“Nothing in medicine is black and white,” you hear your colleague explain to one of the rotating medical students. She looks perplexed as he goes on to explain that there is an “art” to medicine and just because she learned how to evaluate and manage a certain type of patient presentation one way, doesn’t mean there aren’t other “right” ways to do it. The overeager medical student has her mouth half-open to retort back in response, when she sees you out of the corner of her eye subtly shaking your head to warn her to stop before she puts her foot in her mouth. You decide this would be a good opportunity to ask her to follow one of your senior residents as he gets ready to perform a bedside aorta ultrasound on another patient in the department.
The patient who needs the scan is a 56-year-old otherwise healthy female who presented to the ED with a chief complaint of “severe abdominal pain” after she finished lifting boxes of heavy books at her job the day before. She states her pain is worse with movement and is better when she lies still. She has never had pain like this before, and today, it is 10 out of 10 in severity. The pain is described as sharp and tearing, but it does not radiate to her chest or back. She has no other associated symptoms, and she has tried Ibuprofen without any relief.
Her vital signs are all completely within normal limits and her physical exam is only remarkable for tenderness to palpation over her left rectus muscles, and a seemingly pulsatile aorta palpable through her thin abdominal wall. She has no rebound or guarding on abdominal exam, and she has no other abnormal findings. Given her symptoms and her palpable aorta, your senior resident decides it would be prudent to do a quick scan of her aorta to make sure nothing catastrophic is imminent.

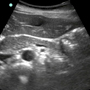
Your resident, with the medical student in tow, places the curvilinear probe on the patient’s abdomen, just below the subxiphoid process and obtains the following image (top). After he scans through the aorta in this plane, he rotates the probe so that the indicator is pointing towards the patient’s head and obtains this image (bottom).

What do you see on the images? Do you have an explanation for the patient’s abdominal pain? Conclusion in the following

Dx: Normal aorta, but what about the liver?
The patient’s aorta (labeled “A”) appears normal in both the transverse and longitudinal views next to the inferior vena cava (IVC). The diameter is less than 3 cm and there is no evidence of any intraluminal clot or dissection flap. Careful review of the ultrasound images demonstrates some abnormalities in the glimpses we get of the surrounding organs. A small piece of the liver can be visualized on both scans just near-field to (below) the aorta. Within the parenchyma of the liver, there is a well-defined lesion seen on both images.

Before your medical student can ask any questions or make any statements in front of the patient that may put everyone in an uncomfortable situation, your senior resident tells the patient that he’s going to order a comprehensive abdominal ultrasound to evaluate some things he visualized on the scan. He explains that the machines in the radiology department have better resolution and imaging capabilities so often times they can clarify subtle things we see on our bedside scans.

The patient is wheeled away for her comprehensive abdominal ultrasound in the radiology department, which leaves ample time to review all of her labs and urinalysis ordered from the ED. Her UA is normal, and her CBC and CMP are only notable for a hemoglobin of 9.0 along with a scattering of anisocytosis, microcytes, hypochromia, ovalocytes, target cells and tear drop cells. As the patient’s comprehensive ultrasound images begin uploading on the PACS machine, you can’t help but gasp at what they show (bottom). What do you see on the scans?
The patient has multiple metastatic lesions seen throughout her entire liver. Your senior resident delivers the news with both empathy and kindness and arranges for the patient to be admitted for a comprehensive oncology evaluation as an inpatient.
You take a moment to provide some teaching pearls to your residents and the medical students who are on service. You remind them that although most things in medicine are not “black and white” there are a few rules that are pretty well accepted:
- Never overlook or ignore questionable or abnormal findings.
- Don’t anchor into a diagnosis and potentially ignore other etiologies on your differential diagnosis. The three most common decision-making heuristics are anchoring, availability and attribution. Try your hardest to avoid these pitfalls:
- Anchoring: refers to the tendency to seize on the first symptom, physical exam finding, or laboratory abnormality and anchor one’s mind onto an answer prematurely.
- Availability: refers to the tendency to assume that an easily remembered prior experience explains the new situation you are facing.
- Attribution: refers to the tendency to invoke stereotypes in our minds and attribute symptoms and findings to those stereotypes.
You are your patient’s best advocate. Be comprehensive and fight for what’s right for them.
Tips & Tricks for Abdominal Ultrasonography
01 Bedside ultrasound can provide you with valuable data to help you make critical diagnoses and expedite patient care. Always approach each scan with an open and inquisitive mind. You may be surprised by what you find.
02 The purpose of performing a focused, limited bedside scan is to answer a select set of questions concerning the patient’s presentation. It is important to make sure you are asking the right set of questions, and to be careful not to anchor into a diagnosis before you get all of the data back.
03 Always visualize the adjacent structures surrounding your target organ of interest. For example, when you seek out to evaluate the aorta, scan through the surrounding liver parenchyma, too. Changes in the surrounding organs can alter the appearance of your target structure, and abnormalities of adjacent structures may provide you with the reason for your patient’s symptoms.
04 When scanning thro
ugh a target organ, obtain at least 4 different views of the area of interest. Use the body’s natural acoustic windows, such as the liver and the urinary bladder, to improve your views.
05 The aorta scan is best performed using the low frequency curvilinear transducer. Start with the transducer in a transverse fashion with the indicator marker pointed towards the patient’s right side. Obtain a good view of the IVC, aorta, and vertebral body.
06 Once all three structures have been identified, slide your probe over the aorta and follow it down through its bifurcation just above the umbilicus.
07 Findings suggestive of a AAA:
- Increased aortic diameter >3 cm
- Focal dilatation (1.5 times the adjacent aortic segment)
- Lack of normal tapering distally
- Presence of intraluminal thrombus
08 Do not mistake a fluid-filled loop of bowel to be an enlarged aorta. Make sure that the round, hypoechoic structure you think is the aorta doesn’t demonstrate any peristaltic movements on ultrasound.
09 When in doubt, you can always apply color-Doppler. Remember that the aorta will demonstrate pulsatile flow, whereas the IVC will show a low flow rumble of color. Bowel should not show any consistent pattern of color flow.
10 Be comprehensive with your scans. Don’t stop scanning just because you have found the answer you were looking for. Often times, interesting pathology can be discovered in the periphery of a focused scan. You may not always know exactly what you are looking at, but at least you can provide the patient with the data and knowledge to take the next best step towards improving their care.