When is it appropriate to bypass a stone-protocol CT scan in a young person?
“Hey Eran, thanks for calling me back so quickly. I want to tell you about my 13-year-old female patient who has a 5 mm right-sided uretero-pelvic junction (UPJ) stone noted on point-of-care ultrasound (Figure 1 below). She experienced the sudden onset of severe right flank pain about three hours ago. Her UA was positive for microscopic hematuria without pyuria, and she has a normal CBC and CRP, a negative urine pregnancy test, and a BUN and Creatinine of 12 (mg/dl) and 0.6 (mg/dl), respectively. She has modest right hydronephrosis (Figure 2 below), but I also noted ipsilateral ureteral jets (Figure 3 below). I did not notice any other stones while scanning from her kidney through bladder. So, I believe she has a solitary UPJ stone without complete obstruction. I know your preference is a stone-protocol non-contrast CT (NCCT). But the patient’s mother, who is an internal medicine physician, would like to avoid CT if at all possible. She suspects her daughter will be just like her husband, who experienced kidney stones as a child, continues to be a frequent stone-former, and is known to have elevated urinary calcium levels. She is also aware that our adult hospital scanner may impart more radiation than the one downtown at the Children’s Hospital and would prefer to wait for more information prior to agreeing to CT. The patient’s pain has now been well-controlled for almost two hours after 75 micrograms of fentanyl and one-half milligram per kilogram of ketorolac, and she is also tolerating PO fluids. Her Mom would prefer to take her home and use oral pain medication as needed. I think it’s likely she’ll spontaneously pass this moderate-size stone and prove to be a biochemical stone-former. I’d like to have them contact your office tomorrow to arrange a follow-up appointment.”

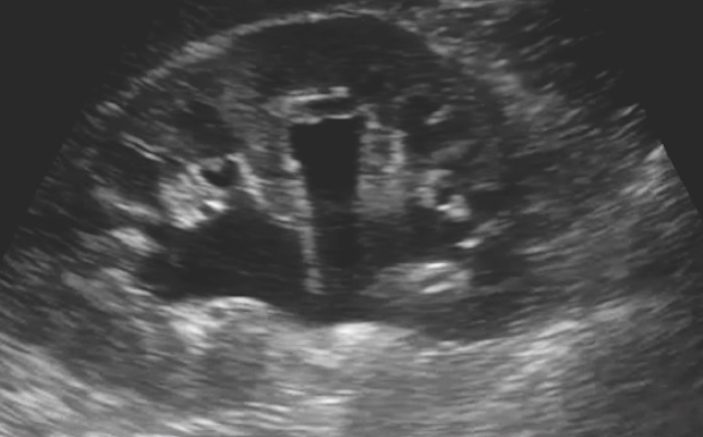
Figure 1. Moderate hydronephrosis associated with posterior acoustic shadowing (arrows) suggesting a stone (designated by arrowhead). This image illustrates the utility of additional associated ultrasound findings in confirming the presence of a stone.

Figure 2. Hydronephrosis. The arrow denotes a moderately dilated renal pelvis.

Figure 3. Right ureteral jet via Color Doppler.
“Dave, you know about the stone-protocol CT. It really isn’t that much radiation.”
“Eran. I understand and expressed this to her Mom. But the millisievert dose we deliver here is still higher than what the new scanner that Children’s provides. Also, the technicians at the Children’s Hospital are more accustomed to reducing the radiation dose proportionate to patient size. Given her young age, she may well experience additional stones in the future. Some of those situations could be more complicated with greater need for CT. Given her daughter’s young age, her mother is concerned about cumulative radiation risk. She fully expected this to be a stone but brought her in so that we could address her pain.”
“Dave. I like to demonstrate that there are no other co-existing significant problems and normal anatomy. There may be other stones too small to see on your ultrasound but visible on CT. I’ve had a few cases that I expected to be simple and were not.
“Eran, that is a perfectly reasonable concern. However, her high likelihood of a stone suggests a very low probability of alternative diagnoses. Also, stones that are too small to see on ultrasound almost always pass spontaneously. Her mother has said she will strain her urine at home and hopes to arrive in your office with ‘stone in cup.’ If it doesn’t go this way, you can get an outpatient non-contrast CT (NCCT).”
“Alright Dave. Straining the urine will be extremely important in both confirming the diagnosis and evaluating for a metabolic etiology. Also, I’d like you to add a plain KUB. Bowel gas can make sonographic visualization difficult between the ureteropelvic and ureterovesicular junctions; we may need to follow the stone if it doesn’t pass reasonably soon.”
“OK. Thanks Eran.”
*****
In the specific scenario that inspired this case, the patient did, indeed, demonstrate a markedly elevated 24-hour urinary calcium excretion while a small stone passed spontaneously within a few days. Stone analysis confirmed calcium oxalate composition. Follow up, utilizing both consultative ultrasound and plain KUB, demonstrated no visible stones. The child did well with only two stone recurrences during the subsequent five years.
The conundrum we face with pediatric kidney stones is the frequency of occurrences over time. Many children undergo repetitive CT scans despite little evidence for improved outcomes. Conversely, relatively few children with suspected urolithiasis are evaluated with ultrasound despite professional guidelines suggesting its use.

Figure 4. Plain KUB radiograph demonstrating right UPJ stone (arrow).

Figure 5. Twinkle artifact highly specific for urolithiasis.
Pearls / Pitfalls: Scanning for Nephrolithiasis in Children
- Although nephrolithiasis in children occurs less often than in adults, the incidence is rising rapidly. Risk factors include the increasing prevalence of pediatric obesity and the ubiquitous use of high-salt diets. Nephrolithiasis beginning in childhood may be a recurring (up to 50% within three years) and life-long problem necessitating numerous evaluations. A clinical strategy that anticipates repeated inquiries is essential.
- There is little doubt that CT provides the greatest accuracy among the various imaging modalities used in the evaluation of renal colic suspicious for nephrolithiasis. Low dose non-contrast computed tomography (NCCT) provides high test sensitivity and specificity.
- Paradoxically, it appears that the 10-fold increase in CT use for suspected urolithiasis that occurred between 1996 and 2007 failed to improve outcomes [1]. Persons with a high clinical probability of stones seldom have emergent co-morbid conditions, while most stones pass spontaneously and quickly, confirming the diagnosis. As a result, greater selectivity in the use of CT has been advocated.
- The dose of radiation to which a given child may be exposed during CT evaluation for a suspected stone may vary among health-care facilities. CT-associated radiation exposure in a study of patients treated in dedicated Children’s versus non-dedicated Children’s facilities was significantly higher in the latter [2]. The authors recommend pediatric-specific calibration of non-children’s hospital CT units or consideration of transfer to a children’s-specific facility with experience in the use of lower radiation doses.
- Until ongoing epidemiologic studies provide additional confirmation of low risk, we believe that radiation exposure should continue to be minimized whenever possible. A staged approach combining lab testing, urine analysis, and ultrasound may provide an adequate initial assessment for children with suspected nephrolithiasis. If ultrasound detects a stone likely to pass spontaneously, then expectant management with pain medication and a urine strainer may be reasonable, as was the case for our patient. If ultrasound is inconclusive for the presence of a stone, CT may be used. This is reminiscent of the “ultrasound-first” staged protocol recommended for use in suspected pediatric appendicitis.
- Although user-dependent, ultrasound has demonstrated accuracy in identifying stones in the renal pelvis, proximal and distal ureters and bladder. Its utility is enhanced in patients who are well-hydrated; hence the recommendation for intravenous fluid prior to scanning. Since most stones are comprised of either calcium oxalate or calcium phosphate, the addition of a KUB radiograph to the screening panel may identify mid-ureteric stones difficult to visualize with ultrasound due to overlying bowel gas (Figure 4).
- Ultrasound strategies are important. The discovery of hydronephrosis provides indirect evidence for a stone when noted in the appropriate clinical context. Hydronephrosis does not, however, mandate immediate intervention as the evidence supports the notion that it does not lead to irreversible loss of kidney function if corrected within a few weeks [3]. In situations where differentiation between hyperechoic artifact and stone is difficult, the detection of post-stone shadowing suggests the latter (Figure 1). Color doppler detection of twinkling phenomenon provides additional confirmation for a stone that is highly specific (Figure 5).
- If a small or moderate-sized stone is visualized during ultrasound and/or plain radiography, renal function is acceptable, oral hydration is successful, and patient comfort is maintained, then home management without immediate CT is reasonable as the majority of stones will pass spontaneously. Subsequent 24-hour urine and stone analysis may provide support for a metabolic etiology. Retrieval of a stone during post-discharge straining of the urine may occur and further contends against the need for an emergent CT to define the cause of renal colic.
- It is important to note that many urologists prefer a NCCT to ultrasound for the first episode of apparent renal colic. NCCT provides slightly higher sensitivity for the identification of alternative causes for presenting symptoms. An initial CT also allows, as does ultrasound, for reasonably accurate assessments of stone size, shape and location and, therefore, can be used to predict likelihood of spontaneous passage.
- What are other indications for a CT? (1) It can be utilized within a staged approach for the evaluation of apparent renal colic when a stone is not confidently identified using ultrasound and plain KUB, (2) when concern exists regarding alternative and/or high-acuity conditions such as malignancy or stone-associated urosepsis, (3) in complex cases characterized by symptoms such as uncontrolled pain or vomiting, and (4) when requested by a urologist for precise localization in anticipation of a stone-removal procedure.
REFERENCES
- Westphalen AC, Hsia RY, Maselli JH, et al. Radiological imaging of patients with suspected urinary tract stones: national trends, diagnoses and predictors. Acad Emerg Med 2014;32:367-370.
- Ronckers CM, Doody MM, Lonstein JE, Stovall M, Land CE. Multiple diagnostic X- rays for spine deformities and risk of breast cancer. Cancer Epidemiol Biomarkers Prev 2008;17:605-613.
- Flint-Richter P, Sadetzki S. Genetic predisposition for the development of radiation –associated meningioma: an epidemiological study. The Lancet Oncology 2007:8(5)403-410.
- Vaiserman AM. Radiation homeostasis: historical perspectives and implications for low-dose cancer risk assessment. Dose-Response ;8(2):172-191.
- Spielmann AL, Heneghan JP, Lee LJ, et al. Decreasing the radiation dose for renal stone CT: a feasibility study of single- and multidetector CT. AJR Am J Roentgenol. 2002;178:1058-1062.
- Pain V. Pathophysiology of urinary tract obstruction. In: Campell-Walsh Urology. Vol 2. 9th ed. Saunders;2007:1227-1273.








1 Comment
Nice review.
Where can I get a list of your references??