Your patient is a previously healthy five-month-old infant who arrived following a brief generalized seizure associated with the recent onset of fever.
Because he is too young (< 6 months) to fit the diagnosis of presumed simple febrile seizure, diagnostic studies and intravenous access are indicated prior to admission for observation. Unfortunately, the ED nurses failed on numerous attempts on this pudgy baby and, well, you’re up.
You recently attended a Point-of-Care Ultrasound course in the hope that it might provide useful skills. One portion of the class involved the use of ultrasound for guidance in intravenous access and you ended up successfully inserting numerous lines on the commercial phantoms constructed for that purpose.
Using an artificial-sugar-flavored pacifier to help calm the infant, you sonographically survey both forearms. Fortunately, you are able to identify an intact forearm vein that is long and straight. On transverse view it is round and easily compressible with no interfering structures.
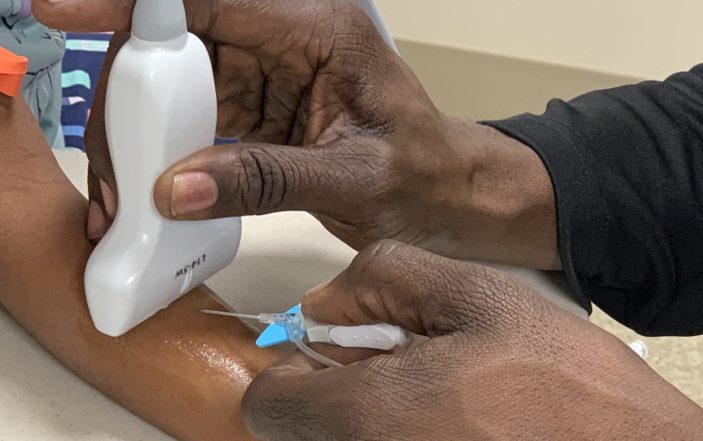
You hold the ultrasound probe perpendicular to the long-axis of the target vein ahead of the skin-entry point and slowly advance the IV device until you visualize the needle tip on your ultrasound screen. Seeing the target vessel below, you “pull” the probe further ahead of the needle with one hand and then advance the needle by “pushing” it further with your other hand until you see the tip appear once again.
Following a couple more cycles of this you can now see the needle tip immediately above the “near-wall” of the target vein. Just as you were taught in class, you gently “bounce” the needle tip against the target vein and ensure you are well-centered prior to attempting vessel entry.
Using slightly more force you puncture the near wall of the vein and observe immediate recoil of the target vessel. You remember that you were told to keep your eyes on the ultrasound screen, so you ask your nurse whether he sees a flashback in the intravenous needle hub. He does.

Next is the threading of the catheter over the needle. This is the part of the procedure where failure often occurs. You carefully rotate the probe 90 degrees to an in-plane orientation in order to better determine whether the catheter is also within the vessel. Your course teacher emphasized that it is possible to get a flashback with only the needle tip and not the catheter within the target vessel lumen, providing false assurance of intraluminal positioning of the catheter.
You proceed to advance the intravenous device a little further while observing the ultrasound screen presenting an in-plane view. A teaching pearl from your class suggested that sonographic visualization of the proximal portion of the needle tip bevel within the vessel lumen was a pre-requisite to attempts to thread the catheter. The catheter now enters the lumen while you narrowly avoid hitting the back-wall of the vein with the needle tip.
“This is what they warned us about…now we need to lower the angle of entry while not pulling the catheter out of the lumen.” You gently lower the base of the intravenous device toward the skin, slightly reducing the angle of incidence. “Is the catheter still in?” Yes it is, but you should not lower it any further if you want to avoid pulling the catheter out. You, once again, attempt to gently advance the catheter over the needle while remaining focused on the ultrasound unit screen. You observe its advance within the lumen while you appreciate little resistance. “I think we did it.”
Key Teaching Points: Ultrasound-Guided Peripheral Intravenous Vascular Access
- Difficulty in establishing vascular access is an unfortunate and all-too-common occurrence in the emergency medicine. Traditional technique that employs anatomic landmarks and palpation, although usually successful, may be ineffective in the presence of obesity and dehydration, as well as in pediatric patients. Virtually all providers have “been there” in regard to numerous unsuccessful attempts at intravenous access resulting in traumatized children and frustrated parents.
- A competing issue in the emergency department is “time.” Although the use of ultrasound guidance for vascular access saves time when compared to numerous unsuccessful blinded attempts, it is still usually more time-consuming than one successful non-ultrasound attempt. The “hassle-factor” involved in moving the ultrasound unit to the patient, locating a trained sonographer, and a time-consuming sonographic search for a suitable target vessel often doesn’t seem “worth it” for busy caregivers who are usually successful with their initial blind technique. Wise judgement on the front-end is absolutely essential.
- Terminology utilized in the discussion of ultrasound-guided intravenous is foundational. In-plane refers to an insertion technique where the length of the high-frequency ultrasound probe is oriented along the long-axis of the target vessel. Out-of-plane refers to a technique where the length of the probe is positioned perpendicular to the target vessel. In the former, the operator’s initial goal is to achieve co-linearity between the probe and the target vein. In the latter, the target vein is approached in cross-section and will have a round appearance. Each technique has its own unique advantages and weaknesses.
- In-plane technique is considered by many to be the most sophisticated and, when possible, is preferable as it can provide visualization of the entirety of the target vessel as well as the approaching intravenous stylet and catheter. It does, however, require considerable operator skill to achieve and maintain co-linearity between probe and target vessel throughout the length of the target vein while simultaneously advancing the intravenous device in that same plane (“tri-linearity”). This technique can be challenging for the novice sonographer for a number of reasons. First, the ultrasound beam is the thickness of a credit card and, therefore, remaining perfectly “in-plane” can be a challenge on a wiggling child. Moreover, in-plane technique is most easily performed in vessels that are both long and straight—conditions not always present in infants and small children.
- Out-of-plane technique intends to maintain focus on the intravenous device’s needle tip as it enters the plane of the ultrasound beam oriented horizontally to the target vein. The application of Euclidian geometry intends to determine the precise skin to target vessel distance and its discussion is often part of the orientation to out-of-plane technique and can provide an estimate of where the probe will be positioned on the patient’s skin to visualize needle contact of the near wall of the target vein (Figure 5).
- The initial sonographic survey for a desirable target vessel is of critical importance. Scanning often begins with the ultrasound probe oriented in transverse axis to the extremity being assessed to identify and distinguish possible target veins from other structures. Optimal veins are identified as hypoechoic, round, easily compressible, and at least three times the diameter of the intended intravenous catheter. The easy compressibility in response to probe pressure helps distinguish a vein from a less compressible artery (Figure 6), while Color Doppler flow characteristics can also assist in distinguishing the two. Increased target vein depth (> 1.5 – 2 cm) may be associated with less success and reduced intravenous device longevity, as it is often associated with proportionately less catheter residing within the target vessel. Additional sonographic interrogation should survey the length of the candidate vein to ensure reasonable linearity allowing for non-traumatic catheter advancement.
- Out-of-plane technique can be described further as “push-pull” or “pull-push.” Both are out-of-plane strategies that involve periodic sonographic surveillance of the needle-tip along its path to the target vessel. In “pull-push” technique, the ultrasound probe is advanced slightly (“pulled”) along the trajectory of the target vessel in advance of the needle-tip. When subsequent advancement “push” of the needle-tip “catches up” to the probe, additional subtle advancement “pull” of the probe can continue. In this manner, the “pull-push” technique attempts to ensure constant operator awareness of needle tip location relative to the target vessel throughout the needle’s approach.
- When the needle tip reaches the target vessel, “tenting” of the target vessel near wall notifies the operator of the location of the needle and catheter relative to the vein and allows for “centering” of the needle tip. At this point, slightly greater pressure will allow entry of the needle through the near wall and into the target vessel
- Confirmation of the needle puncturing the target vessel occurs in two ways. First is via sonographic observation of target vessel near-wall recoil. Second is via the old-fashioned observation of a flashback of venous blood into catheter hub. As in our case scenario, this may be best accomplished by an assistant, allowing the operator to maintain visual focus on the ultrasound screen.
- The next phase involves advancing the catheter over the needle. Too steep of an angle of incidence risks “back-walling” and “blowing” of the target vein. Conversely, lowering the angle of needle entry to avoid “back-walling” risks the opposite–withdrawing the intravenous catheter from the lumen of the vein through the near-wall. The margin for error at this critical juncture can be small while sonographic confirmation of appropriate position is very helpful prior to attempts to thread the catheter. This is where in-plane technique is useful, as direct observation of catheter advancement over the entry needle can occur.
Although requiring practice and patience, the acquisition of skill in ultrasound-guided peripheral venous access is both rewarding and well-appreciated by families, patients and staff.