When the meds aren’t working.
In sign out you receive an elderly patient with a hip fracture waiting to be admitted for surgery. You are having trouble controlling her pain. She is continuing to require multiple doses of opioid pain medication with little relief. Her nurse calls you, “Is there anything else we can give?”
You go assess the patient. She seems a little drowsy, but awake and appropriate. Visibly uncomfortable, she asks, “Doc, this pain is excruciating! The medications are not working.”
Initially, you consider giving her another dose of pain medication, but with her being already drowsy and concerns of possible apnea and aspiration, you instead grab the ultrasound machine.
You let her nurse know, “I’m going to do a nerve block for pain control, could you grab a spinal needle, syringe and 0.5% bupivacaine?”
The patient is laid down with her right hip slightly externally rotated and abducted. You place the high frequency linear probe just distal to the inguinal ligament and search for her femoral vessels. Remembering prior ultrasound guided femoral line placements you’ve done, you know to look for the nerve lateral to the femoral artery.

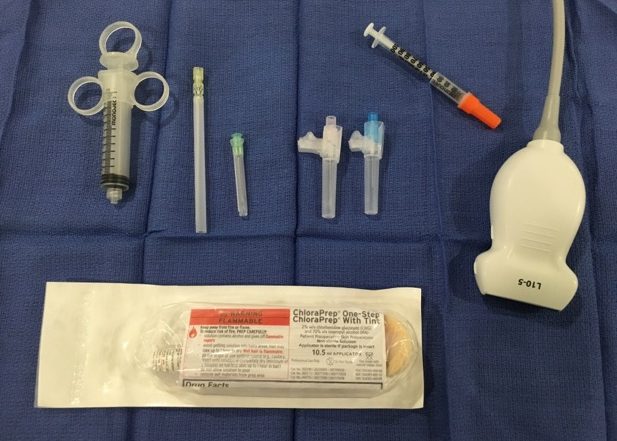
Equipment. You will need a high frequency linear, chloroprep or betadine to clean the skin, a sterile probe cover or tegaderm, a needle long enough to reach the target nerve (LP needle), and an insulin needle to numb the skin (optional).
Using a sterile field, you insert your needle lateral at a 45-degree angle using an in-plane approach, so you can see the needle during the entire procedure. Going through the fascia iliaca you avoid any vascular structures and inject 20ml of bupivacaine along the nerve sheath.
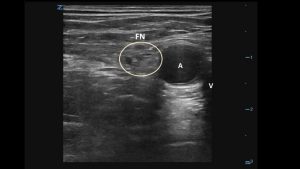
- Anatomy. The femoral nerve (FN) sits lateral to the femoral vein (V) and artery (A), deep to the fascia iliaca. Nerves have a honeycomb appearance on ultrasound.
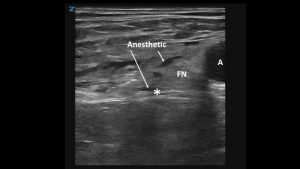
- The block. Aim the tip of your needle below and lateral (*) to the femoral nerve (FN). This will elevate the nerve and bring it closer to the skin surface. After injecting anesthetic, re-direct the tip of the needle above and lateral to the nerve.
The patient tolerates the procedure well. After 30-minutes you reassess her. She is laying comfortably in bed, “Thanks doc! That new med you gave me really worked.”
Pearls and Pitfalls for performing an Ultrasound-Guided Femoral Nerve Block
- Ultrasound guided peripheral nerve blocks are a great adjunct, or alternative, to opioids for pain control in the emergency department.
- The femoral nerve block is helpful in patients presenting with hip and femur fractures, patellar fractures, anteromedial thigh lacerations and abscesses.
- As with any nerve block, you want to be aware of surrounding structures including the femoral artery and vein, and fascia iliaca.
- Failing to penetrate the fascia iliaca may result in block failure.
- Using an in-plane approach allows you to visualize the entire length of the needle, its trajectory and know where the needle tip is at all times.
- Before performing any peripheral nerve blocks you want to be familiar with local anesthetic systemic toxicity (LAST), and how to manage it.