Mobile stroke units reduce the time to treatment, but are we measuring treatment efficacy correctly?
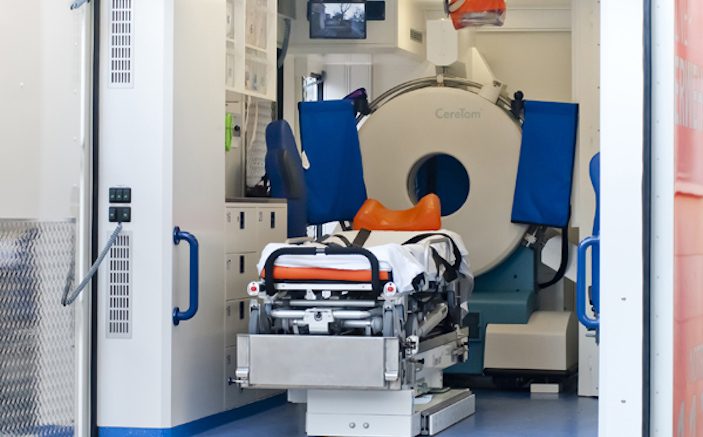
At the 2016 ACEP Scientific Assembly there was an exhibit of an ambulance that contained a head CT unit. The idea is to send the unit with appropriate staff to identify and treat stroke patients in the field based on prehospital triage guidelines.
Fascinating concept. But how would it work in reality? In an article in the Chicago Tribune dated October 20, 2016, initial use of the mobile CT units at two Chicago area hospitals is described. The article notes that the units cost about $1 million each (other articles cite acquisition costs at $500,000 – $600,000) and a spokesman for one of the two hospitals said it would cost between $950,000 and $1.2 million annually to operate each unit (and that’s with the program operating only 12 hours a day).
The plan would have the 911 dispatcher ascertain the symptoms of the patient and, if certain criteria were met (and perhaps on consultation with a physician), the stroke ambulance would be dispatched along with a regular paramedic ambulance. Clearly a highly skilled clinician would need to be involved on scene (even if telemedicine consultation with a stroke neurologist exists) to ascertain the status of the patient because if a stroke is suspected and the CT doesn’t show a bleed, the idea is to give thrombolytic therapy on site. Keep in mind that about 10% or more of strokes are really stroke mimics and that many of these stroke mimics may get thrombolytics unnecessarily if the clinician on site or via telemetry is not astute.
The whole idea behind the project is to save time and direct the patient to the appropriate hospital. That’s where the rubber hits the road. According to the article, doctors at the two hospitals believe that “the mobile units could make huge differences in stroke patients’ recoveries by allowing treatment to start earlier.” However, the data to support that assertion is less than robust: In the original NINDS study, thrombolytic treatment of a stroke resulted in 12% of the patients improving and 6% worsening – with most patients receiving no benefit, and only a fraction of patients meet criteria to receive thrombolytic therapy.
Another article on mobile CT stroke programs (Modern Healthcare, January 4, 2016) indicated that patients received thrombolytic therapy 42 minutes faster compared with standard care (64 minutes vs 104 minutes) based on preliminary data from the Cleveland Clinic and a University of Texas, Houston, program. A large German study of 6,182 patients found only a 15-minute reduction in time to thrombolytic therapy (61 minutes vs 76 minutes) and as anticipated with this small change, there were no differences in secondary outcomes including death. In this study, where times to treatment in the ED are already excellent, little if any improvement can be expected with a mobile CT stroke program. So, the better the ED at quickly assessing and giving thrombolytic therapy the smaller the advantage (if any) that can be expected for a mobile CT stroke program. Let’s look at the study.
EFFECT OF THE USE OF AMBULANCE-BASED THROMBOLYSIS ON TIME TO THROMBOLYSIS IN ACUTE ISCHEMIC STROKE: A RANDOMIZED CLINICAL TRIAL
Ebinger, M., et al, JAMA 311(16):1622, April 23-30, 2014
BACKGROUND: Recent data suggest that door-to-needle treatment time for thrombolytic therapy in stroke patients in the USA may be less than the recommended 60 minutes for only 30% of patients.
METHODS: In the “Prehospital Acute Neurological Treatment and Optimization of Medical Care in Stroke” study (PHANTOM-S) from Germany, 6,182 adult stroke patients received prehospital care from a specialized stroke emergency mobile (STEMO) unit equipped with a CT scanner and a point-of-care lab and staffed by a neurologist-led team, or standard transport to a hospital with a stroke unit. Thrombolytic therapy was initiated in the prehospital setting for eligible patients transported by the STEMO unit. The primary outcome was the time from initiation of stroke dispatch to thrombolysis.
RESULTS: The STEMO unit could not be deployed during the intervention weeks for 44% of qualified patients. Rates of tPA treatment for ischemic stroke were 32.6% with STEMO deployment and 29.0% during STEMO intervention weeks vs. 21.1% during control weeks. The corresponding percentages of patients treated within 90 minutes of symptom onset were 58% and 48% vs. 37%. During the intervention weeks, there was a 15-minute reduction in time to thrombolytic treatment (76.3 min vs. 61.4 min during control weeks). There was no significant difference between the groups in secondary outcomes that included rates of intracerebral bleeding after thrombolytic therapy or inpatient mortality.
CONCLUSIONS: Delivery of prehospital thrombolytic therapy for ischemic stroke by a highly specialized unit reduced the interval to treatment without increasing adverse outcomes.
24 references (martin.ebinger@charite.de – no reprints). Copyright 2014 by Emergency Medical Abstracts – All Rights Reserved 10/14 – #7
Seems like the idea of mobile CT stroke units is catching on in the U.S. with about 20 programs either up and running or online. But can it be demonstrated that these programs make a difference?
The theoretical advantage behind prehospital mobile CT programs is that faster treatment results in better outcomes. Makes sense. But what does the literature show? Here’s a study that fundamentally challenges the concept – and it demonstrates a common statistical trap. Because the study involved so many patients, very slight differences in outcomes (in hospital mortality, OR 0.96; independent ambulation at discharge, OR 1.04 and discharge to home, OR 1.03) become statistically significant when, in reality, the differences for individual patients are likely nominal. As the study authors also note, correlation does not equal causation and perhaps patients treated earliest had the better outcome because they were more likely to have TIAs and therefore recovery would have occurred independent of treatment.
TIME TO TREATMENT WITH INTRAVENOUS TISSUE PLASMINOGEN ACTIVATOR AND OUTCOME FROM ACUTE ISCHEMIC STROKE
Saver, J.L., et al, JAMA 309(23):2480, June 19, 2013
BACKGROUND: Despite a paucity of evidence, advocates of thrombolysis in acute ischemic stroke (AIS) have asserted that earlier treatment leads to improved outcome.
METHODS: These multicentered authors, coordinated at UCLA, examined the association between time to treatment and outcome in 58,353 AIS patients (median age, 72) who were treated with IV tPA within 4.5 hours of symptom onset in 1,395 hospitals in 2003-2012 and were included in the “Get With The Guidelines Stroke” registry.
RESULTS: The interval from symptom onset to treatment was 0-90 minutes in 9.3% of the patients, 91-180 minutes in 77.2% and 181-270 minutes in 13.6%. There was a statistical relationship between earlier treatment and slightly more favorable outcomes, with in-hospital mortality in 7.7% in the earliest treatment group vs. 8.7% in the intermediate group (adjusted odds ratio [aOR] 0.86). Contrary to this hypothesis, mortality was intermediate (8.0%) in the latest treatment group (aOR 0.74). The rate of tPA complications and symptomatic ICH were also slightly better in the group treated earliest.
CONCLUSIONS: The authors suggest the association between earliest treatment with IV tPA and (some) slightly better outcomes implies that earlier treatment is desirable. An association does not apply causation, however, and a more obvious explanation is that the number of “stroke” patients in fact having a TIA is greatest shortly after the onset of symptoms, but diminishes regularly with the passage of time. Thus the number who improve “after tPA” in truth simply because they were actually having a TIA should decrease in a regular fashion with the passage of time, completely independent of “treatment.”
31 references (jsaver@mednet.ucla.edu – no reprints). Copyright 2014 by Emergency Medical Abstracts – All Rights Reserved 2/14 – #9
My conclusion: Mobile CT stroke programs seem pretty nutty. The expense is very substantial both in acquisition and staffing, only a small fraction of stroke patients are likely to receive treatment from the mobile CT stroke units, and a surrogate marker of efficacy (time to treatment) is used as a measure of success (rather than meaningful clinical outcomes).
The most effective way to speed time to treatment for acute ischemic stroke patients is to refine ED systems so that door-to-needle times are very short in all EDs. This allows many more stroke patients to get any benefit there may be from early treatment rather than just a very select few being treated at a huge cost.
But that’s just one person’s opinion.