EMS presents a 47-year-old male with sudden eye pain and decreased visual acuity which occurred while he was putting drops into his left eye. While he was retracting his lids to place the drops, his eye “popped out” with sudden subluxation of the globe.
The patient immediately called 9-1-1 and on arrival, EMS placed a saline-soaked gauze over his left eye. The patient was transported to the emergency department without any complications. His past medical history was notable for a history of prostate cancer, with metastatic disease to the sphenoid bone and globe involvement in his left eye. He had resultant glaucoma in his left eye, which he was treating topically at the time of the event. On initial exam, he had obvious globe subluxation (image 1), was unable to move the eye, with both superior and inferior lids retracted behind the globe. A central corneal abrasion was demonstrated and he only had light perception.

image 1 Globe subluxation
Ophthalmology was immediately consulted, however given the loss of vision, presumably from traction-related optic neuropathy, and expected delay in arrival of the ophthalmologist, the globe was immediately reduced by the treating emergency physicians. After placement of topical proparacaine, gentle alternating pressure was performed on the upper, then lower sclera, while another physician attempted to manually retract the upper and lower lids from behind the globe. While applying gentle downward pressure to the top of the globe, the patient was asked to look up, then down, and the globe gradually reduced. The patient had near immediate relief of pain and return of near baseline visual acuity. He was examined in the ED by ophthalmology after reposition of the globe, and was followed up the following day, primarily because of a large central corneal abrasion. He recovered without sequela.
Globe Subluxation/Luxation
Globe subluxation is an anterior displacement of the eye, out of the orbit, typically with protrusion of the equator of the globe beyond retracted lids. It is rare –there are less than 30 spontaneous cases reported in the literature. However, given that it likely occurs most frequently in physicians offices, during examinations, and the globe will typically spontaneously reduce with manipulation of the eyelid, it is likely very under-reported.

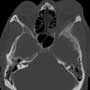
image 2 CT orbit demonstrating irregular osteoblastic lesion of the left sphenotemporal region, proptosis of the orbit and medial displacement of the lateral rectus muscle
Clinical Presentation
When a globe subluxation presents to the emergency department, it is an obvious, dramatic, and very anxiety provoking event. The diagnosis is rarely in question. Symptoms can vary from asymptomatic, to pain and blurred vision, to blindness secondary to traumatic optic neuropathy. Reported complications include exposure keratopathy and corneal abrasion, as occurred in this case, and typically blepharospasm. Traumatic optic neuropathy is sometimes observed. Globe subluxation has been classified into three categories: spontaneous; voluntary; or traumatic. The majority are spontaneous, occurring without conscious effort, but often with a precipitating factor (putting in drops, contacts, manipulation of lids during and exam), triggering the subluxation. Voluntary globe subluxation occurs when a person is able to express one’s globe without any precipitating trigger. Traumatic globe subluxation occurs after direct trauma.
Pathophysiology
Usually a patient or a caregiver will manually spread the eyelids, causing posterior pressure against the globe. As the globe advances, the cornea can become dry, inducing a blink reflex. This causes contraction of the orbicularis muscle causing the eye to sublux. Other triggers include coughing, vomiting, straining, or other valsalva-like maneuvers, as well as extremes of gaze. Risk factors for globe subluxation include underlying exophthalmos, severe lid retraction, floppy eyelid syndrome, orbital infiltrative diseases (such as thyroid orbitopathy) or conditions that predispose patients to shallow orbits. This patient had orbital involvement of metastatic prostate cancer, causing baseline exopathalmos, which put him at risk for the globe subluxation. Although the orbit is an uncommon site for prostate cancer to metastasize, prostate cancer is probably the 3rd most common cancer to cause orbital metastases (behind breast and lung, causing about 4-10% of all orbital metastases. However the orbit (figure 3) is an uncommon site for metastases in general (2-9% of all metastastic disease).
Treatment
Acutely, treatment requires immediate reduction of the globe. Sometimes, patients who have had prior globe subluxation know how to reduce the globe when it subluxes again. As globe subluxation is often iatrogenic, occurring during eye examinations, many patients will often have been reduced in the office and not present to the ED. Patients who present to ED typically have a longer time of subluxation, promoting more obicularis muscle spasm, and have some degree of exposure keratitis, promoting further blephorspasm, making reduction more difficult. Topical anesthetic drops should be used to break the exposure/dry-eye cycle and decrease blepharospasm, allowing the emergency physician to more easily digitally reposition the globe. Sometimes systemic sedation may be required. Manual reduction involves gentle pressure on the globe, pressing on the sclera, and avoiding the cornea, while manipulating the eyelids anteriorly, from behind the globe. One maneuver to reduce a subluxed globe, which patients are sometimes instructed to do at home, involves having the patient maintain a downward gaze, while one hand pulls the upper eyelid upward over the globe while the globe is simultaneously pressed posterior and inferior, with the index finger of the other hand on the superior sclera. The patient is then instructed to look upwards. Another method involves using a Desmarres retractor or a paper clip, bent at a right angle, introduced between the upper lid margin and superior rectus, avoiding the globe. Once the tip is under the eyelid, downward digital pressure is applied. Once the eyelid is over the equator of the globe, the patient is instructed to look up, pulling the eyelid over the eye. Sedation is sometimes necessary to perform the maneuver. In addition, a facial nerve block to relax the orbicularis muscle has been described. Rarely, conscious sedation and even general anesthesia may be necessary, especially in children and mentally handicapped individuals.
Patients who have had a subluxed globe should be educated on potential triggers for recurrent subluxation, particularly lid manipulation, and should be referred to investigate and treat underlying predisposing conditions such as associated with thyroid disease producing exophthalmos or other infiltrative conditions of the orbit, as occurred in this patient. Patient should be instructed on proper repositioning techniques as discussed above. Rarely, ophthalmologists will perform surgical interventions in recurrent cases.
REFERENCES
1. Kunesh JC, Katz SE. A Spontaneous Globe Luxation Associated with Contact Lens Placement. The CLAO Journal 2002; 28: 2-4.
2. Tse, DT. A Simple Maneuver to Reposit a Subluxed Globe. Arch Opthalmol 2000; 18: 410-411.

1 Comment
Very informative article, thank you