You find yourself working in a small – I’m talking very small – rural hospital in South America for your summer “break”. The only imaging modalities available are plain X-ray and a small portable ultrasound machine your group-of-four brought along for the trip. There is no MRI, no CT, and no formal ultrasonography. It might not help much if there were any of these however, as the are no radiologists, or any other specialists for that matter, in the hospital. It’s just you and your three friends: a general surgeon, an OB/GYN, and an orthopedist. The two local doctors who are general practitioners have taken the week off. There is, however, a much larger hospital in the nearest city, but it is over a day’s journey away.
Your current patient is a 55-year-old obese diabetic male who presents with right flank pain that has been getting worse for about 7 days. He was started on Bactrim 3 days ago for a urinary tract infection, but continues to worsen. He denies diarrhea, hematuria or dysuria, but has had fever and has been vomiting about once per day. His medications include glipizide, Tylenol, and Bactrim.
 On exam he is calm, nontoxic, and pleasant, but looks to be in mild distress. His vital signs aren’t bad. Temperature is 97.4, blood pressure 98/58, pulse 108, and respiratory rate is 16 wit a pulse-ox of 98% on room air. Eyes are anicteric. Oropharynx is moist. Lungs are clear. Abdomen is soft and non-tender, but the back has right-sided CVA tenderness. The remainder of the exam is normal.
On exam he is calm, nontoxic, and pleasant, but looks to be in mild distress. His vital signs aren’t bad. Temperature is 97.4, blood pressure 98/58, pulse 108, and respiratory rate is 16 wit a pulse-ox of 98% on room air. Eyes are anicteric. Oropharynx is moist. Lungs are clear. Abdomen is soft and non-tender, but the back has right-sided CVA tenderness. The remainder of the exam is normal.
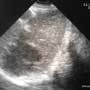
Laboratory data showed a nondiagnostic urinalysis, possibly because he was already taking antibiotics. The metabolic panel was notable only for a glucose of 216, a sodium of 122, and a creatinine of 1.6. The CBC had a white count that was elevated at 21.4. An ultrasound of the kidneys was normal, but the following image of the liver was also taken. What structures are shown in this image? What abnormal finding is shown?
What do you see in the image?
This image demonstrates a view of the right upper quadrant using the 2.5 MHz curvilinear probe just below the costal margin. The liver is moderately echoic and takes up most of the image. The abscess has an anechoic/hypoechoic center with a slightly hyperechoic surrounding rim. The diaphragm is very hyperechoic and separates the liver in the near field (top of image) from the lung in the far field (bottom left of image). The right kidney cannot be seen in this image, but is nearby.
Liver abscesses may be caused by a variety of organisms. Pyogenic abscesses cause about 80% of cases and are often polymicrobial with E. coli or Klebsiella pneumonia being the primary pathogen. Entamoeba histolytica causes about 10% of cases and Candida albicans or another fungal organism is the usual cause in the remaining 10%. Treatment usually entails antimicrobials targeted at the suspected organism or organisms and drainage, often performed percutaneously.
Your patient is admitted to the hospital overnight for antibiotics and antiparasitics. In the morning he is improved and is discharged so that he can get himself to the closest urban hospital where they perform a CT guided drainage of the abscess. The cultures grow out Klebsiella pneumoniae.
Imaging Liver Masses
1. Liver Abscesses: Abscesses may be single or multiple. They are characterized by a hypoechoic fluid collection with a hyperechoic shaggy wall. Early on the abscess contents may be close in echogenicity to the liver parenchyma, but as the contents liquefy further, the fluid becomes hypoechoic or even anechoic.
2. Hemangiomas: Hemangiomas are the most common primary tumor of the liver and are usually solitary. The are quite hyperechoic, often appearing bright white, and are also homogenous and well circumscribed.
3. Metastases: Metastases may be single or multiple. They may be of similar echogenicity to the liver, but in a more heterogeneous pattern. Often liver metastases or primary liver masses are more echoic that the liver due to increased vascularity.
4. Cysts: Liver cysts may be single or multiple. They are usually benign when they have thin walls and an anechoic fluid center. Posterior enhancement may be noted.
5. Gallbladder Stones & Polyps: For a good case example see the November 2009 issue of Soundings or check it out at www.erpocketbooks.com
6. During a focused bedside ultrasound, you may happen to come across a liver mass during the scan. The liver is an excellent acoustic window, so many bedside ultrasound applications will provide you with a great view of the liver parenchyma. Although EM physicians are not typically trained to make “formal” interpretations of liver sonograms, it is useful to understand some hepatic ultrasound basics so that the appropriate management decisions can be made. When a liver mass is discovered during a focused, bedside scan, explain to the patient the limitations of your scan, and ensure that appropriate, comprehensive imaging is arranged for a definitive diagnosis.
7. Practice Makes Perfect: With bedside ultrasound there is no substitute for experience. The more ultrasounds you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is.
An image library of normal and abnormal ultrasounds helps immensely, and we can help. Just click on the ultrasound library link within the Real-Time Readings department.
 On exam he is calm, nontoxic, and pleasant, but looks to be in mild distress. His vital signs aren’t bad. Temperature is 97.4, blood pressure 98/58, pulse 108, and respiratory rate is 16 wit a pulse-ox of 98% on room air. Eyes are anicteric. Oropharynx is moist. Lungs are clear. Abdomen is soft and non-tender, but the back has right-sided CVA tenderness. The remainder of the exam is normal.
On exam he is calm, nontoxic, and pleasant, but looks to be in mild distress. His vital signs aren’t bad. Temperature is 97.4, blood pressure 98/58, pulse 108, and respiratory rate is 16 wit a pulse-ox of 98% on room air. Eyes are anicteric. Oropharynx is moist. Lungs are clear. Abdomen is soft and non-tender, but the back has right-sided CVA tenderness. The remainder of the exam is normal.