What can bedside ultrasound reveal about this 22-year-old’s mysterious lower chest pain?
A 22-year-old G4P2 female is brought to the emergency department by her boyfriend for pleuritic right sided lower chest pain that she has had for approximately 18 hours. The pain is in the low anterior right side of the chest and radiates to the scapula and upper abdomen. It has been constant, but is not associated with nausea, vomiting, fever, chills, diarrhea or shortness of breath. Initially she was able to obtain partial relief with ibuprofen, but now it is not helping at all. She also denies any missed periods, bleeding, discharge or dysuria. She has been with her current partner for about 8 weeks and uses condoms for contraception, but is also on “the pill.”
On exam she appears to be in mild distress and has normal vital signs. Pertinent findings are splinting during maximal inspiration and right-upper quadrant abdominal tenderness. Pertinent negatives are anicteric sclera, clear lungs and lack of tenderness elsewhere on her abdomen and back.
Since the presentation is not really “textbook” for anything and you are worried she may have a pulmonary issue going on, you decide to do your best to avoid unnecessary advanced imaging by starting with a CBC, CMP, lipase, serum beta HCG, D-dimer, UA and a chest x-ray. After confirming that the boyfriend is driving home and they are not going by bus, you also order your favorite opiate to keep her comfortable while waiting for results.
Unfortunately or fortunately, the chest x-ray and all the labs are normal except for the D-dimer, which is elevated at 2000 (normal <250). Based on the high D-dimer, PE jumps to the top of your differential diagnosis, though you find it odd when you confirm she did not have a PE with any of her prior pregnancies, including two that went to term. You decide that since she is young and the chest x-ray is negative and you are not worried about an aortic dissection or an occult pneumonia that a V/Q scan is preferred over a CT. After all, a V/Q scan exposes the patient to a fraction of the radiation of a CT angio and there is no contrast dye involved.
Unfortunately for you (but fortunately for the patient), the V/Q scan is normal and after three and a half hours in the ED, you still have no diagnosis. Is it possible that this could be an atypical presentation for a gallstone? Eighteen hours of continuous pain with normal LFTs suggests otherwise. But rather than risk spending two more hours and who knows how much money on a formal ultrasound from radiology, you decide to take a look yourself first to see if it is really necessary.
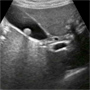
The image at right graces your screen. What does it show? Is this what you expected to find? Does this ultrasound image make sense with the presentation?
Is this image what you expected?

Dx: Is the Gallstone the Cause of Pain?
There is definitely a gallstone present in her gallbladder, but is it the cause of her pain? Simple biliary colic should only last a few hours. The general consensus is that any pain lasting more than six hours that is biliary in nature is cholecystitis until proven otherwise. So does this ultrasound demonstrate evidence of cholecystitis? The simple answer is no. There is no thickened wall, no dilated common bile duct and no pericholecystic fluid. The normal anterior gallbladder wall is less than 3mm thick; this one is about 1mm (estimation – not measured). The normal common bile duct is less than 4mm measured from inside wall to inside wall and this one is about 1-2mm (estimation). It is the dark line just below the gallbladder with hyperechoic walls. Pericholecystic fluid would appear as a dark fluid rim just outside the hyperechoic gallbladder wall. Considering the question of whether this patient’s pain represents atypical biliary colic, this gallstone is not impacted in the neck of the gallbladder. Rather it is mobile in the midportion of the gallbladder, where it is more likely to represent an incidental finding rather than the cause of acute pain. This ultrasound is consistent with an attack of biliary colic that has already resolved or with an incidental gallstone, but not with 18 hours of ongoing RUQ pain. There must be something else going on here. Could this be Fitz-Hugh-Curtis syndrome, with subdiaphragmatic irritation causing this patient’s prolonged pain?

Before pitching this case to GYN you perform a HIDA scan, which is more definitive for cholecystitis than an ultrasound, and perform a pelvic exam. The HIDA is, as suspected, normal but the pelvic is also non-diagnostic. While there was a minimal discharge, there was no cervical motion tenderness. Her gynecologist agrees that she should be treated empirically for STDs noting that she will follow her up, but is still doubtful that this is true Fitz-Hugh-Curtis syndrome since she lacks true pelvic pain.
A week later her gynecologist calls you to let you know that the chlamydia test came back positive and the patient is feeling much better and is off all pain medications. Does she now think this was Fitz-Hugh-Curtis? Reluctantly she agrees and compliments you on your good pick up.

Tips & tricks for Gallbladder & RUQ Ultrasound
01 Know your limitations: Ultrasound may help clarify findings elicited by a thorough history and physical exam. When used correctly, it can greatly improve diagnostic accuracy, and help guide patient management, especially for time-critical diagnoses and treatment of unstable patients. It can also decrease the use of CT scan and thereby minimize radiation exposure. If you use ultrasound in your ED, you need to consider your skill level and know your limitations. When unsure, order a formal study. If your department has an ED dedicated ultrasound machine, it should consider implementing a quality improvement program that is approved by both ED administration and radiology.
02 The Sonographic Murphy’s Sign: To check for a sonographic Murphy’s sign, which is a sign of cholecystitis, place the ultrasound probe at the maximal point of tenderness in the right upper quadrant. If the probe is placing direct pressure on the gallbladder fundus, you have a positive sonographic Murphy’s sign. False negatives may occasionally occur if the patient has received opiates prior to examination.
03 The Gallbladder Wall: One sign of cholecystitis is a thickened gall-bladder wall. The normal gallbladder wall can be up to 3mm thick. The most common conditions other than cholecystitis that may cause thickening of the gallbladder wall include hepatitis, hypoalbuminemia, tumor, hyperplastic cholecystosis, adenomyomatosis, and CHF. The presence of pericholecystic fluid, in the absence of ascites also supports the diagnosis of acute cholecystitis. If there is clinical uncertainty, a nuclear biliary scan (HIDA or DESIDA scan) may be performed.
04 The Common Bile Duct: A dilated common bile duct is another sign of acute cholecystitis. The normal common bile duct inner diameter should be less than 4mm, but may be higher, up to 10mm, post-cholecystectomy. In addition the diameter may be higher in older patients, up to 1mm per decade of life.
05 The Gallbladder Contents: Look for a dilated gallbladder, evidence of stones, and for sludge. Gallstones should be mobile, unless they are impacted in the gallbladder neck, and should cast an acoustic shadow. If all stones are mobile in a patient who remains symptomatic, consider that they may be a red-herring and not the true cause of the patient’s pain. Remember that approximately 15% of adults have asymptomatic gallstones. If there are no sonographic signs of cholecystitis, but a gallstone is impacted (non-mobile) in the gallbladder neck, be suspicious for early cholecystitis and consider admission, additional imaging or at least next-day follow-up. Always also consider early cholecystitis when pain lasts for more than 6 hours, even when the ultrasound is normal except for the presence of a stone. Uncomplicated gallstone attacks usually should only last a few hours. Make sure to explain this to patients if you for some reason decide to send them home with opiates. Attacks lasting longer than that may be something more serious.
06 Pitfalls: Don’t miss a single obstructing gallstone hidden in the gallbladder neck. It can sometimes be hard to see. Also, do not get faked out by an incidental “red herring” gallstone. As previously mentioned, many people have gallstones for years with no symptoms, so if everything does not fit clinically, look further for something else causing the abdominal, flank or rib pain. Some examples include aortic aneurysm, Fitz-Hugh-Curtis syndrome, high appendicitis, PE, kidney stone and pneumonia. Finally don’t miss a AAA, even if it is also incidental, because you did not look for it. Ultrasound techs look. The aorta is not that far away, and should be checked routinely in anyone over the age of 50 who is having an abdominal ultrasound for another reason. Screening saves lives!