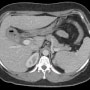
A 40-year-old Hispanic female presented to our Emergency Department complaining of upper abdominal pain, nausea and vomiting for 1 day. She denies fever; last bowel movement was the previous day. She has no history of prior abdominal surgeries and past medical history was unremarkable. Vital signs were normal except for tachycardia at 112 bpm.
On examination, the patient was in moderate distress, vomiting with abdominal tenderness upper quadrants. Laboratory studies including complete blood count with differential showed WBC 12.1 with 88.6% neutrophils, Liver Function Tests and Lipase were within normal limits. Computed Tomography of the abdomen showed free air within the gallbladder and “Gallstone ileus: perforated cholecystitis with an associated small bowel obstruction secondary to a 3.3 cm gallstone lodged within the ileum”.

With occurrence in less than 0.5% of patients, Gallstone ileus is an uncommon complication of cholelithiasis. The typical route of gallstone passage into the bowel lumen is through a biliary-enteric fistula, which results in mechanical obstruction in about 1 to 4 percent of cases [1]. More than half of these fistulas are between the gallbladder and the cholecystoduodenal but fistulas can also be formed between the gallbladder and the cholecytocolonic, as well as, the gallbladder and the cholecystogatric; all potentially resulting in gallstone ileus [2]. Once these gallstones enter the bowel lumen their most common sites of impaction are in the ileum, duodenum or colon. The least likely location for gallstone impaction is the proximal duodenum or pylorus. Gallstone impaction in this area ultimately leads to the development of a gastric outlet obstruction clinically termed Bouveret’s syndrome [3]. The Mirizzi syndrome refers to common hepatic duct obstruction secondary to extrinsic compression of the common bile duct by a large, impacted gallstone in the cystic duct [4]. A relationship linking the Mirizzi syndrome and the incidence of a cholecystoenteric fistula has been suggested, due to the chronic inflammatory process caused by the impacted gallstone in the cystic duct a complex fistula may form between the biliary tract and adjacent viscera [5].
The classic clinical presentation is an elderly female with intermittent obstruction. There are typically signs of abdominal pain, nausea and vomiting which may subside if the gallstone dislodges but may recur as the stone enlarges and impacts further down the bowel lumen. Diagnosis of gallstone ileus can be difficult and often is not made until during laparotomy in about half the cases. The most useful diagnostic tests are abdominal plain films and abdominal CT scans. Classic radiologic findings of gallstone ileus are: pneumobilia; partial or complete intestinal obstruction; change in position of a previously sited stone; direct visualization of a calcified stone and two adjacent small bowel air-fluid levels in the right upper quadrant.

The goal of treatment is to relieve intestinal obstruction following management of fluid and electrolytes. The surgical options are: a one-stage procedure which involves treating the gallstone obstruction with a cholecystectomy, and fistula division, with or without common bile duct exploration; or a two-stage procedure during which the obstruction is treated with enterolithotomy alone. The one –stage is contraindicated in patients with high operative risk factors, thus, the two-stage procedure is often the treatment of choice.
References
- Reisner RM, Cohen JR. Gallstone ileus: a review of 1001 reported cases. Am Surg 1994; 60:441-446.
- Van Hillo M, van der Viiet JA, Wiggers T, et al. Gallstone obstruction of the intestine: an analysis of ten patients and a review of the literature. Surgery 1987; 101:273.
- Kavuturu S, Parithivel V, Cosgrove J. Bouveret’s syndrome: A rare presentation of gallstone disease. OPIS 12 Scientist 2008; 2 (2): 25-26.
- Mirrizi, PL. Syndrome del conducto hepatico. J int de Chir 1948; 8:731-733
- Beltran MA, Csendes A, Cruces KS. The relationship of Mirizzi syndrome and cholecystoenteric fistula: validation of a modified classification. World J Surg 2008;32:2237
Dr. Elfond is Associate Director/Director of Academic Affairs, Department of Emergency Medicine, Nassau University Medical Center, East Meadow, NY. Dr. Alagoa is the Research Director, Department of Emergency Medicine, Nassau University Medical Center, East Meadow, NY.