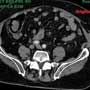
An 82-year-old man presented to the ED with abdominal pain. While walking in his yard he had fallen onto a two-inch-diameter piece of steel rebar. EMS reported seeing a locally expanding area while the patient was being prepared for transport. He had no history of surgery or swelling in the affected region.
On examination the patient was normotensive without signs of shock. He had a small abrasion on his head but did not lose consciousness, showed no altered mental status, and did not have a headache or focal neurological signs. His abdomen revealed a well-circumscribed area where the rebar impacted, with an abrasion extending inferiorly. His abdomen was soft, tender only over the abrasion, with no rebound or guarding or abnormal bowel sounds. There were no other positive exam findings.
Labwork, including CBC and creatinine, was normal. An abdominal CT with contrast showed a left lateral abdominal wall hernia. The hernia had a four-centimeter neck and contained colon without findings of obstruction, perforation, or significant hematoma.
The patient was referred to the trauma service and underwent an urgent abdominal exploration and repair of the traumatic hernia. A small serosal hematoma was discovered on the descending colon, which was unroofed and then repaired after showing no evidence of a full thickness injury. The hernia was reduced and the abdominal wall defect was repaired without mesh.
The patient developed a post-operative ileus and paroxysmal atrial fibrillation but was discharged home in stable condition twelve days later.




Dx: Traumatic Abdominal Wall Hernias
Traumatic abdominal wall hernias (TAWH) are related to blunt trauma and, although rare, are increasingly identified with the more frequent use of CT scanners. The cases described in the literature are diverse. Most of the adult literature involves motor vehicle or motorcycle accidents and most pediatric cases relate to handlebar injuries. The majority of the hernias in the literature are either lumbar or anterior wall hernias. The transmitted forces from blunt trauma increase intra-abdominal pressure, and the hernia that forms is at an anatomical weak point, not always at the site of impact.

When seeing blunt trauma patients with mechanisms such as motor vehicle crashes, handlebar injuries, falls onto small objects, or any trauma that increases intra-abdominal pressure, emergency physicians should look for TAWH.
Signs and symptoms of TAWH are relatively nonspecific and may be easily missed during a trauma evaluation. Increasing abdominal pain during an observational period and even a relatively small area of ecchymosis can be the only findings with these hernias. In this case, there was obvious clinical evidence of a growing hernia reported by EMS along with significant point tenderness over the ecchymosis.
While the physical exam can offer clues to the diagnosis, a CT scan or laparotomy will confirm the diagnosis and rule out hemorrhage or other associated pathology. A contrast CT scan of the abdomen is the diagnostic modality of choice in stable patients due to its noninvasiveness and its relatively high sensitivity. Ultrasound is another possible diagnostic modality easily utilized in the ED and can be diagnostic in experienced hands. Unstable patients with findings indicating TAWH should proceed directly to the operating room (see inset).
When TAWH are identified, look for associated injuries such as hollow viscus, solid organ and bony injuries – especially to the lumbar spine – and diaphragmatic injury or rupture. This is particularly true with high-energy TAWH where these injuries more commonly coexist, but even a relatively low impact mechanism causing TAWH can cause secondary injuries. Strangulated hernias are not typically an immediate concern in trauma but can develop later.
Disposition is admission and evaluation by a trauma surgeon; however, the treatment for traumatic hernias is controversial among them. Because TAWH and other intra-abdominal injuries commonly occur together, many sources say that an immediate exploratory laparotomy is mandatory. Others contend that more conservative action is appropriate, depending on the mechanism and manner of diagnosis. For example, in a study of 34 patients with TAWH by Netto et al. (2006), only half of hernias diagnosed by CT scan alone (24) had additional findings that required urgent surgery. However, the researchers also found that 70% of hernias evident during physical examination and 100% of anterior hernias were associated with other serious injuries. For these reasons, urgent laparotomy is widely accepted as the standard of care.
In summary, emergency physicians should consider the mechanism of injury and look for signs of TAWH during physical examination, using computed tomography or ultrasonography when appropriate. When a TAWH is identified, a thorough search for associated traumatic injuries should be made and early surgical consultation should be obtained.
Findings for which urgent laparotomy should be considered due to high incidence of associated injuries:
1. Restrained motor vehicle crash victims, especially back seat passengers with TAWH
2. Clinically apparent hernias
3. Anterior hernias
Summarized from 3Netto FA, Hamilton P, Rizoli SB, Nascimento B Jr, Brenneman FD, Tien H, Tremblay LN. Traumatic abdominal wall hernia: epidemiology and clinical implications. J Trauma. 2006 Nov;61(5):1058-61