Time to choose best management solution.
A 64-year-old female with a history of CML on active chemotherapy presents as a stroke code for acute right-sided facial droop. She keeps telling everyone that what really bothers her is an incredible burning on her left flank. The stroke workup is negative. Upon inspection of her left flank, you find a vesicular rash along a single dermatome. What is the next best step in management?
- Admit with IV acyclovir and prednisone
- Admit with IV prednisone
- Discharge with PO acyclovir
- Discharge with PO acyclovir and prednisone
- Discharge with PO prednisone
Correct answer:
- Admit with IV acyclovir and prednisone
The patient is presenting with Ramsay Hunt syndrome as part of disseminated herpes zoster (shingles). Shingles is caused by the reactivation of the varicella zoster virus (VZV). Primary infection with VZV presents as varicella (chickenpox).
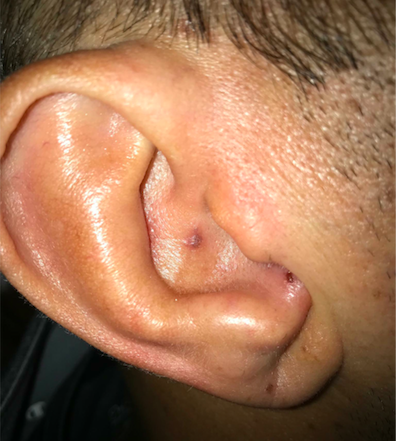
Ramsay Hunt syndrome is a herpes zoster infection of the geniculate ganglion, and is commonly associated with a facial nerve palsy, as presented here. If paralysis presents prior to onset of the vesicular rash, this syndrome can be indistinguishable from Bell’s palsy. Additional symptoms can help the physician distinguish Ramsay Hunt syndrome from Bell’s palsy, including severe facial pain or a vesicular rash. Cranial nerve VIII may also be involved, and can cause nausea, hearing loss and vertigo. The photo shows an example of auricular vesicles seen in Ramsay Hunt. Even without seeing the auricular vesicles, the facial nerve palsy should clue the physician in to concern for Ramsay Hunt syndrome due to disseminated zoster. This patient is undergoing active chemotherapy, which puts her at higher risk for disseminated zoster. Disseminated zoster requires admission for IV acyclovir and can be aided by steroids. Since she is already immunocompromised, an argument can be made against prednisone; however, without question she needs IV acyclovir.
Incorrect answers:
Without putting together the pieces of disseminated zoster, this case can be confused as the patient having both Bell’s palsy and shingles. Whereas the mainstay of therapy for Bell’s palsy is steroids, the mainstay of therapy for shingles is both antivirals (usually acyclovir) and steroids.
It would be an unusual combination of events for the patient to present with classic Bell’s palsy and classic shingles, and is much better explained by disseminated zoster, making admission with only steroids (Choice 2) incorrect.
Although patients with uncomplicated zoster can be discharged with antivirals (potentially even if immunocompromised if they have close follow up), this patient should not be discharged (Choices 3, 4, and 5) because the zoster is disseminated. That said, treatment with only acyclovir (Choice 3) would be appropriate for local zoster and treatment with only prednisone (Choice 5) would be reasonable for uncomplicated Bell’s palsy. Giving both acyclovir and prednisone (Choice 4) would be equally reasonable for both conditions, since the literature is currently debated.
References:
Gupta N, Andrus P. Ch 172: Acute Peripheral Neurologic Disorders. In: Tintinalli JE, Stapczynski J, Ma O, Yealy DM, Meckler GD, Cline DM. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 9e New York, NY: McGraw-Hill.
Stankus SJ, Dlugopolski M, Packer D. Management of Herpes Zoster (Shingles) and Postherpetic Neuralgia. Am Fam Phys. 2000; 61(8):2437-2444.
Somasundara D and Sullivan F. Management of Bell’s palsy. Aust Presc. 2017; 40(3): 94–97.