Your next patient is a 28 year old female who has been triaged by one of the new nurses as” right lower quadrant pain for about nine hours”. Knowing that clothes generally stay on in the triage area, and the belly button usually remains unseen, the first thing you do after you close the curtain and introduce yourself is to have the patient pull up her blouse and point to where she feels the pain. You are not surprised to find that she is actually pointing to her right upper quadrant. She is not all the way up at the costal margin, but definitely is gesturing superior to the level of the umbilicus. It’s not Murphy’s area, but at least it’s a lot closer to Murphy than it is to McBurney and the pelvis. “Hopefully we can save this woman from an ED pelvic exam” you think silently to yourself.
After localizing the area of interest more accurately, you proceed with the rest of your history. She states the pain started about nine hours ago after eating Mexican food from a street cart. She then developed some generalized abdominal pain, two episodes of non-bloody, non-bilious vomiting, and diarrhea. She seems certain that she has food poisoning and wants the cart owner to be held responsible. You are too seasoned to put the wastebasket diagnosis of “gastroenteritis” at the top of your differential and so you say to her, “You may be right, but let’s make sure it isn’t your gallbladder or your appendix before we blame the food.” Probing deeper into what she means by “diarrhea” you discover she had one non-watery, non-bloody, semi-formed stool, not exactly impressive for a toxigenic food-borne illness. She denies any fever, but states that she came to the ED because she is still nauseated and the pain has become gradually worse and worse. She feels it all over her abdomen, but the right-upper quadrant is where it seems to be most severe.
Triage vital signs were all essentially normal, but you do notice her oral temperature was a tad above normal at 99.2°F. Her head and neck exam shows that she has anicteric sclera and a moist oropharynx.
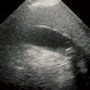
Except for being overweight, the rest of her exam is essentially normal other than some tenderness in the right upper abdomen and possibly some very mild right CVA tenderness. You order a dose of ondansetron, a dose of morphine, IVF’s, and standard blood and urine tests. Her hCG and UA come back normal. Her CBC and CMP are unremarkable. But her pain is still present and it’s not actually getting better. Based on this, she may be right and have a case of “gastro”, but you are still suspicious for a gallstone. Since it is late and you don’t want to call in the ultrasound tech from home on a patient you think you can safely discharge, you decide to use the ED’s ultrasound machine to look for gallstones. Above is the image you capture.

What do you see? Is it safe to discharge this woman home with a diagnosis of biliary colic? Conclusion in the following

Dx: Is this gallstone a red herring?
The ultrasound image shows the gallbladder with a single mobile gallstone with posterior acoustic shadowing. The gallbladder wall is not thickened and there is no pericholecystic fluid (bottom image). The common bile duct does not appear dilated. The novice sonographer might at this point declare, “Aha, (I’m so smart) I found the cause of your pain”, but you realize that this case actually requires a bit deeper thought. The stone does not appear to be impacted in the gallbladder neck and so if it had been the cause of the patient’s pain, that pain should be gone or at least abating by now. However, her pain was actually continuing to worsen. A mobile gallstone may have caused an attack of biliary colic, but if the pain persists beyond 6 hours a diligent search for another cause needs to be considered. If a gallstone is lodged in the gallbladder neck it may be the nidus for early cholecystitis. If it is instead, mobile, it may just be a red herring. Since about 15% of adults have asymptomatic gallstones, the discovery of a gallstone in a patient with abdominal pain does not necessarily mean that it is or was the cause of the patient’s pain. Other common considerations should include acute appendicitis, kidney stones, pancreatitis, ulcers, enteritis, PID or a ruptured abdominal aortic aneurysm. Sending the patient home with a script for hydrocodone may do no more than mask a serious medical condition, adding insult to injury.

Astutely, you inform the patient that she has a gallstone, but you do not think that it is what is making her sick. Suspecting that what she actually may have is neither food poisoning, nor early cholecystitis, but rather colitis or even an atypically located appendicitis, you first repeat your physical exam and then decide to order a CT scan of the abdomen and pelvis. The CT demonstrates acute appendicitis with the tip of the appendix in an atypical location all the way in the right upper quadrant. This patient really forgot to read the medical books before coming in to see you. At least she didn’t have chronically elevated LFT’s from a fatty liver to add to the confusion. You pat yourself of the back for all the pitfalls you have avoided and then call one of your surgical colleagues, who books the OR and removes the appendix without complication.
Tips & Tricks for Ultrasound Evaluation of the Gall Bladder & RUQ
01 Know Your Limitations: Ultrasound may help clarify findings elicited by a thorough history and physical exam. When used correctly, it can greatly improve diagnostic accuracy, and help guide patient management, especially for time-critical diagnosis and treatment of unstable patients. If you use ultrasound in your ED, your department should have a quality improvement program set up that is approved by both ED administration and radiology.
02 Don’t Anchor: A good sonographer or sonologist will perform an ultrasound without forming a diagnosis first. If you scan with a definitive diagnosis in mind, you put yourself at risk for capturing the images that support your diagnosis. Be thorough and systematic with every scan you perform. The goal is to use your sonographic findings as additional data to help you solve the case.
03 The Sonographic Murphy’s Sign: To check for a sonographic Murphy’s sign, which is a sign of cholecystitis, place the ultrasound probe at the maximal point of tenderness in the right upper quadrant. If the probe is placing direct pressure on the gallbladder fundus, you have a positive sonographic Murphy’s sign. False negatives may occasionally occur if the patient has received opiates prior to examination.
04 The Gallbladder Wall: One
sign of cholecystitis is a thickened gall-bladder wall. The normal gallbladder wall can be up to 3mm thick. The most common conditions other than cholecystitis that may cause thickening of the gallbladder wall include hepatitis, hypoalbuminemia, tumor, hyperplastic cholecystosis, adenomyomatosis, and CHF. The presence of pericholecystic fluid, in the absence of ascites also supports the diagnosis of acute cholecystitis. If there is any uncertainty, a nuclear biliary scan (HIDA or DESIDA scan) may be performed.
05 The Common Bile Duct: A dilated common bile duct may be present in acute cholecystitis or with ductal obstruction from choledolcholithiasis. The normal common bile duct inner diameter should be less than 6mm, but may be higher, up to 10mm, post-cholecystectomy. In addition the diameter may be higher in older patients, up to 1mm per decade of life after 60 years of age.
06 The Gallbladder Contents: Look for a dilated gallbladder, evidence of stones, and for sludge. Gallstones should be mobile, unless they are impacted in the gallbladder neck, and should cast an acoustic shadow. If all stones are mobile in a patient who remains symptomatic, consider that they may be a red-herring and not the true cause of the patient’s pain. Remember that approximately 15% of adults have asymptomatic gallstones. If there are no sonographic signs of cholecystitis, but a gallstone is impacted (non-mobile) in the gallbladder neck, be suspicious for early cholecystitis and consider admission, additional imaging or at minimum, next-day follow-up.
07 Pitfalls: Don’t miss a single obstructing gallstone hidden in the gallbladder neck. Also, do not miss a AAA because you did not look. It is not that far away, and should be checked routinely in anyone over the age of 50 who is having an abdominal ultrasound for another reason.