You’ve got a seemingly straightforward complaint. Should you reach for your Foley or your ultrasound probe?
Nothing is as it seems tonight. That super sweet grandma who just checked into triage just tried to stab one of your nurses in the eye with her knitting needles. The muscular gentleman with tattoos all over his face and scalp surprised most of your staff when he started howling like a baby in the midst of a digital block. Your third patient seems relatively straightforward at least. He is an otherwise healthy 65-year-old male who presents with a chief complaint of “I can’t pee”.
You sign up for the patient on your computer, read quickly through his chart, and wheel in your trusty ultrasound machine since you have a sneaking suspicion a point of care ultrasound (POCUS) is going to be quite useful. On quick review of the chart, you note that he is slightly tachycardic with a normal blood pressure, respiratory rate, oxygen saturation, and temperature. He denied any past medical history, surgical history, or medications to your triage team, and there doesn’t appear to be any prior visits to your facility noted in his records.
Entering the room, you see sitting in front of you a stoic gentleman who appears his stated age. His nurse is just finishing up the peripheral IV start and rainbow of blood collection tubes that were ordered in triage. The patient actually seems genuinely happy to see you when you shake his hand and introduce yourself. “Doc, I hope you can help me tonight. I can’t really figure out what is going on…” You notice he grimaces slightly as he repositions himself for your evaluation. “For the past two days, it has just been getting harder and harder to pee” he says. “I feel like I have to go, but only a little bit comes out each time. I’m a detective by trade, and I’m befuddled by my own case” he jokes. It sounds like your patient has done his fair share of internet browsing prior to coming into the ED and he tells you that none of the stuff he’s read online really fits his condition.
As he continues to elaborate on his history, your brain automatically starts working through a broad differential of potentially emergent and urgent etiologies for his chief complaint. Simultaneously, you power up your ultrasound machine and enter in the requisite information required for saving, archiving, and billing for your point of care ultrasound. You continue eliciting key elements of his history and then explain to him that you will be performing a point-of-care ultrasound as part of his evaluation in the ED tonight. “As emergency physicians, we’re sort of detectives, also,” you state with a grin. “We have to sort through a myriad of clues and piece together complex information in order to solve each case that comes through our doors. This scan is going to give me some important ‘inside’ information – literally.”
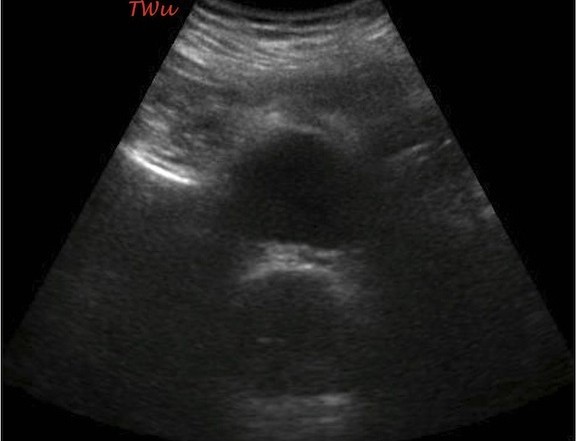
You have seemingly won him over just as your nurse comes back into the room with a urinary catheter and leg bag kit. You ignore the less-than-thrilled look he has on his face and focus on obtaining some ultrasound images and clips of his bladder and both of his kidneys (Images 1, 2, and 3).

Image 1: Transabdominal ultrasound of the urinary bladder

Image 2: Ultrasound of the right kidney

Image 3: Ultrasound of the left kidney
What do you see on the ultrasound images above? What should your nurse do with that urinary catheter and leg bag? What’s your diagnosis?
Obstruction Found, Foley Averted
As part of the differential diagnosis for this patient, you (and probably everyone else in the department) considered urinary retention as the most likely diagnosis given his age and chief complaint. The bedside bladder ultrasound you performed immediately ruled out that diagnosis given the small, almost empty bladder that was visualized (Image 4).
As you scanned through his kidneys, the patient provided you with more pertinent information regarding his case. It sounds like he is having dysuria and oliguria, but has been trying to go to the bathroom every hour or so because he feels some urgency to void. You obtain images of his kidneys and you notice that both kidneys have moderate hydronephrosis and, oddly enough, both also have large hyperechoic calculi near the ureteropelvic junction (UPJ) (Image 5).
Your deductions are supported with the hematuria noted on his urinalysis and bump in his creatinine on the basic metabolic panel ordered from triage. With all of your data now readily available, you explain to your patient how rare his diagnosis is and why he probably couldn’t find the right answer reading through blogs and advice columns online. He is happy you have solved his case, and even happier he doesn’t have to have that urinary catheter inserted.
You admit him to internal medicine with urology consultation and marvel at just how useful clinical ultrasound has become in your daily practice. The patient shakes your hand one last time on the way upstairs to thank you for your good work. You just can’t resist the urge to leave him with a parting thought “Like a famous detective once said, ‘It is my business to know what other people don’t know…I was just doing my job.’ Case closed.”

Image 4: Transabdominal ultrasound demonstrating an almost empty bladder

Image 5: Left kidney ultrasound demonstrating an obstructive UPJ stone
Pearls and Pitfalls for Ultrasound of the Bladder and Kidneys
1. Use it: Bedside ultrasound, also known as clinical ultrasound or point-of-care ultrasound (POCUS) can be used as a tool to help expedite diagnosis and improve patient care. Use it during the initial evaluation of your patients to help guide your management and treatment plans.
2. Getting started: Remember that lower frequency probes allow you to visualize deeper structures (at the expense of resolution). For most bladder and renal ultrasounds, choose a low frequency curvilinear or phased array transducer. The smaller footprint of the phased array transducer allows you to get in between the ribs for an unobstructed view of the kidneys bilaterally.
3. Start simple: A quick look at the urinary bladder can provide you with a wealth of information. Is your patient obstructed? What is the post-void residual? Is there an obvious cause for their urinary complaint? Point-of-care ultrasound can be used to diagnose urinary retention, intraluminal bladder masses, debris, stones, and foreign bodies. You can also visualize the area immediately surrounding the bladder for external causes of obstruction such as masses, an enlarged prostate, an enlarged uterus, etc.
4. Calculating volume: Bladder volume can be calculated quickly at the bedside. A post-void residual bladder volume should be measured immediately after the patient completes a spontaneous void. Remember that the bladder is not a simple structure like a sphere or cube. Its trigone shape makes calculations a bit more mathematically intriguing. To estimate the bladder volume, measure the bladder diameter in 3 planes (height, width, depth) and divide the product of these 3 measurements by 2. Bladder volume = A x B x C/2, or A x B x C x 0.5 where A, B and C are the height, width and depth. A normal post-void residual urine should be less than 50-100ml. Be aware that some experts recommend different formulas for estimating volume with values up to A x B x C x 0.75. Many ultrasound machines will have preset formulas and programs that estimate bladder volume for you. Simply enter the height, width, and depth measurements you obtained, and the computer will calculate the volume in mL’s for you.
5. Look upstream: Once you have assessed the bladder, evaluate both kidneys for potential abnormalities. Hydronephrosis will be seen as a black, anechoic area of dilation within the renal pelvis and calyces. As the obstruction worsens, the anechoic areas increase in size and the calyces and pyramids begin to compress the surrounding echogenic renal parenchyma and cortex. Image 5 demonstrates moderate hydronephrosis where the area just proximal to the white renal stone is dilated and filled with black, anechoic urine.
6. Be thorough: Evaluate the entire target organ or structure using a fanning motion. You may need to move your probe up and down a couple of interspaces during the scan. If you have a difficult time viewing either kidney, have the patient take a deep breath and then halt their inspiration. This brings both kidneys inferiorly. Obtain both long-axis and short-axis views of both kidneys and don’t stop just because you find an abnormality. Sometimes the culprit causing the obstruction can be seen on your clinical ultrasound.
7. Compare sides: Because most people have two kidneys, any questionable findings on one side can benefit from a comparison view of the other kidney. Although uncommon, patients can present with bilateral obstructing renal stones like our patient in this case. If your patient has bilateral hydronephrosis and you don’t see obvious bilateral obstructing stones at the UPJ, consider other causes besides kidney stones: bladder outlet obstruction, bladder cancer or large intravesicular clots, valvular disease and reflux, or compression of the bilateral ureters by pregnancy, a mass, or intraperitoneal abnormalities. It is important to remember that it is often very difficult to find and evaluate the ureters on ultrasound.
8. Be consistent: If your hospital and institution has not developed and implemented a formal protocol and policy for clinical or point of care ultrasounds, this is the time to do it. Work together to develop a toolkit that includes your ultrasound program goals, quality management, scope of practice for your practitioners, training and proficiency, emergency ultrasound director and leadership, delineation of privileges, professional practice evaluation, equipment selection, maintenance and cleaning, coding and documentation, financial impact, and available resource documents from ACEP, AIUM, etc.