“Get them out of here,” you hear your colleague next to you exclaim. “Treat ‘em and street ‘em. We need to open up some more beds.” You wrinkle your nose and wonder quietly if we’ve all become so focused on throughput that we’ve somehow lost sight of why we all signed up for this job in the first place. As if to put salt into the wound, one of your senior residents comes up with three new cases to present, but notes that all three are already “dispo’d” and just need your blessing.
You pause to listen to his stories and tell him, “Great. Let’s talk about what we can do to help some of these people.” Blessed with good insight and even better people-reading skills, your resident reconsiders his fast and furious approach and slows down the tempo just a bit. The first two patients were indeed relatively straightforward, and once you do a little bit of probing and drop a few “pearls of wisdom,” you are comfortable that he didn’t just perform superficial evaluations to keep the revolving door turning. You tell him you will go see those two patients next.
Happy that he’s two for two so far, your resident launches into the tale of his third patient. He’s a 56 year-old male who presents to the ED with left leg pain. A few weeks ago, he had an uncomplicated operation for perforated diverticulitis and intra-abdominal abscess management. Since then, he has noted increased left leg pain. The patient denied any other systemic symptoms including chest pain, shortness of breath, palpitations, fevers, chills, nausea, vomiting, abdominal pain, or lightheadedness. Your resident notes that the patient’s vital signs were normal and that the only significant clinical findings were a non-tender abdomen with a well healed surgical incision, and mild left lower extremity swelling. To summarize his assessment and plan, your resident goes on to explain that he performed a bedside ultrasound, diagnosed the patient with a DVT, started him on Lovenox, and called the medicine team for admission so that he could be bridged to Coumadin. The patient’s blood work results have been reviewed and the patient is in line to be seen by the medicine team.
Not wanting to miss a good teaching opportunity, you review the various management options available as your resident pulls up the images he obtained during the patient’s DVT scan. You finish your review of the various anticoagulation options and take a long, hard look at the DVT images he acquired.

What do you see in the image? What other images do you want to see? What else do you want to know about this patient? Conclusion in the following
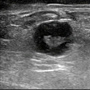
Dx: Femoral Artery? Look Again

LN=lymph node superficial to the common femoral vein and common femoral artery
Knowing that the devil is in the details, you ask your resident to describe what we are looking at on the ultrasound image. He states that there is a round, anechoic vascular structure with a hyperechoic clot in the middle. When you ask him to tell you which vessel he saw the clot in, he states authoritatively, “the common femoral vein.” You then ask him to identify where the common femoral artery is on his image. You can almost feel his consternation when he suddenly realizes his mistake. “That’s not a vessel is it?” he asks, as he is begins walking towards the order sheet to cancel his Lovenox order.
After he gracefully explains to the patient what has happened, and palpates the enlarged lymph nodes he saw on his bedside ultrasound, you help your resident repeat the left lower extremity vascular ultrasound. You walk him through how to map out the pertinent vessels and identify the corresponding, adjacent structures. As you scan through the femoral triangle, you help him identify the superficial inguinal lymph node sitting right above the common femoral vein and artery (pictured above).
A quick review of the lower extremity anatomy helps him remember to map out each vessel’s course and you finish your scan by reminding him to obtain both longitudinal and transverse views of the vessel to ensure he is indeed looking at the intended target structure.
One negative DVT study later, your resident has learned a valuable lesson about one of the common pitfalls in bedside vascular ultrasonography, but even more importantly, he has seen that haste can indeed make waste.
Lymph nodes quick guide:
Normal: Size Reactive: Size <2cm, duration <2wks, soft, tender, may have fever
Cancer: Varying sizes, hard, matted, duration >3wk, weight loss
source: Quick Essentials: Emergency Medicine 4.0
Pearls & Pitfalls for Vascular Ultrasound
1. Bedside ultrasound can provide you with valuable data to help you make critical diagnoses and expedite patient care. Minimize the chances of a false positive or false negative scan by approaching each scan with an open and critical mind. Don’t inadvertently “see” what you are hoping to find.
2. Always visualize and identify adjacent structures and anatomical landmarks. Figure out “where you are” in the body before you jump to any conclusions. Novice sonographers will place the ultrasound probe right over the point of interest, make a quick diagnosis, and put themselves at risk for common pitfalls. Improve your accuracy by obtaining multiple views of the target structure.
3. Most vascular ultrasounds are performed with a high frequency, linear array transducer. Pay close attention to the depth markers on the side of the image and ask yourself if the sonographic images you see make sense with anatomical expectations.
4. Lymph nodes will appear as round or oval shaped hypoechoic structures on bedside ultrasound. Enlarged lymph nodes can often be mistaken for a clotted vessel in the short axis view. Obtaining a long axis view can help delineate the borders of the structure you are evaluating. Lymph nodes will have a well-defined border when you rotate your probe.
5. Utilize power and color Doppler to provide you with physiologic and anatomic information that can help you make the proper diagnosis.
6. Always correlate your sonographic findings with the clinical picture. Evaluating lymph nodes via ultrasound is beyond our scope of clinical practice as emergency physicians. Ensure appropriate follow up and further evaluation if suspicious appearing lymphadenopathy is visualized on a bedside scan. Abnormal lymph nodes are usually rounder with peripheral or mixed vascularity.