“I’ll bet you a package of chocolate covered raisins that she has an anion gap acidosis.”
Your intern overhears your bet with the nurse and looks at you with an expression of puzzlement. “Doc, what does that patient have? How do you know that she has an anion gap acidosis by looking at her?” he asks. “She hasn’t even been roomed yet!” You encourage him to go see the patient himself and come up with his own differential.
The patient arrived via EMS and you had the chance to do a “quick look” at her in triage. She is 19 years-old and called 911 because she has been having nausea, vomiting, and severe abdominal pain for the past two days. On arrival, EMS found her curled up into a ball on her couch, groaning in pain. She is tachycardic, hypotensive, and tachypneic, with a normal oxygen saturation and temperature.
“Everything hurts. Can’t you please give me something for the pain?!” she cries as your intern starts asking her some historical questions. The nurses are putting in her peripheral IV and drawing a rainbow of blood tubes, as he continues to ask her about the onset and quality of her symptoms, if her pain radiates, what the severity of her symptoms are, etc. His question, “Does your pain radiate anywhere?” is met with forceful heaving and non-bilious, non-bloody emesis all over the bed.
With great resolve, your intern ignores the specks of vomit he just got splattered with and continues to examine the patient. You whisper to the nurse to give the patient a 2L bolus of normal saline, 4 mg of IV odansetron, and 50 mcg of IV fentanyl, as you leave the room so your intern can work his magic independently.
A short while later, your intern emerges. “Aha! Now I know how you knew she had an anion gap acidosis!” your intern exclaims as he walks confidently out of the room. “Her sugars are over 500 mg/dL on the accucheck.” You smile, but shake your head. “No, we didn’t know what her sugars where when she arrived. Before she puked on you, what did you smell?” You explain to your intern that you could smell the fruity, sweet odor of DKA as she rolled through the door. “There are some truly distinct smells in emergency medicine that you will learn to recognize and appreciate after years of exposure. DKA, pseudomonas, melena, and the telltale smell of a urinary tract infection, to name a few.”
“Now let’s go ultrasound her abdomen.” Your intern gives you the same look of confusion asearlier, but dutifully goes and grabs the ultrasound machine.
Systematically, you start scanning through the patient’s abdomen and pelvis. You note that her IVC is thin and has almost complete collapse with inspiration. Her heart is hyperdynamic but otherwise grossly normal. You have your nurse ensure she gets a full 30 mL/kg bolus of IVFs and teach your intern to perform serial exams of her IVC during the resuscitation. As you move through your differential for abdominal pain in your head, you take a peek at the patient’s lower abdomen and pelvis with bedside ultrasound.
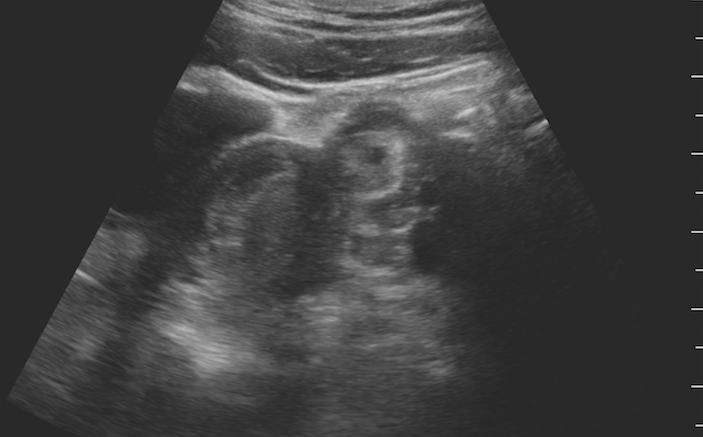
What do you see in images 1 (top of screen) and 2 below? What are your next steps in management?

“What? Really?! She has DKA and also has an ectopic pregnancy?” your intern exclaims as you pan through the patient’s left adnexa. You talk the team and patient through what you see on point-of-care ultrasound of her pelvis. She has a nice, clean, and normal bright white endometrial stripe in her uterus, and just to the right of it on the image (which is the patient’s left), you can see a circular adnexal mass. Within the mass, there is a dark, black circular gestational sac, with a bright white, hyperechoic fetus with a visible heartbeat (Image 3 below).

Your intern gives the patient the news, obtains a comprehensive gynecologic history, performs a pelvic exam, and consults OB immediately. On review, the patient has always had irregular periods, and of course, didn’t know she was pregnant. He finishes off the point-of-care scan by looking at her hepatorenal juncture. Luckily, it doesn’t appear as if she has ruptured and there is no free fluid in her right upper quadrant or pelvis just yet.
As your intern is cleaning up the machine, he stops you, “Ok, I get how you knew she had DKA by smelling the ketones on her breath, but how in the world did you know she had an ectopic pregnancy?”
With a nod and a smile, you advise him, “I really didn’t know about the ectopic and I actually didn’t even have a hunch it would be there before we started scanning. I was relying on the art of medicine to diagnose her DKA based on my initial whiff at triage. My dedication to the systematic science of practice is what made me perform an ultrasound of her abdomen.”
“We didn’t stop just because we had a diagnosis to explain her symptoms. We systematically went through our differential, which probably saved this young woman’s life.”
You grab your chocolate covered raisins, and wheel the ultrasound machine back to the charging station, marveling in the joy of practicing emergency medicine. A joy and thrill of discovery that you hope keeps you in the game for many years to come.
Pearls / Pitfalls
- Point-of-care ultrasound (POCUS) can be used to evaluate and assess a myriad of patient complaints and provide useful data in the assessment of almost any patient arriving to the emergency department.
- Females with abdominal complaints can be diagnostically challenging because of the various organs that could be causing their symptoms. Use bedside ultrasound to augment your clinical findings and to help expedite care.
- Point-of-care ultrasound can be performed at the patient’s bedside and information can be obtained quickly and accurately without exposing the patient to ionizing radiation.
- In patients who are receiving IV fluids, it is often helpful to know what their IVC looks like before and after fluid administration. Perform serial IVC scans to see if the patient is retaining the IV fluid intravascularly and to gauge how the resuscitation is progressing. [Add another sentence about what to look for with serial IVC exams]
- In patients of childbearing age with a functional uterus and ovaries, it is helpful to perform a point-of-care ultrasound of their pelvis if they have a complaint of pelvic or abdominal pain.
- Perform a transabdominal ultrasound of the pelvis and assess the uterus for the presence or absence of an intrauterine pregnancy. A low frequency curvilinear probe works best for evaluating the pelvic organs from a transabdominal approach.
- Perform the scan when the patient has a full or partially full bladder. Urine serves as a great acoustic window to enhance visualization of the structures deeper in the pelvis.
- In many instances, it is possible to positively identify an adnexal mass or ectopic pregnancy on transabdominal approach alone. With the newer, higher-resolution ultrasound machines, we can often visualize the ectopic gestational sac and fetus with cardiac motion on a transabdominal scan.
- If a patient is pregnant and you do not clearly see an ectopic pregnancy on transabdominal imaging, perform a transvaginal scan or order a comprehensive study through the radiology department. Remember that you should never send unstable patients to radiology. Have the sonographer come perform the scan at the patient’s bedside in the ED.
- Stay up to date on how you can use bedside ultrasound to enhance your clinical practice and improve patient care. Check out the ultrasound app “SonoSupport” available now for smartphones and tablets.









1 Comment
so true expirience the other EM textbook