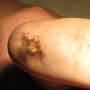
A 16-month-old female presents to your emergency department with her mother after stepping on a bare wire left plugged into a wall. The child has no past medical history and is up to date on all vaccinations. A thorough exam reveals the pictured wounds to the plantar surface of the left foot. The patient is acting appropriately, with normal vitals, and the remainder of the exam is nonfocal. What is your management of this patient?

Even before the modern age, human fascination with the power of electricity was heralded in tales of the deities Zeus and Thor wielding thunderbolts from the sky. Whether you prefer the Greek or Norse version of that myth, today’s society not only remains intrigued by electricity, but it is largely dependent upon it. However, as with all power, electricity comes with consequences. Electrical burns account for 3000 burn center admissions in the US each year, cause up to 1000 deaths annually, and comprise 3% of pediatric burns. When this electrical injury arrives in your ED, will you know how to manage it?
Pathophysiology
Severity of an electrical burn injury is dependent on many factors (see Table 1 for a review).

Direct current (DC) at high-voltages will cause a single forceful muscle contraction, often throwing the victim from the electrical source and limit the duration of exposure, but increasing the risk of traumatic injury. Alternating current (AC) is the common household current in the US and is more dangerous than DC at similar voltages because the cyclical current stimulates muscle tetany, often causing the victim to grasp the source and prolong the exposure.
ED Evaluation
Head- If the injury occurs near the head, 6% of patients may develop cataracts, immediately or delayed. Be sure to check visual acuity and fundoscopic exam. More rarely, hearing loss may occur. The most common electrical injury in patients under age 4 is an oral burn from chewing on a household cord.
Cardiovascular- Electricity can cause direct myocardial necrosis or conduction abnormalities. Cardiac arrest is rare but can occur in high-voltage injuries. Prolonged CPR should be considered in these patients since most victims are young and good outcomes have been noted even when the initial presenting rhythm is asystole. Several studies indicate that most cardiac affects present acutely and ECG and cardiac monitoring is needed only for high-voltage injuries or patients with cardiac history, symptoms, or suspicion of cardiac conduction injury. Findings on ECG can include sinus tachycardia, ST elevation, QT prolongation, PVCs, atrial fibrillation, or bundle branch block. Thrombosis of the vasculature is common secondary to heat coagulation and vessel injury and may be delayed in presentation.
Extremities- Muscle necrosis can occur, even distant from the apparent skin injury, and the resultant massive release of myoglobin may lead to renal failure. Compartment syndromes are common due to vascular compromise and muscle edema, so monitor closely for elevated pressures and perform fasciotomies as indicated. Joints often exhibit more severe injury from the concentration of heat in these areas where less muscle is present to conduct current.
Skin- The hands and skull are the most common sites of contact with the source, the heels are the most common areas of ground contact. Keep in mind that a single patient may have multiple source and ground contacts. Severity may range from mild erythema to 3rd degree burns. Dress all wounds and consider tetanus status.
Neurologic- Transient loss of consciousness, cranial nerve deficits, and seizures have been documented after electrical injury. The most serious direct neurologic effect occurs when injury to the respiratory control center results in respiratory arrest. Spinal cord injuries may result from direct transection during horizontal transmission or due to fractures and ligamentous disruptions of the spine when muscles contract forcefully during electrical injury.
Management Pearls
Algorithms for fluid resuscitation based on affected body surface area are unreliable in electrical injuries as much of the damage may be unseen. However, crystalloids should be started and maintenance of urine output to 1-1.5 mg/kg/ hr can guide fluid management. Treat pain aggressively, the extent of injury is often difficult to appreciate. No literature currently supports prophylactic use of antibiotics in these injuries.
Management of Electrical Injury
- Address airway issues
- Evaluate for trauma (FAST, CT, X-rays, labs)
- EKG or cardiac monitor if indicated
- Initiate fluid resuscitation, monitor urine output
- Evaluate for compartment syndrome, consider fasciotomy
- Consider CPK and creatinine for muscle and kidney injury
- Check visual acuity and fundoscopic exam
- Treat pain
- Dress wounds, update tetanus
- Consult burn specialist
- Transfer to trauma/ burn center as indicated
Disposition
Patients with significant burns or trauma should be stabilized and admitted or transferred to a burn center. If cardiac symptoms are present or cardiac damage is suspected, the patient should be monitored 12- 24 hours even if no other significant injuries are discovered. A victim with only cutaneous burns or mild symptoms after a low-voltage exposure can be discharged if an ECG and urinalysis are normal. All patients should be referred for close follow-up to monitor for long term sequelae. Children with low-voltage injuries likely do not need an EKG unless symptomatic. Pediatric patients with isolated oral burns can also be discharged with a vigilant adult and referrals to dentistry or surgery as indicated.
Case Outcome
Our 16-month old patient was observed in the ED for several hours. A thorough exam revealed no other injuries or signs of compartment syndrome. A burn specialist was consulted by phone and recommended cardiac monitoring in the ED for signs of arrhythmia, although her risk of cardiac injury was thought to be very low with entrance and exit wounds on the same extremity. After an uneventful observation period, she was discharged home with parents, with instructions for wound care and strong advice about the dangers of exposed wires. The patient was reportedly behaving and ambulating normally when she returned to the ED the next day for a follow-up check. No evidence of compartment syndrome, infection, or other injuries was found on examination and additional studies were deemed unnecessary. The patient returned home with her parents.
Take home
1. Evaluate thoroughly for associated traumatic injuries.
2. The visible burn may not represent the true extent of electrical injury, fluid resuscitation should be guided by urine output, not the Parkland formula.
3. High-voltage injuries or patients with cardiac symptoms require extended cardiac monitoring. Low- voltage, asymptomatic patients can be discharged after a normal ECG.
4. Check for myoglobinuria and renal failure when muscle necrosis is suspected.
*Board Exam Pearl*
Be watchful for delayed hemorrhage from the labial artery in pediatric patients with oral burns when the eschar falls off about 2-3 weeks after the initial injury.
Special Considerations
Pregnant patients require extra caution as data suggests that fetal demise can result even from low-voltage exposure, although the actual risks are unknown due to the low number of cases reported. In this population, be thorough in examining for trauma, especially for evidence of placental abruption. All patients at >24 weeks gestation should be sent for OB monitoring. Those with nonviable pregnancies should be informed of an increased chance for miscarriage and instructed in close OB follow-up. Affected women are generally placed in a “high-risk” category for the remainder of their pregnancy.
References
- Baxter CR, et al. Emergency treatment of burn injury. Ann Emerg Med 1988; 17: 1305.
- D’Souza, AL, et al. Pediatric Burn Injuries Treated in US Emergency Departments Between 1990 and 2006. Pediatrics 2009; 124: 1424-1430.
- Koumbourlis AC, et al. Electrical Injuries. Critical Care Medicine 2002; 30(11): S424-S430.
- Marx, JA, et al, ed. Rosen’s Emergency Medicine Concepts and Clinical Practice. 7th Edition. Philadelphia: Mosby Elsevier, 2010. 1893-1902. Print.
- Xenopoulos N, Movahed A, Hudson P, Reeves WC. Myocardial injury in electrocution. Am Heart J 1991; 122: 1481.