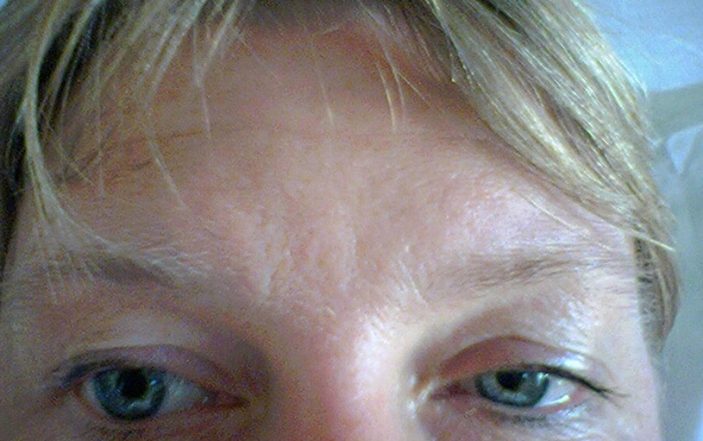
A previously healthy 42-year-old female presents to the Emergency Department the day after being rear ended while at a stop light. She is complaining of headache and left sided neck pain. She has no midline neck tenderness and non contrast CT scan of the head and cervical spine are negative. On exam you notice the following and confirm that she has her baseline visual acuity. What is the next appropriate step in workup and diagnosis?
A. CT angiogram of the brain to evaluate for a posterior communicating artery aneurysm
B. CT angiogram of the neck to evaluate for carotid dissection
C. CT orbits and facial bones to evaluate for fracture and extraocular muscle entrapment
D. Lumbar puncture to rule out subarachnoid hemorrhage
E. MRI brain to evaluate for acute CVA
Correct answer: (B). CT angiogram to evaluate for a carotid dissection
This patient is demonstrating Horner’s Syndrome (ptosis, miosis and anhidrosis), which is caused by a lesion compressing the sympathetic nerve pathway to the eye. After a trauma, and in the setting of neck pain, this is concerning for a carotid dissection. Horner’s may also be caused by CVA, tumor, herpes zoster and direct trauma. In children, the differential includes neuroblastoma, lymphoma and metastatic malignancy.
Incorrect answer choices:
CT angiogram of the brain to look for a posterior communicating artery aneurysm (Choice A) is incorrect given the patient’s clinical presentation with Horner’s. If the patient presents with acute cranial nerve 3 palsy and ipsilateral mydriasis, this is a PCA aneurysm until proven otherwise. Headache is often present as well, and treatment includes emergent blood pressure lowering if hypertensive, neuroimaging and neurosurgical consultation.
A CT of the orbits and facial bones is reasonable in an MVC with concern for facial trauma including orbital wall fractures, however this patient’s findings are not consistent with facial trauma (atraumatic face) and the external exam is not consistent with entrapped extraocular muscles (would not cause ptosis or pupil changes) as can occur with orbital wall fractures.
Lumbar puncture to rule out subarachnoid hemorrhage (Choice D) is not the best answer in this scenario. Traumatic subarachnoid hemorrhages would present with post traumatic headache, and CT is a sufficient screening exam (in contrast to the need for LP to fully evaluate spontaneous SAH). Spontaneous subarachnoid hemorrhage secondary to ruptured aneurysms (which must be considered here since it is the day after the accident) presents as sudden onset, severe headache, often posteriorly and sometimes associated with neurological deficits.
Most will show up on a non-contrast CT if the patient presents within six hours. As time goes by, the sensitivity of CT goes down and lumbar puncture may be required to evaluate for xanthochromia if clinical suspicion remains high. Horner’s would also not be a typical presentation.
MRI brain to evaluate acute CVA (Choice E) is not the best choice in this patient with post traumatic Horner’s. Though Horner’s may be caused by CVA, since this patient presents with neck pain and recent trauma, and without other neurologic deficits or risk factors, a carotid dissection is a more likely etiology for the Horner’s, and workup for this should be pursued first.
References:
Walker, Richard A and Adhikari, Srikar. Chapter 241: Eye Emergencies. In: Tintinalli JE, Stapczynski J, Ma O, Yealy DM, Meckler GD, Cline DM. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e New York, NY: McGraw-Hill; 2016.