You really hope today’s shift is better than yesterday’s. You had to tell a really nice homeless man that internal medicine refused to admit him for his femoral DVT because he doesn’t meet “admission criteria” and that he would have to find the means to pay for his outpatient Lovenox on his own. Then a patient came into the ED with chronic pack pain, and you ended up diagnosing him with metastatic prostate cancer with spinal metastases.
Your next patient seems nice enough. She’s 29 years old and is accompanied by her husband at the bedside. She starts by saying, “Please just tell me my baby is OK. We’ve been trying to conceive all year!” She is a G1P0 who is otherwise healthy and without any co-existing conditions. She came into the ED because she’s been having some mild cramping and some intermittent spotting. Her OB appointment is next week, and she has not had any prenatal care. She is taking over-the-counter prenatal vitamins regularly, and Tylenol to help with her pain. She appears anxious and worried and is hanging on every word, gesture, and movement you make in the room.
Her vital signs are normal and her physical exam is only remarkable for some mild suprapubic tenderness on palpation, and a scant amount of blood near her closed cervix in her vaginal vault. You send off a serum quantitative hCG level given the fact that she doesn’t know exactly when her last menstrual period was. You also order a peripheral IV so you can send off a basic CBC with diff, BMP, pT/pTT, type & Rh, and provide her with IVFs to get her prepared for her pelvic ultrasound and UA. You give her some Tylenol for her abdominal cramping and keep her NPO otherwise.
She questions you with her eyes intently and says, “What do you think could be going on with my baby? My pregnancy test at home was positive. I just don’t know why I’m having all of this bleeding and pain.”

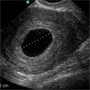
You gently coax her into the lithotomy position so that you can perform a good transabdominal pelvis scan followed immediately by a transvaginal evaluation of her uterus and adnexa. You insert the intracavitary probe with the indicator pointing anterior towards the patient’s pubic symphysis. You carefully sweep through the patient’s uterus and this is what you see (above).
What do you see on your ultrasound? What do you need to do now? Conclusion in the following

Dx: Blighted Ovum
Within the uterus, you see a clear view of a gestational sac that measures almost 30 mm in its widest diameter. As you fan through, you do not see any evidence of a yolk sac or a fetal pole (above image).
The patient’s labs start to return and she has a quantitative hCG level of 3500 mIu/mL. With a quantitative hCG level that high, you would expect to see a yolk sac already.
Because the mean gestation sac measures >14 mm, and there is no visible yolk sac on the scan, it is likely that your patient has an anembryonic gestation or blighted ovum at this time.
You walk back into your patient’s room and pull up a chair so that you can have an uninterrupted conversation with her and her husband about her ultrasound findings. You hold her hand and explain to them that the ultrasound images obtained today suggest that she is having a blighted ovum in her uterus and that it doesn’t look promising for a viable pregnancy. You take your time to explain to her and her husband that it wasn’t anything they did wrong, and that it doesn’t mean they can’t try again in the near future. You reinforce that many couples have had miscarriages or a blighted ovum, and are still able to conceive and have beautiful, healthy babies in the future. Your nurse provides them with multiple pamphlets and references that they can read and refer to with any questions they may think of after they leave the ED. You recommend subsequent imaging in the next week or two to ensure that nothing else has progressed unexpectedly. The patient and her husband thank you for your time and empathy, and schedule their outpatient radiology and OB appointments as they walk out of your ED. It doesn’t appear as if your clinical black cloud is going to clear up anytime soon. You prepare for your next case with hopes of sunshine and silver linings.
Tips & Tricks for Ultrasound Evaluation of a Blighted Ovum
01. Always begin your pelvic ultrasound with a full bladder and a transabdominal scan to map out the important organs and structures. A full bladder provides an excellent acoustic window. Remember that everyone’s anatomy is different and once you start performing the intracavitary portion of the exam, your view is more limited because of the confined space.
02. On your transabdominal scan, determine how the uterus is lying and determine if there is any obvious free fluid or intrauterine findings.
03. To perform the endovaginal portion of the pelvic ultrasound, start by covering the intracavitary transducer with a gel filled sheath and apply a copious amount of clean gel to the outside of the sheath.
04. Insert and advance the transducer with the indicator marker pointing anteriorly towards the patient’s pubic symphysis. Alternatively, you may let the patient insert the probe herself as this method is often less uncomfortable.
05. Scan through the uterus in this sagittal plane, noting the presence or absence of a gestational sac, yolk sac, fetal pole, fetal heartbeat, etc. If the patient has a positive urine or pregnancy test, and the uterus appears empty, an ectopic pregnancy should be suspected.
06. If you see a gestational sac, carefully evaluate the size and shape of the sac, and correlate the size of the sac to the quantitative hCG level and date of the patient’s LMP.
07. When the gestational sac is larger than 10 mm and no yolk sac is identified, it is likely that the patient has a blighted ovum or anembyonic pregnancy.
08. If you see a yolk sac that is larger then 7 mm but you do not see a developing fetal pole, this also suggests a nonviable intrauterine pregnancy.
09. Remember that the fetal pole is typically seen on transvaginal ultrasound at approximately 5-6 weeks gestation. You should see a fetal pole when the gestational sac is >18 mm on transvaginal ultrasound or >25 mm on transabdominal ultrasound.
10. At times, it is difficult to determine if the sac you are seeing is a true gestational sac, or a pseudogestational sac associated with an ectopic pregnancy. To determine the difference, look at the location of the sac. A gestational sac will be seen within the decidua, whereas pseudogestational sacs are usually in the endometrial canal. When color Doppler is applied over a gestational sac, it will be “warm” and highlight with color. A pseudogestationa
l sac is usually “cold” and no color is visualized on color Doppler.
11. Rememeber, the mean diameter of the gestational sac +42 should = the gestational age of the fetus in days. Use that number to help determine if you see the expected fetal structures for that size of the gestational sac.
12. Patients with a suspected blighted ovum warrant an OB/Gyn consultation in the ED or very close outpatient OB/Gyn follow-up. It is important that patients undergo a follow-up ultrasound with a high-resolution ultrasound machine to ensure that a small yolk sac or fetal pole is not overlooked.

36 Comments
Cyst
The same thing is now happening to me. I had my 1st ultrasound and found out I was 4weeks and 5days pregnant. Even my blood test came back positive. But when I went back for my 2nd ultrasound, it showed an empty sac but it was growing by 4cm. Please is there anyone on here who had the same problem but ended up with a successful pregnancy? And what was wrong?
I went to see the doctor after 7 weeks 6 days. Doctor told me the sac is empty ,not able to see the baby.i was so worried and doctor said I cannot see the baby growing. Doctor appoints me after 2 weeks for another ultra sound check up.i wish everything will be ok and pray for me,,,
Same thing has happened to me
Neelam, I am having the same problem at 6 weeks 3 days. I have my next ultrasound in 2 weeks. How did yours turn out? I guess I am trying to be positive and praying that everything is ok. Hope all went well with you.
how did this go?
Hi Dear,
How did your next week scan went?
All looks okay now?
Yes; my sister. I’m experiencing the same thing. She keeps telling me to wait….
I have the same experience. First scan its Twin. Second scan both sac empty but growing
Few months ago, I had a 6cm dermoid cyst removed from my right ovary via lap cystectomy. My period was normal post-op until last month, it’s 2 weeks late. I went to see my Obgyn, he performed an ultrasound and found an empty sac just like the ones you showed here. He also asked me to take hCG test, it came back negative. He gave me NE to make my period come and reminded me to come and see him again on the 12th day of my period.
Me and my husband’s been trying to conceive for a year now, but all came back negative. It’s heartbreaking to know that this one’s also negative.
I’ve been having all the symptoms, frequent urination, nausea, backpain, increased appetite and headache… Now I’m having a second thought, whether I should take the NE now or give it another week.
Hello,
Question for you – I had an ultrasound at 6 weeks, 5 days. A gestational sac was visible but no yolk sac or fetal pole. My hcg was 31,700. I had a second hcg test 96 hours later and it was 51,000. I have a second ultrasound scheduled for next week but am wondering what you think? It’s very hard to wait. Thanks in advance!
Hey Rebecca, what news did you receive if you don’t mind me asking
I’m 5 weeks had an ultrasound doctor and I seen gestational sac but no yolk sac or fetal pole my hcg was 4723 and I’m doing another he said it was ugh hcg but she should see yolk sac he scheduled me an appointment to see him in two weeks tomorrow or Thursday I will get a call to see if my levels go higher I’m scared .
Hi, I know I’m really late but how did it go? I’m in the same position now…
Could you let me know what ended up happening? I’m literally in the exact same situation. 5 weeks, 5000 hcg but no yolk sac. I’m freaking out
Am 9w 6d pregnant spotting pink blood when wiping out in the bathroom and I have seen my gynaecology today and the scan looks like the one above. Doctors said baby not developing well and had to go for womb scraping. Is the no way that I can change?
I was 3 months when I went in to find out the baby was not viable and had actually started to “disolve”. It was devastating. I prayed for it to change, but it did not. I did wait a week and went back to make sure was not viable before the DNC.
Hi, I’m six weeks and four days from what the gestational sac shows but there is no fetal pole. Is this a blighted ovum. I have been trying to conceive for months now and now that I have this happens again. A miscarriage, I am not bleeding or spotting or nothing. So when does everything happen. Since I am already six weeks and four days. Will I start bleeding next week when I am seven? I am already assuming this is a miscarriage because it is literally a third time two years later.
Hey Rebecca
The same thing just happened to me and I am waiting for the second ultrasound mind sharing what happened?
Thandie and Rebecca what was your result? Going through the same thing
I’m experiencing the same. Do you have an outcome?
Hi Rebecca, I’m in exactly the same situation – how did yours work out?
What was update
I’m presently going through the same thing. I’m 7 weeks but no sight of the baby. I’m scheduled to go back next weej
Hi Tanya, do you mind sharing what happened with you? I’m going through the same thing.
I am nearly 6 weeks. They can’t locates the pregnancy sac or anything. I had an ectopic pregnancy in 2018, a chemical pregnancy in November last year and now my gynaecologist seems to think this may be another ectopic pregnancy. My hcg is only in the 800s but still slowly rising, my progesterone plummeted from 42 to 12 in 24 hours. I have no bleeding or pain which I did with both of the others. I’m terrified of losing my second tube as I will have to try IVF if I do. How long to I keep waiting before it’s too late and I do lose my tube??
Hi Tanya, I’m in the same situation – how did it work out for you? I have to wait a week but the thoughts of that when I feel so sad is hard.
Thanks
Does anyone reply? I’m 7 weeks, No sac. HGC 12,000, 3 days prior it was 4000. Anyway, next ultrasound is next Fri. Any positive vibes or outcomes would be greatly appreciate.
Hey Rae,
How did it go? I am at 5 weeks and 3 days or 6 weeks. My ultrasound looks like the one above and the sonar showed warm, or red. The doctor said I was pregnant but I have a gut feeling I am not.
Hi,
I came across this article and felt the need to share my story in hopes that it could help anyone going through the same thing. At my first ultrasound, my gestational sac was found empty as well and I was immediately told it was a blighted ovum. I was in shock and also probably a little denial. After being told to wait for it to “pass naturally” I sought after a second opinion from another group of doctors. To my dismay, they had determined the same thing. For some reason my hcg levels kept rising and my body wasn’t realizing I wasn’t “pregnant” anymore so I had to schedule a dnc. The whole experience broke me. At the time I felt I had failed or I was doing something wrong by having the dnc but I know now that it was what was meant to be. God doesn’t make mistakes. If you are experiencing a blighted ovum and you are feeling all of the painful confusing feelings I felt, please know that a. You aren’t alone and b. Everything will happen as it should. You will get through this, I promise you. Don’t give up hope.
Hi what happen when u go for ur next scan… I go trgh tha same i went there Tuesday thy say tha sac is empty i ws so down cuz i tried aftr we lost a child on 33weeks pregnant… I need to ho back on 9may but im so scared
According to my LMP I would be 9 weeks and 1 day. However some heavy bleeding and slight cramping sent me to the ER. The doctor said no fetal pole was detected and HCG was only 2000. Which could either mean I am earlier than expected or miscarriage. I have 7 living children I bled with all 7 and was told it was a threatened miscarriage but this time it seems way off. I have to wait a whole week to follow up with my doctor. I am so anxious and I can’t sleep.
I’m 7wks 3days. Had 2nd TVU today and still just sac and yolk with no visible fetal pole. One more Ultrasound next week before we call it. Longest wait of my life.
I am also waiting for my last ultrasound tomorrow before calling it. Thus past two weeks have been a roller-coaster. I should be 10 weeks tomorrow
I am going through the same thing. I am measuring at about 7 weeks. We saw a gestational sack and a yolk sack but no fetal pole. My doctor told me it’s 50/50 but there were some abnormalities. Yesterday I thought my Symptoms started to go away but then today I woke up and felt like my boobs were being crushed again and spent more that half the day dry heaving. I got back for my next ultra sound on Tuesday but I have hope that my baby will be there. I just keep praying.
What is the update?