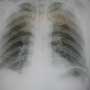
Triage walks back a 45-year old Hispanic man with chest pain. “He said ‘dolor’, and pointed right here,” says the triage nurse, indicating on himself a mid-sternal location. “Good enough for me. I brought him straight back.” Your Spanish is a little thin, but you get the high points – “nausea, vomito, mucho dolor,” the patient says, making good eye contact. Physical exam shows P 70, BP 130/70, RR 22, sat 98% RA and tenderness in the epigastric region. His cardio-pulmonary exam is normal, and the first 12-lead EKG is normal.
It’s a good story for angina, and from the primary nurse’s assessment, you gather that these are new symptoms. Easy admission! The usual diagnostics – including CXR, EKG and cardiac enzymes – are pending, and you order aspirin, morphine and anti-emetic treatment along with a fluid bolus. A short while later the radiologist phones you (hey, it’s during the daytime). “You know,” he starts out between sips of espresso, “I’m not entirely sure about this chest X-ray. There might be a little air in the mediastinum. If it’s alright with you, I’ll ask the radiology techs to drop off a little gastrografin down there.” Sure, you think, no problem. I’ve got other fires to fight. “Let me know what you find,” you quip back.
A short while later you review both the CXR and the gastrografin swallow. What do they show? What comes next?
Dx: Boerhaave Syndrome
My physician mentors always told me, “everything is in the history.” Time and again, especially with the busy pace of ED practice, I have returned to a case only to pick up a small piece of history that alters my diagnostic or disposition plan.
In this case, the missing history was “I got my chest pain after I vomited,” a classic history for Boerhaave syndrome (esophageal perforation). After the gastrografin study, which showed a lower esophageal leak (arrows), we – God forbid – went back with a better translator and got this information. In this case, we were lucky rather than good. My own review of the initial chest X-ray was (and still is) that the film is normal. The radiologist, suffering from “recent CME-itis,” probably overcalled this film – even though it led to the correct diagnosis.
Boerhaave syndrome (aka Boerhaave’s syndrome) is a classic but rare cause of chest pain, and like aortic dissection, may mimic acute coronary syndrome in its severity and persistence of symptoms. Perforation usually occurs near the gastroesophageal junction, leading to leakage of esophageal contents and subsequent mediastinitis, which is associated with high mortality, especially if the diagnosis is delayed. Classically, the diagnosis is made by esophagography (gastrografin swallow), which shows a leak of contrast. However, CT scanning is highly sensitive for air in the mediastinum – the sine qua non of Boerhaave’s – and may be superior to esophagography in ruling out the diagnosis. At the very least, it is certainly helpful as an adjunctive imaging method. Treatment is surgical.
This case emphasizes the need for a good translator in any translingual encounter, and a lot of patience. Sit and listen, go back and re-evaluate the patient, look at the vital signs and listen to the family.
Dr. Dallara practices EM in Virginia and North Carolina, and directs the Emergency Medicine PREP Course. www.emprepcourse.com