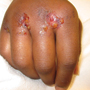
The patient is a 24-year-old male with right hand inflammation and discomfort after punching another human in the mouth 12 hours prior to arrival. Patient had no past medical history and had no other injuries and was without allergies to medication. Patient was taken to the operating room for an I & D from skin to tendon of second, third and fourth webspace. There was found to be no extensor tendon injury and no joint involvement. Patient was given IV antibiotics in the hospital and was treated with Augmentin upon discharge. Patient was seen in clinic and found to be healing well with no signs of active infection.

What are the important considerations with a “fight bite”?

Clenched Fist Injuries
“Fight bites” or clenched fist injuries, which typically result when one person strikes another in the teeth with a closed fist, may appear innocuous at first glance, but can lead to significant morbidity due to both direct trauma and subsequent infection. Delayed presentation, patient intoxication, misleading history, or lack of patient cooperation may lead to inadequate examination and wound exploration in the emergency department, significantly increasing a patient’s risk for soft tissue infection, septic arthritis, or osteomyelitis. Additionally, many patients may ignore these wounds until they develop significant pain, swelling, or purulent drainage. As a result upon presentation may already have an established complicated infection, further increasing the morbidity associated with “fight bites.”
Clenched fist injuries typically present as traumatic lacerations over the third and fourth metacarpophalangeal joints (MCP) or proximal interphalangeal joints (PIP) of the patient’s dominant hand. The initial laceration may be small in appearance, however these wounds are highly prone to infection due to the close proximity of the skin to the underlying joint capsule. If the laceration extends into the joint capsule, when the fist is relaxed immediately following injury, bacteria from the mouth and skin are carried by the extensor tendon into the deep compartments and tendon spaces of the hand. Infection may then spread to the potential spaces within the subcutaneous, subfascial, subtendinous, and web space tissue. Pathogens are typically polymicrobial with streptococcus S. aureus, and anaerobes mostly commonly isolated from wound cultures.
Wounds are typically 12-15mm in length over the MCP or PIP joints of the patient’s dominant hand. In patients who present immediately after sustaining a clenched fist injury, wounds may appear innocuous. However, presentation may be delayed for several days until patients awaken with a painful, throbbing, swollen hand. Swelling and erythema typically spread proximally rather than distally, and patients may experience reduced range of motion of the ICP, MCP, or wrist joints. Not uncommonly patients appear to have pain out or proportion to exam, which should raise concern for periosteal penetration and osteomyelitis. In addition to infection, patients may also have underlying extensor tendon injuries or metacarpal neck fractures, further limiting range of motion and contributing to pain and swelling. Purulent discharge, lymphangitis, fever and other signs of systemic infection are rarely present even when extensive soft tissue infection occurs.
 Aggressive management of clenched fist injuries include analgesics, wound care, antibiotics, and tetanus vaccination. Wounds should be irrigated copiously with normal saline followed by careful exploration and removal of any visible foreign debris. Radiographs should be considered to evaluate for underlying fracture, osteomyelitis, or foreign body. Additionally, immediate consultation of a hand surgeon is advised to allow for surgical evaluation of tendon, bone, or joint injuries, and to further assess nerve or muscular injury. Emergency physicians should initiate empiric antibiotic therapy to cover the most common isolates. This includes aerobic gram positive organisms such as Viridans streptococci (100%), group A strep (53%), and S aureus (29%). Oral anaerobic flora peptostreptococcus, fusobacterium and bacteriodes (25-55%) along with gram negative organisms such as Eikenella corrodens (25%) should also be considered. Enterobacteriaceae and Pseudomonas species are rarely cultured so therapy generally does not need to be tailored to these organisms. (See Table 1 and 2 click to enlarge). Monotherapy with agents that lack activity against Eikenella corrodens, including first-generation cephalosporins, penicillinase-resistant penicillins (nafcillin, oxacillin), macrolides, clindamycin, metronidazole and aminoglycosides should be avoided. Following evaluation, the injured extremity should be elevated and immobilized from the fingers to the elbow in a position of comfort that maintains the maximal length of ligaments and intrinsic hand muscles. In patients who have completed a primary immunization series, but have not had a booster in more than five years, a tetanus toxoid and diphtheria (Td) booster should also be administered in the emergency department. Tetanus immunoglobulin and toxoid should be administered to patients who have had two or fewer primary immunizations.
Aggressive management of clenched fist injuries include analgesics, wound care, antibiotics, and tetanus vaccination. Wounds should be irrigated copiously with normal saline followed by careful exploration and removal of any visible foreign debris. Radiographs should be considered to evaluate for underlying fracture, osteomyelitis, or foreign body. Additionally, immediate consultation of a hand surgeon is advised to allow for surgical evaluation of tendon, bone, or joint injuries, and to further assess nerve or muscular injury. Emergency physicians should initiate empiric antibiotic therapy to cover the most common isolates. This includes aerobic gram positive organisms such as Viridans streptococci (100%), group A strep (53%), and S aureus (29%). Oral anaerobic flora peptostreptococcus, fusobacterium and bacteriodes (25-55%) along with gram negative organisms such as Eikenella corrodens (25%) should also be considered. Enterobacteriaceae and Pseudomonas species are rarely cultured so therapy generally does not need to be tailored to these organisms. (See Table 1 and 2 click to enlarge). Monotherapy with agents that lack activity against Eikenella corrodens, including first-generation cephalosporins, penicillinase-resistant penicillins (nafcillin, oxacillin), macrolides, clindamycin, metronidazole and aminoglycosides should be avoided. Following evaluation, the injured extremity should be elevated and immobilized from the fingers to the elbow in a position of comfort that maintains the maximal length of ligaments and intrinsic hand muscles. In patients who have completed a primary immunization series, but have not had a booster in more than five years, a tetanus toxoid and diphtheria (Td) booster should also be administered in the emergency department. Tetanus immunoglobulin and toxoid should be administered to patients who have had two or fewer primary immunizations.
Patients with evidence of clinical infection on exam should be admitted to the hospital for continued administration of intravenous antibiotics and further evaluation. Patients with complicated infections, such as tenosynovitis, may require prolonged therapy (up to 6 weeks) as well as operative management with incision, drainage, and debridement of necrotic tissue. If after consultation with a hand surgeon, the patient does not appear to have a laceration that invades the joint capsule or clinical signs of infection, discharge home on oral antibiotics may be considered. However, prompt and reliable follow-up is an absolute requirement when considering discharging a patient home.