Taking a methodical approach to the medical resuscitation of a critically-ill patient.
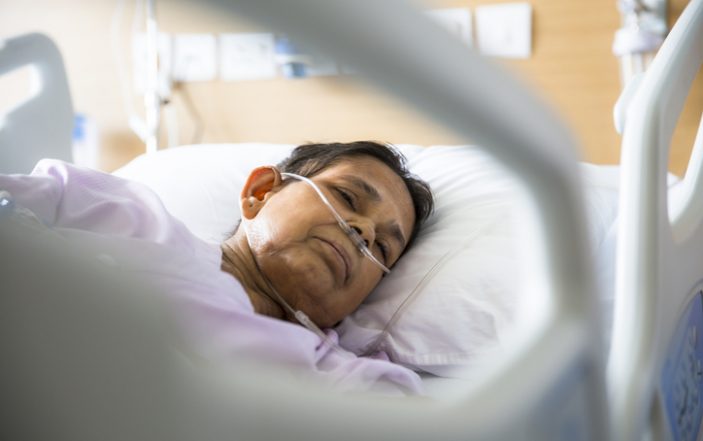
A 78-year-old woman presented to the Emergency Department via medics. The patient had baseline dementia, and medics were uncertain of her mental status baseline. On arrival, the patient was hypothermic, hypotensive, and hypoxic; no medications or fluids were given during transport. On initial exam, the patient had dry mucosa, pulmonary rales, and was obtunded with a non-focal neurologic examination.
Presenting vital signs: Temp 32.8C (91F) rectal, HR 77, BP 66/36, RR 24, O2 85% on 15L non-rebreather. Point of care glucose 212.
Medical Decision Making
This case is an example of how real-life critical resuscitation decisions are made with unknown and/or incomplete data. As the case progresses, only the information that was available to the medical team at the time of decision-making will be presented.
Both the attending and the resident physicians swiftly recognized that the patient was critically ill, and needed immediate lifesaving measures. The first decision discussed was:
When to Intubate?
With such profound hypotension and a mean arterial pressure in the 40s, rushing to intubate would likely decrease preload to the point of risking peri-intubation cardiac arrest (PICA). Paralytics and the associated loss of sympathetic tone would also make early intubation hazardous. Therefore, the team decided to bolus two liters of normal saline, obtain central venous access, and begin vasopressor support prior to intubation.
The literature supports this “resuscitate before you intubate” mantra. The combination of positive pressure ventilation decreasing venous return and paralytics causing a loss of sympathetic tone predispose to PICA. Inadequate ventilation after intubation worsens acidosis and can also contribute to further decompensation.
Pulseless electrical activity progressing to asystole is the most common reported rhythm in fatal PICA.[1] Anesthesiology reports that PICA occurs in 0.02 – 0.05% of intubations. Reflecting the different patient population, up to 4% of intubations in the Emergency Department are complicated by PICA.[2] The ICU rate of PICA is reported to be approximately 2.5%.[3] The Shock Index (heart rate / systolic blood pressure) is a quick tool to assess the risk of PICA. Every 0.1% increase in Shock Index increases the odds of cardiac arrest 1.16 times. In short, “resuscitate before you intubate” is backed by significant evidence.
The recognition of a patient who is extremely high risk for PICA and the delay in intubation was the first decision point that avoided a fatal mistake. She responded well to fluids and vasopressors, and central access was quickly obtained.
The next decision discussed was:

Which Rapid Sequence Intubation (RSI) Meds are Best?
Several options were discussed at bedside. Benzodiazepines and propofol were quickly due to the likelihood of persistent hypotension leading to PICA. Another potential option was etomidate and succinylcholine; a rapidly acting combination that would not leave the patient with loss of sympathetic tone for an extended period of time, and a familiar regimen used by most emergency physicians.
However, etomidate can cause adrenal suppression in profoundly septic patients, and sepsis seemed likely in this case. The elevation in serum potassium that succinylcholine can cause was also concerning. The patient had dementia but it was unknown if she was bedridden or had a history of stroke. Her initial EKG demonstrated a wide QRS complex; concerned about potential hyperkalemia, succinylcholine was dismissed.
The team instead chose ketamine and rocuronium. Ketamine guards against PICA by recruiting catecholamines that were not previously depleted by septic compensation. Rocuronium avoided the risk of hyperkalemia as it is a non-depolarizing agent; losing a neurologic examination for about one hour was discussed, but seemed justified to avoid PICA.
Clinical scenarios vary too widely for a clear consensus on which RSI medications are indicated for each patient. Emergency physicians must therefore be familiar with all modalities and classes of medications used in airway management. The article by Allen et. al. is a concise review of many RSI medications and includes mechanism of action, route, dosing, adverse effects, and contraindications.[4]
The patient was given ketamine and rocuronium with successful endotracheal intubation via direct laryngoscopy and PICA was avoided. When lab results became available, the next decision was:

Which Fluids to Resuscitate?
The team assessed that in addition to profound hypotension from hypovolemia, the patient was likely septic and also in distributive shock. This was complicated by profound electrolyte derangements (see Table 1), with a free water deficit calculated as 5.3 L. With two liters of normal saline fluid already bolused, the team discussed fluid selection. The first option was to continue normal saline, providing 154 mEq of sodium per liter.
Another option considered was lactated ringer’s (LR) solution, with 132 mEq sodium as well as bicarbonate and potassium. The team considered the risk of cerebral edema associated with decreasing sodium too quickly as well as adding to total body potassium in a patient with extreme hyperkalemia and compromised renal function. Ultimately a bicarbonate drip was selected due to the profound acidosis and hyperkalemia.
The BICAR-ICU Trial published in 2018 attempted to assess whether a sodium bicarbonate infusion in patients with metabolic acidosis had an effect on mortality. At the 28 day endpoint, there was no clinical difference in the bicarbonate group compared to the control group.[6] However, the SALT-ED Trial published in March 2018 compared the clinical effects of balanced crystalloids versus normal saline in non-critically ill patients that were not in an intensive care unit. The balanced crystalloids had a lower incidence of acute kidney injury within 30 days as compared to the normal saline group.
Although the non-critical SALT-ED Trial study population does not directly match our critically ill patient, it does speak to renal physiology and lend support to the effect of worsening metabolic acidosis with normal saline.[7]
At the same time the SALT-ED Trial was being run, any patients that were deemed critically ill and needing ICU level care were enrolled into a study with a similar concept called the SMART Trial. SMART found that at hospital discharge or 30 days (whichever occurred first) the balanced crystalloid group had a lower rate of death, new renal replacement therapy, or persistent renal dysfunction when compared to the normal saline group. This suggests that balanced solutions may be safer than normal saline for critically ill patients.[8]
The Free Open Access Medical education (FOAMed) resource, PulmCrit, also published an article prompted by the release of these studies. It outlines several theories to support the use of balanced crystalloids rather than normal saline and describes some of the associated physiology.[9] While this is a fantastic article, it focuses on lactated ringer’s solution and normal saline, but does not discuss sodium bicarbonate boluses or drips.
The critically-ill elderly female with severe metabolic acidosis, hypernatremia, and hyperkalemia needed fluid resuscitation and safe correction of her electrolytes. The fluid selection was even more important given her tenuous hemodynamics and the extent of her new kidney injury. The team discontinued further normal saline to avoid worsening metabolic acidosis and its associated potassium shifts. LR was deferred since it would have added to the total body potassium and corrected sodium too quickly. A sodium bicarbonate drip was initiated to help begin correcting all the electrolyte derangements until dialysis could be arranged.

Discussion:
Ultimately the patient was transported to the ICU where she remained intubated for over one week. She underwent continuous renal replacement therapy and was then transitioned to intermittent hemodialysis.
After approximately two weeks in the hospital, she was discharged back to the nursing home with a G-tube and on hospice status. Unfortunately, she never returned to baseline mental status and passed away less than two months after returning to the nursing home.
The case represents a not uncommon occurrence in a typical Emergency Department. When patients are unable to provide a history and the ideal data set is not readily available, slowing down to make careful weighted decisions becomes imperative. The critical nature of the patient was identified early, but only the carefully coordinated decision making ultimately overcame her perilous physiology.
REFERENCES:
- Self, M. and Wardi, G., 2021. “Peri-Intubation Cardiac Arrest: New Insights into an Uncommon and Potentially Preventable Cause of Mortality in Critically Ill Patients.” [online]Acep.org. Available at: <https://www.acep.org/how-we-serve/sections/critical-care-medicine/news/july-2018/peri-intubation-cardiac-arrest-new-insights-into-an-uncommon-and-potentially-preventable-cause-of-mortality-in-critically-ill-patients/> [Accessed 30 April 2021].
- Heffner AC, Swords DS, Neale MN, et al. “Incidence and factors associated with cardiac arrest complicating emergency airway management.” Resuscitation. 2013 Nov; 84(11):1500–4.
- Wardi G, Villar J, Nguyen T, et al. “Factors and outcomes associated with inpatient cardiac arrest following emergent endotracheal intubation.” Resuscitation. 2017 Dec; 121:76-80.
- Kaminsky M, Malesker M, et al. “Evaluation of the Effects of Etomidate for Induction with Mechanical Ventilation in Patients with Sepsis: A Retrospective Analysis.” Chest. 2020; 10.1016/j.chest.2020.08.642.
- Allen P, Desai NM, Lawrence VN. “Tracheal Intubation Medications.” [Updated 2021 Jan 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507812/
- Jaber, Samir, et al. “Sodium Bicarbonate Therapy for Patients with Sever Metabolic Acidaemia in the Intensive Care Unit (BICAR-ICU): A Multicentre, Open-Label, Randomised Controlled, Phase 3 Trial.” The Lancet, vol. 392, no. 10141, 2018, pp. 31 – 40. Crossref, doi: 10.1016/s0140-6736(18)31080-8.
- Self WH, et al. “Balanced crystalloids versus saline in noncritically ill adults”. The New England Journal of Medicine. 2018. 378(10):819-828.
- Semler MW, et al. “Balanced Crystalloids versus Saline in Critically Ill Adults”. The New England Journal of Medicine. 2018. 378(9):829-839.
- Farkas, Josh. “PulmCrit – Get SMART: Nine Reasons to Quit Using Normal Saline for Resuscitation.” EMCrit Project, 27 Feb 2018, emcrit.org/pulmcrit/smart

4 Comments
Nice review of DSI (delayed sequence intubation). Good job!
I work in the ED in rural area, the patient described above is common in many rural E.Ds. This is great presentation and like the review on selection of patients for intubation and resuscitation of the patients before intubation and selection of muscle relaxants. I have given benzos only and waited for five minutes and the patient relaxed and able to intubate with no complications. Recently I started using Ketamine and this works great
I think the greatest learning point of a case like this, is how to approach each critical decision point. It is no longer “A B C” for everyone. We are more sophisticated than that, as we should be. Great case guys. Thank you for sharing it.
Thanks so much, Ed. Great to hear from you and we miss you at Wright State!