A 32-year-old male presented to the emergency department with concerns about a possible infection in his left lower extremity. The patient had a history of HIV and poorly controlled type 1 diabetes. He presented with a chronic ulcer to the left medial ankle and had an incision and drainage to the area about 45 days prior. Over the past 3 days the pain and swelling had progressively worsened. The patient denied any systemic symptoms of nausea, fever, or chills.
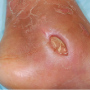
Examination revealed a 3 cm x 2 cm ulcer to left medial ankle with surrounding soft tissue swelling, erythema, and yellow discharge (figure 1). Distal pulses and sensation were intact. No crepitus was appreciated on exam, however there was pain with palpation along the calf. Radiographs of the leg demonstrated “soft tissue swelling of the ankle with a lateral defect and subcutaneous air; cortical irregularities of the medial malleolus and medial talus concerning for osteomyelitis”.

Figure 1: The 32-year-old patient in front of you had this chronic ulcer incised and drained in the ED 45 days ago. What will you do?
An ultrasound was done to evaluate for a drainable fluid collection. The ultrasound demonstrated hypoechoic fluid containing tiny echogenic foci with dirty shadowing in the perifascial region of the Achilles tendon and gastrocnemius. This extended proximal from the wound nearly up to the knee, consistent with fluid and air in the tissue (figure 3). Based upon the U/S and radiographs, a diagnosis of necrotizing fasciitis was made. Vancomycin and piperacillin-tazobactam were immediately started. General Surgery and Orthopedic Surgery were consulted. The patient was emergently taken to the OR. The operative findings were consistent with necrotizing fasciitis and osteomyelitis of the distal tibia. He underwent debridement of the soft tissue and left lower extremity and osteotomy of medial malleolus (figure 4).

Figure 2: Radiographs of the leg demonstrated “soft tissue swelling of the ankle with a lateral defect and subcutaneous air.
Figure 3: The ultrasound demonstrated hypoechoic fluid containing tiny echogenic foci with dirty shadowing in the perifascial region of the Achilles tendon and gastrocnemius

Figure 4: Debridement of the soft tissue
During the hospital stay, the patient required multiple episodes of debridement and ultimately a below the knee amputation. Cultures taken from the wound were positive for group C Streptococcus, Proteus mirabilis, and Streptococcus mitis. Patient was discharged after three weeks to a skilled nursing facility in stable condition. He did not require antibiotic therapy as an outpatient and the amputation healed well.
Disease Features
Necrotizing fasciitis is a rare disease that is rapidly progressive and can be difficult to diagnose.1,12 Physical exam early in the disease is often nonspecific until the patient has systemic manifestations such as septicemia and septic shock. In addition to the lack of specific exam findings early in the disease, there is no single diagnostic investigation with good sensitivity and specificity outside of surgical exploration.3 This makes the past medical history particularly important especially if the patient has an associated immunodeficiency. Early on, many cases are wrongfully diagnosed as cellulitis.7
Even with the early administration of broad spectrum antibiotics and surgical intervention (debridement), mortality ranges 20-40% in most studies but has been reported to be as low as 6-9%.4,5,6 Delays in diagnosis and treatment increase risk of mortality, amputation, and extensive surgical reconstruction.3 As such, it is important for the emergency physician to consider necrotizing fasciitis under the appropriate conditions in order to reduce the risk associated with this fatal disease.
MRI has been reported to have a sensitivity of 90-100%, however it is not readily available and should not delay initiating treatment.2
Specific ultrasound findings of necrotizing fasciitis have previously been described as thickening of the fascia with associated fluid accumulation along the deep fascial layer.8,9 Using these criteria, one study found the sensitivity and specificity were 88.2 and 93.3% respectively.9 In addition to the fascial thickening and perifascial fluid, this case also demonstrated air in the fascial planes. Air in the fascial planes on radiographs is often taught as a classic finding for necrotizing fasciitis. However, air on plain radiographs is seen in less than 25% of cases.10
Ultrasound has a high sensitivity and specificity for detecting subcutaneous air (100% and 87.5% respectively).11 Clinicians should also be familiar with the characteristic ultrasound appearance of air within tissue: tiny, often mobile, echogenic foci with dirty, grey shadowing posteriorly.11 While a lack of subcutaneous air does not rule out the possibility of necrotizing fasciitis, the presence of air in the SQ tissue or the fascial plane in the appropriate clinical setting, mandates immediate initiation of antibiotics and surgical consultation, as earlier treatment has been shown to reduce morbidity and mortality.2 The practitioner must realize that ultrasound is limited and when findings are equivocal, the physician should continue further workup and imaging as required by the clinical scenario.
In the case presented, bedside ultrasound was used as an adjunct in the diagnosis of necrotizing fasciitis in the Emergency Department. The ability to use ultrasound at the bedside and obtain rapid results makes it useful in such a rapidly progressing condition.
References
1. Bellapianta JM, Ljungquist K, Tobin E, Richard U: Necrotizing Fasciitis. J Am Acad Orthop Surg 2009;17:174-182.
2. Sarkar B, Napolitano LM: Necrotizing soft tissue infections. Minerva Chir 2010;65:347-362
3. Sultan HY, Boyle AA, Sheppard N: Necrotising fasciitis. BMJ 2012;345:e4274 doi: 10.1136/bmj.e4274.
4. Bernal NP, Latenser BA, Born JM, Liao J: Trends in 393 necrotizing acute soft tissue infection patients 2000-2008. Burns 2012;38:252-260.
5. Oglive CM, Miclau T: Necrotizing soft tissue infections of the extremities and back. Clin Orthop Relat Res 2006;447:179-186.
6. Sudarsky LA, Laschinger JC, Coppa GF: Improved results from a standardized approach in treating patients with necrotizing fasciitis. Ann Surg 1987;206:661-5.
7. Ryssel H, Germann G, Kloeters O, Radu CA, Reichenberger M, Gazyakan E: Necrotizing fasciitis of the extremities: 34 cases at a single center over the past 5 years. Arch Orthop Trauma Surg 2010;130:1515-1522.
8. Chau CLF, Griffith JF: Musculoskeletal infections: ultrasound appearances. Clinical Radiology 2006;60:149-159.
9. Yen ZS, Wang HP, Ma HM, Chen CS, Chen WJ: Ultrasonographic screening of clinically-suspected necrotizing fasciitis. Acad Emerg Med. 2002;9:1448-1451
10. Puvanendran R, Huey JCM, Pasupathy, S: Necrotizing fasciitis. Canadian Family Physician. 2009; 55:981-987.
11. Butcher CH, Dooley RW, Levitov AB: Detection of subcutaneous and intramuscular air with sonography: a sensitive and specific modality. J Ultrasound Med. 2011; 30:791-795.
12. Lancerotta L, Tocco I, Salmaso R, Vindigni V, Bassetto F: J Trauma Acute Care Surg. 2012; 72:560-566.