How the involuntary hold creates violence.
Nearly half of all emergency physicians report being assaulted in the emergency department during their career,[1] with many assaults resulting in significant injury or even death.
Given recent studies indicating that emergency physicians lead the nation in career burnout, and the simultaneous critical shortage of nurses, [2] the threat of physical violence at work deeply exacerbates an escalating public health crisis.
It begs consideration: Could some of these assaults on healthcare workers have had iatrogenic, and thus avoidable, causes? Given human nature and the inherent instability of addiction, intoxication, and mental illness, are our medical interventions themselves escalating the situation? How many of these assaults are, in fact, iatrogenic violence?
A 29-year-old male with a history of methamphetamine addiction, chronic suicidal ideation, and multiple prior visits to your emergency department is brought in by police after behaving erratically shortly after injecting methamphetamine, fentanyl, and drinking an unknown amount of alcohol.
The patient is handcuffed but is exhausted from struggling and falls asleep. Upon awakening, he begins vomiting and declares, “I wish I was dead.” This is witnessed by a nurse, who notifies a behavior health specialist to whom the patient refuses to talk; after receiving ondansetron, the patient returns to a comfortable sleep.
Unable to complete a cooperative psychiatric assessment, the behavioral health counselor recommends an involuntary hold until the patient can be assessed by psychiatry. The patient awakens after a long nap. He is still intoxicated with an unsteady gait and demands to leave. The physician attempts to verbally de-escalate the patient; when unsuccessful, the physician orders lorazepam and haloperidol. The patient refuses, becoming threatening and agitated.
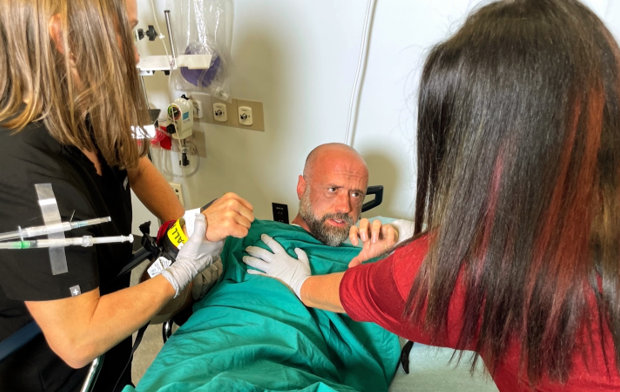
A hold-and-release for medication administration is attempted by nursing and hospital security, and during the ensuing tussle, the patient punches a nurse, fracturing her jaw. The nurse never returns to work, compounding the acute staffing crisis in a healthcare system already at its breaking point.
The patient spends the next two weeks in the emergency department awaiting a psychiatric bed and is discharged shortly after transfer with a diagnosis of drug abuse and antisocial behavior. The nurse does not press charges as she believed it doubtful to have a successful prosecution due to the assault being defended as a “psychiatric emergency” and her understandable hesitancy to further identify herself to this dangerous patient.
Did this have to happen? Why didn’t the hospital let the patient leave when he asked to? Could a career-ending assault on the nurse have been avoided? How would the outcome change if the patient were allowed to leave? Most (but not all) of the time, the patient would go on to metabolize the substances he earlier ingested and return to his baseline, not bringing harm to anyone else or himself.
Iatrogenic violence, defined here as intervention by the physician (or police or EMS) that unleashes patient violence, is a deadly and potentially preventable complication. Drugs, alcohol abuse, and mental illness in patients are a daily component of every emergency physician’s workload. Personality disorders and mundane criminality in the general public further impede the hospital’s mandate of caring for the sick and injured who have nowhere else to go.
Allowing a patient to leave the emergency department while intoxicated, much less after professing any sort of suicidal ideation, is anathema to most emergency physicians; moreover, it is a morass of medicolegal liability. What if: The patient stumbles in front of a bus; assaults someone else; goes on to kill themselves, and the physician is accused of dismissing a psychiatric medical condition?
These outcomes do occur but must be balanced against the legal, ethical, and medical quandary of confining a patient against his or her will, as well as the questionable benefit of brief psychiatric hospitalization for suicidal ideation. There is little evidence that hospitalization prevents suicide, [3, 4] and there is a chilling suggestion that the social and psychological damage of involuntary commitment (IVC) may in fact increase it.[5]
Before restraining a potentially violent patient against his or her will, we must first consider “do no harm” [6] –or at least, do less harm than good. In our state of North Carolina, the average patient waits 12.5 days for a psychiatric bed after presenting to an emergency department, [7] which is a not insignificant consequence for a patient who got drunk and, in the misery of a hangover, verbalized wishing he was dead. Those 12.5 days can push an overwhelmed hospital to the breaking point. At the same time, ED boarding can push a mildly depressed patient to violence. A lengthy involuntary hold can wreak disastrous results on a patient’s life, even causing the patient to lose his or her job, spouse, or children, thereby increasing the patient’s shame, despair, or hopelessness.
Extreme intoxication from drugs and alcohol is endemic in the United States. If EMS were to patrol a college town after a huge football win, they’d likely find some fans inadvisably beyond a healthy level of intoxication.
If confined in the emergency department until clinically sober, a small minority of the fans would naturally become outraged and physical. A smaller minority still may seriously injure a provider, be injured themselves, or even die in restraints. In Kowalski v. St. Francis Hospital and Health Centers, a patient sued the emergency physician after he left the ED against medical advice (AMA) while intoxicated and was struck by a car leaving him a quadriplegic.
The courts found the hospital not liable—and moreover, they did not have the right to restrain him against his will even while intoxicated. [8,9] Contrast this with the police officers in Boulder, Colorado, who handcuffed a severely intoxicated man and placed him face down in the transport van. While taking him to a detox facility, he died. The officers were convicted of manslaughter and sentenced to up to six years in prison.[10]
In many cases, when we restrain a patient against his or her will, we are trading a small risk of them later harming themselves or someone else, for the certain risk of stressing the patient, and the additional risk of peril to the providers and other patients in the ED. Chaos is contagious, and a department managing chaos cannot provide the best care to any of its patients.
If a patient truly lacks the capacity to make decisions, certainly we should do everything within reason to get them medical care. However, not all intoxication, drug use, or psychiatric diagnosis renders a patient incapacitated. Intoxicated and mentally ill patients are due the rights provided in the Patient Bill of Rights including “safe, considerate, and respectful care, provided in a manner consistent with your beliefs”;[11] however, the rights and safety of the other patients in the emergency department should not be infringed upon.
Requiring the emergency department to function as a prison for involuntary holds, where physicians and nurses, and hospital security provide services normally performed by trained guards, surely infringes on the rights of hospital staff. [12]
At some time during their life, 13.5% of the population of the United States will have thoughts of suicide[13] (including 1/3 of medical residents during their residency). [14] Tragically, 46,000 people per year will go on to complete it, making a gross risk of 0.4% for every person that seriously contemplates suicide.[15] This is a risk not to be trivialized, but it should be considered alongside other standards of care.
Compare, for example, a chief complaint of chest pain and a HEART score of 3 where the ACEP guidelines freely acknowledge that a patient with a 2% risk of a major adverse coronary event should be allowed to go home due to the risks of overdiagnosis and iatrogenic harm.18 We confine, sedate, and frequently aggressively restrain patients to “keep them safe” to prevent a suicide risk of far less than that. Is restraint really “for their own good”? There is little evidence that brief psychiatric stays prevent the long-term risk of suicide [4,5] while there are many documented cases of death while being restrained for acute agitation. [15]
This is a double-edged sword, like many decisions in emergency medicine. The same attorney may simultaneously sue one hospital for not committing patients against their will who go on to injure themselves and sue another for “illegally confining” patients with an IVC. So, what is morally right? The most devastating legal risk may be patient death while in custody or under medical care, which also seems most morally fraught.[18]
The Model Penal Code allows “an exception from the assault statute for physicians… who act in good faith in accordance with the accepted medical therapy.” [19] A physician can physically restrain a patient against his will if, in good faith, the physician believes that the patient’s psychiatric emergency is placing him in “imminent danger” of harming himself. Do we truly believe that a patient on his or her 20th visit to the ED with alcohol intoxication and years of passive suicidal ideation is an imminent danger to himself?
If the medically stable patient wants to leave AMA, is it worth the medicolegal and ethical risk of physically restraining him? We must give pause to the concerns of the United Nations that forced psychiatric treatment involving “the infliction of severe mental pain or suffering” even if unintended by the perpetrator may be considered torture if that suffering was reasonably foreseeable.[20]
If we must IVC every patient who is a danger to themselves, then it follows that we must IVC every patient who is using cocaine, binge drinking, smoking cigarettes, or non-compliant with their antihypertensives. If we must IVC (or forcibly restrain to evaluate) every patient who has suicidal thoughts, then we must physically confine the 12.2 million Americans who have suicidal thoughts each year. [15] There should be a higher bar to remove a person’s rights, to compel their presence in the ED for hours-to-days awaiting an in-depth psychiatric evaluation. There should be an even higher bar to put physicians and nurses in harm’s way.
We propose a call to action: Just as Six et al., created the HEART score and determined the risk of a major cardiac event,[21] we call on the emergency psychiatric research community to determine not only what risk factors are higher and lower, like the Columbia Suicide Severity Screener, but to determine the absolute risk of suicide for patients in the low, medium, and high-risk groups.
Such a determination can help weigh those risks against the violence a patient may perpetrate against health care providers or be subjected to by those seeking to confine them against their will. If healthcare resources were plentiful, if the committal process were gentler, and if all patients had job security and family support, factors might differ. But in a climate where inpatient beds are staggeringly scarce, we must acknowledge the uncertain benefit of involuntary confinement for emergency department patients with intoxication or passive suicidal thoughts versus the iatrogenic harm caused by involuntary commitment or forced ED evaluation.
We must work with our lawmakers to obtain legal protection against frivolous lawsuits for reckless or criminal acts that patients choose to make after leaving the emergency department, based on the false construct that restraining them against their will for hundreds of hours in a bright, noisy environment would have made them more peaceful. Is a 12-day involuntary confinement in a non-psychiatric hospital beneficial to mental health? Moreover, will that patient ever again be honest about their feelings with a health care provider?
We must educate the public and the press about evidence-based interventions that help with drug and alcohol abuse and prevent suicide and dispel the erroneous belief that the benefit of locking someone up against their will always outweigh the harm.
References:
- ACEP Emergency Department Violence Poll Research Results: Prepared for the American College of Emergency Physicians. Marketing General Incorporated. September 2018. https://www.emergencyphysicians.org/globalassets/files/pdfs/2018acep-emergency-department-violence-pollresults-2.pdf
- Gorman VL. Future Emergency Nursing Workforce: What the Evidence Is Telling Us. J Emerg Nurs. 2019 Mar;45(2):132-136. Doi: 10.1016/j.jen.2018.09.009. Epub 2018 Oct 24.
- Waterhouse J, Platt S. General hospital admission in the management of parasuicide. A hospitalized controlled trial. Br J Psychiatry 1990; 156: 236–42.
- Van der Sande R, Van Rooijen L, Buskens E, et al. Intensive in-patient and community intervention versus routine care after attempted suicide. A hospitalized controlled intervention study. Br J Psychiatry 1997; 171: 35–41.
- Large MM, Kapur N. Psychiatric Hospitalisation and the risk of suicide. Br J Psychiatry 2018; 212, 269–273. doi: 10.1192/bjp.2018.22
- Hippocrates/Kuhn, Karl Gottlob (ed). Magni Hippocratis Opera Omnia (tomus III, 395) Leipzig: Car. Cnoblochii, 1827 BIU Santé (Paris). http://www.biusante.parisdescartes .fr/histmed/medica/cote?hippokuhnx03
- Knoph T. New mental health data show ‘unsustainable’ burden on NC hospitals. NC Health News. August 2022. https://www.northcarolinahealthnews.org/2022/08/22/emergency-department-burden-shown-in-mental-health-data
- Bitterman RA. New York’s High Court Rules Hospital Is Not Liable for Failure to Retain an Intoxicated Patient. ED Legal Letter. October 1st, 2013. https://www.reliasmedia.com/articles/63947-new-york-s-high-court-rules-hospital-is-not-liable-for-failure-to-retain-an-intoxicated-patient#:~:text=The%20Court’s%20Ruling.,act%20under%20New%20York%20law.
- Kowalski v. St. Francis Hospital and Health Centers, et al., No. 128, (NY Ct. of App., June 26, 2013).
- Oravetz J. ‘They made decisions not to follow the rules’: Former deputies sentenced after manslaughter conviction. 9News. Denver, Colorado. November 4th, 2021. https://www.9news.com/article/news/crime/former-deputies-sentenced-manslaughter-conviction/73-b6bde94b-7ff6-4d98-9ade-0c1080f15dc6
- Patient Bill of Rights. NIH Clinical Center. May 2021. https://clinicalcenter.nih.gov/participate/patientinfo/legal/bill_of_rights.html
- Parker M. Physician Bill of Rights. KevinMD. February 2017. https://www.kevinmd.com/2017/02/physicians-bill-rights.html
- Kessler RC, Borges G. Walters EE. Prevalence of and Risk Factors for Lifetime Suicide Attempts in the National Comorbidity Survey. Arch Gen Psychiatry. 1999;56:617-626.
- Laramée J, Kuhl D. Suicidal ideation among family practice residents at the University of British Columbia. Can Fam Physician. 2019;65:730–5.
- Suicide Prevention. Center for Disease Control and Prevention. October 2022. https://www.cdc.gov/suicide/
- Tomaszewski CA, Nestler D, Shah KH, MD, et al. Clinical Policy: Critical Issues in the Evaluation and Management of Emergency Department Patients With Suspected Non–ST-Elevation Acute Coronary Syndromes. Ann Emerg Med. 2018;72:e65-e106.
- Rubin BS, Dube AH, Mitchell EK. Asphyxial deaths due to physical restraint. A case series. Arch Fam Med. 1993 Apr;2(4):405-8. doi: 10.1001/archfami.2.4.405. PMID: 8130919.
- Phillips N, Schmelzer E. Colo. officers, paramedics charged in Elijah McClain’s death. The Denver Post. September 1, 2021. https://www.ems1.com/legal/articles/colo-officers-paramedics-charged-in-elijah-mcclains-death-09mm0mnDatRI2cWa/
- Wexler DB. Seclusion and restraint: Lessons from Law, Psychiatry, and Psychology. Int J Law Psychiat. 1982;5:285.
- United Nations. Torture and other cruel, inhuman or degrading treatment or punishment. Report of the Special Rapporteur*. Human Rights Council Forty-third Session. (A/HRC/40/59, para. 41; and A/HRC/37/50, para. 60). March 2020. https://documents-dds-ny.un.org/doc/UNDOC/GEN/G20/070/73/PDF/G2007073.pdf?OpenElement
- Six AJ, Backus BE, Kelder JC. Chest pain in the emergency room: value of the HEART score. Neth Heart J. 2008;16:191–196.

1 Comment
I believe the issue that continues to be avoided is a basic legal tenet. We have gone on much too long absolving patients for violent behavior toward healthcare workers (I am speaking on behalf of nurses in particular) has become the norm. Just because patients are intoxicated, delusional, or suicidal/homicidal, they are not precluded from right vs. wrong judgment and, therefore, should not be held to a different standard. Those issues can be considered mitigating circumstances, however, that is a decision for the legal system. I also believe that healthcare workers defending themselves in a violent manner (when necessary) should not be discouraged by healthcare systems who are petrified of liability. I appreciate this article and author’s thoughts on the issue. We need a multi-dimensional approach to the issue, however, staff and public safety needs to take precedence at some point.