After evaluating this article participants will be able to:
1. Understand critical injuries associated with blast injuries, incorporating these concepts into clinical practice
2. Identify blast injuries in separate organ systems, avoiding missed injuries and improving patient care
3. Improve care of patients with blast-related injuries
There is no doubt that the likelihood of treating explosive-related injuries is increasing around the globe. Between 1999 and 2006, both terrorist-related explosive incidents and associated injuries increased dramatically. In Operation Iraqi Freedom and Operation Enduring Freedom, over 40,000 men and women have been injured and 4,300 have died. Of those deaths, over 1,800 were related to explosive injuries and 25% of returning troops have explosive-related traumatic brain injury. Thus, the importance for emergency physicians to have a significant understanding of the pathophysiology and the specific management options of explosive injuries cannot be overstated.
Breaking Down the Blast
When an explosion occurs, a solid or liquid rapidly converts to gas. This reaction results in a significant exothermic reaction. A concentric blast overpressure (BOP) wave travels out from the point of detonation and is associated with extreme blast winds from displacement of surrounding air. This BOP can reach over 100 atmospheres of pressure (ATMs) while the winds can be up to several hundred miles per hour depending on the size of the explosion. The BOP is amplified at close distances and underwater or when its energy reflects back on a victim (e.g., proximity to a wall). Specifically, closed-space explosions (e.g., indoors or on a bus) are of great concern due to these amplified forces (see figure 2). Victims in these settings have higher injury severity scores, incidence of explosive-related injuries, and overall mortality.
click on image to view pdf of graphs

Explosive injuries fall into five main categories depending on their causative mechanisms (see table 1). While secondary, tertiary and quaternary blast injuries result from mechanisms that most emergency physicians see on a regular basis, primary blast injury patterns are relatively unique and deserve special attention. However, it must be noted that secondary blast injuries due to fragmentation occur with much greater frequency. Explosive fragments can be propelled for hundreds to thousands of yards causing severe injury, whereas the blast overpressure wave exerts its force over tens of yards.
Primary blast injuries are caused by barometric forces on the body at areas of significant air-tissue interface. Thus, the pulmonary, gastrointestinal, and auditory systems are at greatest risk. While certain BOP thresholds may correlate with certain injuries, it is important to recognize that these relationships are not absolute (see table 2). For instance, exposures to high pressure explosions may not rupture the tympanic membrane because of head location, ear protection, or other factors (see insert on opposing page for specific injuries).
With explosive-related injuries occurring with an ever increasing frequency, blast injuries are no longer the sole the concern of battlefield physicians. It’s critical that EPs know the unique diagnostic and management aspects of these devastating injuries.
It is critical to suspect blast lung injury when evidence of a significant blast overpressure is present. Most often a chest radiograph will show bilateral pulmonary infiltrates in a butterfly pattern. If a patient remains symptomatic with a normal radiograph, admit or observe the patient for six to eight hours to exclude delayed development of contusion and edema, respiratory distress, or hypoxia. Two specific challenges exist when managing a complicated blast victim with pulmonary injury. The first is that impaired oxygenation may require positive pressure ventilation, which may in turn worsen a patient’s barotrauma or risk for arterial air embolism. When positive pressure ventilation is indicated, lung protective settings (e.g., low tidal volumes, pressure-controlled, permissive hypercapnia) can be combined with low positive end-expiratory pressures (PEEP) and 100% FiO2 to maximize the ventilation and oxygenation while minimizing the risk of additional systemic air emboli. The second challenge is balancing the need for volume resuscitation in a hypotensive patient with pulmonary blast injury. Excessive fluids may worsen pulmonary compliance in patients with pulmonary contusions, necessitating positive pressure ventilation and the concomitant risks.
Patients with hemodynamic instability should undergo emergent surgery. Permissive hypotension (systolic blood pressure of 90 mm Hg) has been advocated to improve outcomes in patients without traumatic brain injury. In hemodynamically stable patients with abdominal pain perform a computed tomography scan to evaluate for abdominal solid organ injury. If negative and the patient reports ongoing abdominal complaints, observe the patient for 6-8 hours for intestinal contusion and mesenteric injury or consider explorative laporatomy.
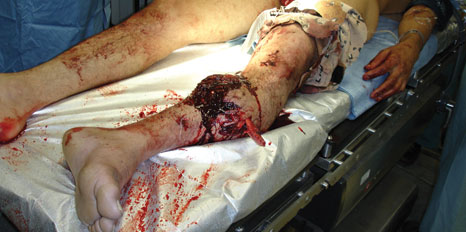
Fifty-four percent of combat injuries involve the musculoskeletal system. Fragmentation injuries, which can appear small and benign at first glance, can hide devastating deep tissue or visceral injuries and demand exploration and diagnostic work-up. Recent military conflicts have involved very high rates of fasciotomies for compartment syndrome related to explosive injuries. Deep tissue injuries, burns, and aggressive volume resuscitations increase tissue edema and compartment pressures leading to ischemia. The exact role of the blast overpressure and blast-induced release of inflammatory mediators is uncertain. Finally, traumatic amputations are a musculoskeletal system injury that results from very high blast overpressures. Boney fractures concomitant with high blast winds cause partial or complete extremity amputations. These injuries do not necessarily occur at joints and are associated with very high immediate and delayed mortality rates (up to 85%).