“I think it’s time we go on ambulance diversion again,” your charge nurse suggests, looking as tired and frustrated as you feel. This is the third time this week that you have had to close your ED. All of the beds in the hospital are full, and your ED is bulging at the seams with sick patients that aren’t going anywhere anytime soon. You are holding 10 admissions at the present moment, and the hallways are lined with patients calling “doctor” every time you walk by.
As much as you hate doing so, you concede to the request to close to ambulance traffic and then walk briskly over to the chart rack to see what you can do to help improve the current situation. Your eager intern is right on your heels and says he has a new patient to present to you. “This should be a really simple case,” he spurts out. You raise your eyebrows and bite your tongue.
The intern paints a story of a 40-year-old female who came into the ED today because she was feeling “under the weather”. She’s had a cough and nasal congestion on and off for the past 4 weeks. The cough has been productive of yellowish-white mucus, and the same stuff is seen running down her posterior pharynx on exam. She’s also reporting tactile fevers, chills, myalgias, and a headache. Coughing makes the headache worse, but she has no neck pain or neck stiffness, and the headache came on gradually and is not that severe. She also complains of some chest pain, and states it feels like a “sharp pain in her heart” that’s worse when she coughs. Her throat hurts, her ears ache, and just like everyone else in your ED, she thinks she has the flu.
Other than the post-nasal drainage in her throat, her only significant exam findings are some faint crackles in the left lung base and a mild pharyngitis. Your intern wants to order a chest x-ray, a flu-swab and a urine pregnancy test and provide her with some supportive therapy both in the ED and as an outpatient after she gets discharged. He recommends some IV fluids for her heart rate of 118 bpm, Tylenol for her headache and some Tessalon Perles for the cough. He doesn’t think she has strep pharyngitis based on the Centor criteria, and so he doesn’t want to test for that.
On the way to go see the patient you grab the ultrasound machine and comment, “Teaching point number one is conservation of energy. One of the best ways to be efficient is to ensure that you minimize the amount of time wasted. If you might need the ultrasound machine, take it with you so you don’t have to walk back out of the room to go get it.”
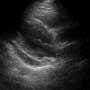
When you enter the room, you see that your intern’s presentation was pretty accurate. The poor lady looks miserable and she is sitting in the bed, hunched over her knees, coughing up some yellowish-white sputum. You wash your hands, introduce yourself, and take advantage of the moment to listen to her lung fields with her sitting upright and leaning forward. You take a quick peek at her lungs with the ultrasound machine and note that there is no obvious pneumothorax, consolidation, or pleural effusion. You have her lie back in the bed so you can perform the rest of the exam. As reported, she likely has a mild viral pharyngitis and no concerning signs for meningitis. As you are about to listen to her heart sounds, the patient asks if she can sit up because her chest feels better when she leans forward. Your Spidey-sense tells you that something isn’t quite right, so you place the phased array ultrasound transducer over her heart and obtain the following parasternal long-axis view (Image 1). What do you see? What could this be from?

You place the phased array ultrasound transducer over her heart and obtain the following parasternal long-axis view. What do you see? What could this be from? Conclusion in the following

Image 2: Parasternal long-axis view of the heart demonstrating a pericardial effusion. (RV=right ventricle, LV=left ventricle, Ao=aorta, LA=left atrium)
Dx: Not Your Typical Viral Infection
You allow the patient to remain in whatever position is most comfortable for her and begin explaining to her that you see a small collection of fluid around her heart (Image 2). She seems indifferent as you begin explaining that her viral infection could have led to pericarditis and development of a small pericardial effusion that requires further testing. “As long as you make me feel better, doc, do whatever you have to do…” she replies in between her dry, hoarse coughs.
You walk your intern through the rest of the bedside cardiac ultrasound and even though the effusion is not large, you double-check to make sure there are no signs of early tamponade physiology and no other obvious issues with the patient’s cardiac output or wall motion. You give your intern teaching point #2: “Don’t stop your evaluation just because you find something abnormal. Make sure you follow through and complete the rest of the exam or ultrasound.”

In your institution, patients with pericarditis are admitted to the hospital so you order the tests you know your internal medicine colleagues will want to have: EKG, CXR, CBC, CMP, ESR, CRP, cardiac enzymes, LDH, TSH, Free T4, HIV, and a QTB. You defer the rheumatologic and neoplastic workup and potential biopsy option to them.
As you are wrapping up your shift with your intern, you are greeted with a smile and a big thank you from the patient being wheeled upstairs for admission. With all of the influenza and viruses you have been seeing this season, you knew you would eventually come across something unexpected. You turn to your intern for your final teaching point on the case: “Being able to find that needle in a haystack is what differentiates great doctors from the rest. Then again, sometimes its just better to be lucky than good.”
************************
Tips & Tricks for Performing a Bedside Cardiac Ultrasound to Evaluate for Pericardial Effusion
01 Bedside ultrasound is the stethoscope of the future. Ultrasound is more sensitive and specific than physical exam alone in assessing for the presence of a pericardial effusion. Especially in patients where it can be difficult to determine if a pericardial friction rub or diminished heart sounds are present, perform a bedside cardiac ultrasound.
02 Use a low frequency transducer with a small footprint (e.g. a 1-5 MHz phased array transducer).
03 Place the patient in a supine or left lateral decubitus position to bring the heart anteriorly in the chest wall and closer to the probe.
04 Pericardial effusions will appear as a black or anechoic collection of fluid anterior to the descending thoracic aorta.
05 Effusions are typically categorized by the following guidelines:

06 Small effusions are generally confined to the area just posterior to the left ventricle when the patient is lying supine. For this reason, it is very important to increase the depth of your scan to evaluate the region posterior to the heart.
07 Large effusions will appear circumferentially around the heart and you may see the heart swinging in the bag of fluid with each contraction.
08 Note that loculated effusions can be seen anywhere in the pericardial space.
09 Effusions from viral infection, uremia, or recent myocardial infarction can contain fibrinous material and appear more heterogenous on bedside ultrasound.
10 When you see a pericardial effusion, determine if there is any evidence of cardiac tamponade. On ultrasound, cardiac tamponade should be suspected if you see end-diastolic right ventricular or right atrial collapse in the appropriate clinical setting. Avoid the pitfall of confusing normal right-sided systolic contraction with abnormal diastolic collapse.
11 Remember that large pleural effusions can mimic the appearance of a pericardial effusion on bedside ultrasound. Make sure you visualize the descending aorta and see how the hypoechoic fluid courses in relationship to the aorta. Pericardial effusions will be seen layering out anterior to the descending aorta (between the aorta and the heart) on a parasternal long-axis view of the heart. Pleural effusions will run posterior to the aorta on a parasternal long-axis view.