. The left-upper-quadrant image is shown above. What are the notable findings? What additional imaging studies would you order on this patient or should he instead go straight to the OR?
click on image to enlarge
 Dx: Massive Hydronephrosis Causes False-Positive FAST Exam
Dx: Massive Hydronephrosis Causes False-Positive FAST Exam
The FAST exam done during the initial evaluation shows a large amount of anechoic fluid in the left upper quadrant (LUQ) in the area of the splenorenal space (fig. 2). The remainder of the FAST exam was normal. This fluid was later better delineated on CT scan to be due to hydronephrosis rather than due to trauma. The patient also had a chest X-ray that was unremarkable, and an X-ray of the right femur that revealed a mid-shaft femur fracture. He remained hemodynamically stable. CT scans preformed of the brain, cervical spine and chest were all normal. The abdomen/pelvis CT showed a comminuted pelvic fracture of the sacrum, a right inferior ramus fracture, and right L5 and S1 transverse process fractures. Also noted was severe left hydronephrosis extending down to the level of the bladder with severe renal cortical thinning (fig. 2). There was no intra-abdominal injury or free fluid noted. All laboratory results were unremarkable.
The patient was taken to the operating room and underwent an open reduction and internal fixation (ORIF) of his right femur. He was then transferred to a tertiary care facility for fixation of his pelvic fractures. At 3-week follow-up he was still admitted to the hospital and no further intervention was performed for his hydronephrosis.
This is a case of a patient with massive left hydronephrosis causing a false positive FAST exam. The hydronephrosis is localized to the upper pole of the left kidney, but because the renal cortex is so thin, it gives an appearance similar to a fluid collection at the splenorenal recess. Further testing showed that this patient had a duplicate collecting system in the left kidney, which was previously undiagnosed. The more superior system was obstructed causing hydronephrosis and hydroureter. This congenital abnormality is present in 0.2% of live births and has a 12% prevalence in first degree relatives. A duplicated urinary collecting system predisposes patients to obstruction, reflux and infection, though most remain asymptomatic.
Anechoic fluid detected on FAST exam, in the right clinical scenario, is suggestive for intra-abdominal bleeding. The FAST exam has become an integral part of the bedside assessment of patients with blunt or penetrating trauma. The results of this exam are often used to make critical decisions in patient management. At many institutions, a hemodynamically unstable patient with a positive FAST exam is taken to the OR for an immediate exploratory laparotomy. However, stable patients with a positive FAST exam can be usually be further evaluated with a computed tomography study.
The FAST exam is generally considered positive if there is detection of intraperitoneal fluid on any of the three abdominal windows (hepato-renal space, spleno-renal space or supra-pubic space) or if there is pericardial fluid detected on the cardiac window. However, not all anechoic collections represent a hemoperitoneum. Fluid-filled bowel, fluid-filled stomach, ascites, free urine from an intraperitoneal bladder rupture, perinephric fat pads, subcapsular hematomas, renal cysts and fluid-filled gallbladders have all been reported as etiologies that resulted in false positive FAST studies.
Relevant to this case, distinguishing hydronephrosis from free intraperitoneal fluid, it is important to remember that free fluid in the LUQ typically lies in a dependent location forming an anechoic strip at the tip of the spleen or more commonly, between the spleen and the diaphragm since the phrenicocolic ligament restricts the amount of fluid that can collect in the splenorenal space.
On review of the literature, hydronephrosis has not been previously reported as a cause of a false positive FAST exam. Undoubtedly, a skilled ultrasonographer would be able to diagnose this anechoic collection as severe hydronephrosis. A neophyte may have more difficulty. It is imperative for the emergency physician who is incorporating the FAST exam into their trauma assessment to be able to recognize this and other causes of false positive studies to prevent unnecessary laparotomies and thereby avoid increased morbidity and mortality.
References
- Kendall J, Ramos J. Fluid-Filled Bowel Mimicking Hemoperitoneum: A False-Positive Finding During Sonographic Evaluation for Trauma. J Emerg Med 2003; 25:79-88.
- Nagdev A, Racht, J. The Gastric Fluid Sign: An Unrecognized False-Positive Finding During Focused Assessment for Trauma Examinations. Am J Emerg Med 2008; 26:630.e5-630.e7.
- O. John MA, Kefer M. Ultrasound Detection of Free Intraperitoneal Fluid Associated with Heptaic and Splenic Injuries. So M
ed J 2001; 94:54-55. - O. John MA, Matter J, Blaivas M. Emergency Ultrasound. 2008: The McGraw-Hill Co.
- Scoutt L, Sawyers S, Bokhari J, Hamper U. Ultrasound Evaluation of The Acute Abdomen. Ultrasound Clin 2007:293-523.
- Sierzenski P, Schofer J, Bauman M, Nomura J. The FAST Double-Line Sign: A False Positive Finding on the Focused Assessment with Sonography for Trauma (FAST) Examination. J Emerg Med 2009; Oct 1.
- EMresource.org: http://www.erpocketbooks.com/er-ultrasounds/trauma-ultrasounds-from-the-ed/
Pearls & Pitfalls for Trauma Ultrasonography
1. Blood appears anechoic (black) when acute and free flowing, but hypoechoic (gray) when subacute or clotted. When blood is gray it is much easier to miss, especially if you are not looking for it. Blood in the pericardial space that is related to trauma is often hypoechoic (gray).
2. The sensitivity of ultrasound in trauma improves with Trendelenburg positioning, repeat imaging and if you know how and where to look (experience). Always image the inferior tip of the liver, as this area may be positive when Morrison’s pouch is not. Also, turn down the gain on the pelvic view if the bladder is full, otherwise the enhancement behind the bladder may “white out” a small pocket of fluid. The sensitivity is ~85% if done serially, but as low as 24% in some studies. Usually >200ml of fluid can be detected
3. The specificity of the FAST exam is about 95%. False positives may include fluid mimics such as the prostate, psoas, a perinephric fat pad, severe hydronephrosis, fluid filled bowel or stomach, or a large blood vessel. They may also include other causes of free fluid such as ascites, urine, physiologic fluid, and inflammatory fluid from infection, pancreatitis or ischemic bowel.
4. If you cannot see the heart at all on the parasternal view, consider a small anterior left sided pneumothorax until proven otherwise. The chest film usually will not be sensitive enough to pick this up. If the patient is going to the OR consider either going to chest CT first or placing an empiric chest tube if the patient remains unstable and must be rushed to surgery.
5. Ultrasound can also be used to evaluate directly for pneumothorax or hemothorax. For hemothorax use the curvilinear probe to image above the diaphragm for fluid. Ultrasound is more sensitive than x-ray as it can detect as little as 20ml of fluid. For pneumothorax, use the linear small-parts probe in the sagittal plain. If safe, elevate the head of the bed 60 degrees and scan 2-3 interspaces at the most anterior part of chest. Look for the absence of the normal lung sling & comet tail artifacts that move with respiration. Sensitivity has been reported at ~95%, which is better than chest x-ray. False positives include mainstem intubation, bleb, infiltrate, contusion, ARDS, atelectasis, adhesions, and pulmonary fibrosis
6. If you work in a trauma center and don’t have an ED dedicated bedside ultrasound machine yet, you should. Get together with the trauma surgeons and request the hospital buy one and put on a course to train or re-train your doctors.