What clinical clues reveal the emergent conditions?
History of present illness:
A 60-year-old male presented to an emergency department complaining of a rash he noticed on his shins that began earlier that day. He described the rash as a few, small red spots without associated itching or pain. Nine hours later, he noted worsening redness and some sloughing of the skin. He took a shower with non-scalding water and began to have constant, aching, throbbing non-radiating pain involving both of his legs, which prompted him to seek medical attention at a nearby emergency department.
The patient stated that he was in his usual state of health that morning with no preceding symptoms. He initially denied new exposures, changes to home medications, or over-the-counter medications although further history revealed two pertinent medication changes. He was started on Plavix two weeks ago after a procedure for “clotting,” which was confirmed to be a fistulogram due to difficulties with hemodialysis. He had been receiving dialysis via a tunneled catheter in the right chest since this procedure.
Additionally, three months ago he began taking Naproxen and Tylenol with codeine for lower back issues as prescribed by his primary care doctor. The outside emergency room physician documented clear bullae formation to bilateral involvement of the hands, feet, legs, forearms, abdomen and back and was transferred to a tertiary care hospital because of a concern for the diffuse nature and rapid progression of his skin lesions.

Review of systems: Negative for fever, chills, chest or abdominal pain, shortness of breath or throat discomfort
Past medical history: end-stage renal disease on hemodialysis, hypertension, congestive heart failure, chronic obstructive pulmonary disease, peptic ulcer disease, pleural effusion s/p thoracentesis (remote) and syncope s/p loop recorder placement.
Social history: occasional beer, but denied smoking or illicit drug use
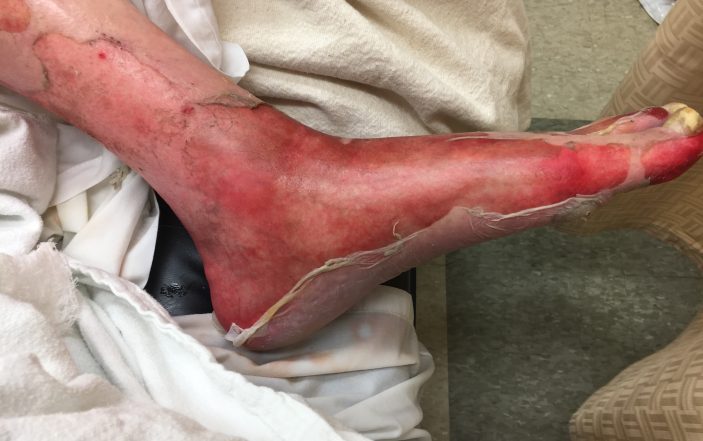
Physical exam in the emergency department revealed an alert male in minimal, but no acute distress. Vitals were: T 93.7F, HR 70, BP 83/52, RR 26, SpO2 94% on room air, wt 78.9kg. Oral exam demonstrated moist mucous membranes, posterior pharynx symmetric noninjected and no intraoral lesions. There was mild conjunctival injection bilaterally. Cardiac and pulmonary exams were unremarkable. There were diffuse blisters involving the scrotum, desquamation of the glans of the penis and eroded red plaques bilaterally involving the forearms, hands, feet, abdomen, back left flank and glans of penis involving 46% total BSA, with no mucosal involvement. (Figures 1-3).

Laboratory evaluation results were: WBC 32.9, Hgb 12.2 platelet clumping unable to quantify, bands 25; electrolytes – glucose 56 Na 138 K 3.9 Cl 109 BUN 29 Cr 3.93; ABG on room air– pH 7.26 pCO2 28 pO2 110; INR 2.12, AST 1368, ALT 605, lactate 7.7

Initial treatment included: IV Fluids – Parkland resuscitation 4cc x 46% BSA x 79kg = 14.5L fluid requirement: 4L normal saline, which were given at the outside hospital and an additional 3.5L lactated ringers bolus was given on arrival to the emergency department at the tertiary care hospital. A central line was placed for norepinephrine administration for hypotension. Bair hugger, wound care and warmed IV fluids were administered for hypothermia and broad-spectrum IV antibiotics vancomycin and piperacillin-tazobactam were initiated.
Consultations included: renal for inpatient hemodialysis, burn surgery for wound management and ICU admission, and dermatology for evaluation and punch biopsy.
Discussion:
The patient presented with an undifferentiated dermatologic emergency. Dermatologic emergencies encompass a wide array of disease, but can be characterized as either a primary skin disease or a severe systemic illness with skin manifestations. Stevens-Johnson syndrome, toxic epidermal necrolysis, angioedema, exfoliative erythroderma and DRESS syndrome (drug rash with eosinophilia and systemic symptoms) are all examples of can’t miss primary skin emergencies.
Clinical clues to these emergent conditions are the presence of fever with a blistering or denuding rash, full body redness, palpable purpura, or a rash occurring in the immunocompromised patient. Severe systemic illnesses such as necrotizing fasciitis, meningococcemia, staphylococcal or streptococcal toxic shock syndromes, staphylococcal scalded skin syndrome and rocky mountain spotted fever must also be considered along with the aforementioned cases as they will all require aggressive supportive measures and ICU level of care to address hypotension and multiorgan dysfunction or failure.
Stevens-Johnson syndrome and toxic epidermal necrolysis lie along the same spectrum of mucocutaneous skin reaction that is typically precipitated by a new medication initiated one to three weeks prior to manifestation. Symptoms may include fever and mucositis (tender conjunctivitis or odynophagia) that precede painful erythematous macules that rapidly progress to flaccid bullae and epidermal detachment. Ocular involvement is fraught with complications and may result in blindness. Common precipitants include antibiotics, antiepileptics and NSAIDs.
After removing the offending agent, treatment is entirely supportive as neither IVIG, corticosteroids nor the combination of the two has shown any benefit over supportive care alone. Mortality is less than 10% in Stevens-Johnson syndrome and roughly 30% for toxic epidermal necrolysis, which is most often due to septicemia.
DRESS syndrome has several important differences from SJS-TEN. The latency period after introduction of the inciting agent is far longer at two to eight weeks. The rash is far more variable — typically a morbilliform rash that becomes edematous, but may contain vesicles, bullaee, pustules, purpura, target lesions or erythroderma. The morbidity and mortality attributed to DRESS syndrome is more visceral in nature including hepatitis, pneumonitis, myocarditis, pericarditis, nephritis, thyroiditis, synovitis and colitis. Fulminant hepatitis is the leading cause of death. Hallmarks of the disease are leukocytosis with eosinophilia (seen in 90% of patients), morbilliform rash, edema of the face and visceral involvement. Treatment is again supportive in nature as corticosteroids and immunosuppressants like cyclosporine have not shown significant benefit over supportive care alone.
The facial swelling in DRESS syndrome may be confused for angioedema. Angioedema most commonly is precipitated by medications but may be hereditary or idiopathic as well. The resulting edema has a well circumscribed, waterbag appearance and is caused by increased vascular permeability that poses an immediate threat to the airway. Treatment includes removal of the offending agent and aggressive airway management. Androgens, C1 esterase inhibitor concentrate, icatibant and fresh frozen plasma may all be considered for the treatment of hereditary angioedema.
Exfoliative erythroderma is distinguished from other dermatologic emergencies most easily by the typical appearance of its rash which is scaly, erythematous and generalized typically involving 90% or more of total body surface area. Most patients with this condition will have an underlying skin disorder such as eczema, psoriasis, cutaneous T-cell lymphoma or leukemia, pityriasis, paraneoplastic syndrome or dermatomyositis. Drug reactions may also cause exfoliative erythroderma. The mortality rate approaches 20% due to hypotension, electrolyte imbalance, congestive heart failure and enteropathy that result from excessive vasodilation. Treatment is again centered around supportive care.
Findings:
The presumptive diagnosis in this case was toxic epidermal necrolysis given the classic progression of the rash from painful macules to bullaee and subsequent epidermal detachment of a large body surface area. Evidence of mucositis was also present noting the conjunctival and genital involvement. The patient had been on NSAIDs for knee pain for some time, but had recently been started on Plavix and exposed to IV contrast for his fistulogram.
Although rare, a few case reports involving TEN precipitated by IV contrast and Plavix have been described. All three of these medications may have been the offending agent or trigger.
The diagnosis was not definitively confirmed as the patient did not survive long enough to receive biopsy results despite extensive wound care, aggressive fluid resuscitation and management of hypothermia, hypotension and multiorgan dysfunction.
REFERENCES:
- Bechtel, M. Dermatologic emergencies [Power point slides]. Retrieved from: https://ccme.osu.edu/WebCastsFiles/483%20-%20Dermatologic%20Emergencies%20Final%20-%202.pdf
- Chen, A. (2013). Dermatologic emergencies [Powerpoint slides]. Retrieved from: https://www.bumc.bu.edu/im-residency/files/2013/07/Derm-Emergencies-July-2013.ppt
- Choudary, S., McLeod, M., Torchia, D., and Romanelli, P. (2013). Drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome. Journal of Clinical and Aesthetic Dermatology, 6 (6): 31-37.
- Davidovici, B. and Wolf, R. (2007). Emergencies in Dermatology: Diagnosis, Classification and Therapy. Expert Review of Dermatology, 2 (5): 549 – 562.
- Freiman, A., Borsuk, D., and Sasseville, D. (2005). Dermatologic emergencies. Canadian Medical Association Journal, 173 (11): 1317 – 1319.
- Schneck J. (2008). Effects of treatment on the mortality of Stevens-Johnson syndrome and toxic epidermal necrolysis: A retrospective study on patients included in the study on patients included in the prospective EuroSCAR study. Journal of the American Academy of Dermatology, 58: 33-40.