A 19-year-old man was brought by EMS after being struck by a high speed auto. The exact mechanism of injury and the site of the impact was unknown. Vital signs were normal at the scene and in the trauma room. He admitted to drinking alcohol prior to the accident, but was awake and alert and had no other major complaints aside from pain in his neck. Initial ED assessment revealed an intoxicated young man with multiple abrasions and lacerations to the body. Aside from slurred speech, the patient was neurologically intact. After completion of the primary and secondary survey he was taken for CT. Significant images are shown at right.
Neurosurgery was consulted and the patient was admitted to trauma intensive care unit.
Discussion:
Burst fracture of C1 is caused by an axial load on the occiput. Classically, Jefferson fractures (JF) have 4 fracture sites, 2 on the anterior and 2 on the posterior arches of C1, but variations, such as 2 and 3 part can occur. Despite being an unstable fracture, it is often initially not associated with neurological deficit because the fractured arches of C1 “burst” away from the cord. Nonetheless, patients remain at grave risk for neurologic compromise if not promptly diagnosed and appropriately stabilized and treated. With enough force, the transverse ligament may also be disrupted. Suspect this if the lateral masses have displaced 7mm or greater. In 1982, Trafton ranked the top 15 C-spine injuries in order of most to least unstable. While simple JF was in the bottom 50%, rupture of the transverse ligament of C1 was the #1 most unstable lesion. In addition, about 30% of JF are associated with fractures of C2, especially fractures of the odontoid process. Rarely JF are associated with fractures of the occipital condyle, which may be initially missed.
CT of the cervical spine demonstrates the number of fractures, their locations and degree of displacement. Treatment in the ED is directed toward providing ABC’s with special attention to stabilizing the C-spine. Closely monitor the patient’s neurologic and mental status while awaiting urgent neurosurgical or orthopedic consultation for definitive treatment (halo or surgery). In the case of suspected transverse ligament rupture, provide immediate traction to the head until more definite stabilization can be achieved.
Occipital condyle fractures are extremely rare, with only 58 cases reported in live patients between 1817 to 1994, most of these unilateral. They are categorized into 3 types, each generally associated with a unique mechanism. Type I occur as an impacted fracture secondary to axial loading, and are typically stable as the fragments comminute but rarely displace. Type II occur as part of a basilar skull fracture secondary to direct blow to the head, and are also usually stable because the alar ligaments remain intact. Type III result from either lateral flexion or rotation causing strain or tear of the alar ligament, and, like tear-drop fractures, should be considered unstable despite lack of displacement on CT.
Occipital condyle fractures may present with cranial nerve injuries in up to 31% of cases, with the Hypoglossal nerve most frequently involved (67%) due to it’s close proximity to the condyle. Look for slurred speech, difficulty swallowing, or tongue deviation in the absence of intracranial or intra-oral pathology. These fractures less commonly involve the jugular foramen, through which cranial nerves 9, 10, and 11 run. Unilateral paralysis of all 4 cranial nerves is called Collet-Sicard syndrome. Delayed cranial nerve palsy, up to 2 to 3 months, has also been described in the literature. While treatment for Type III fractures is usually surgical, Type I and II occipital condyle fractures may be treated conservatively with hard collar for 4-12 weeks.
click on image to enlarge

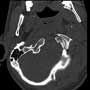
Burst fracture of C1 with fracture lines through both anterior and posterior arches with minimal displacement and prevertebral hematoma (extending from C1-C5)

Fracture of the left occipital condyle. (Right condylar fracture not seen in this image due to rotation)
What does the evidence say about spinal immobilization?
The incidence of C-spine injury (CSI) in blunt trauma is about 2-6%, and up 20% in the setting of concomitant TBI. While no formal guidelines exist on when or how to image, at this point CT is generally accepted as the test of choice for high and even low-risk patients, as the ability of plain films to pick up CSI is marginal at best: in NEXUS, plain films picked up 498/818 injuries, in Daffner et al: 108/245, in Mathen et al: 27/60, and in Bailitz et al: 18/50. The first clinical decision rule applied to CSI was the 2000 NEXUS criteria. Of the 34,069 blunt traumas and 818 CSIs, 2 (0.2%) clinically significant injuries were missed and imaging could have been deferred in 12.6%. One year later the Canadian C-spine Rule (CCR) was applied to 8,924 stable adults with 151 CSIs. Though more complex and perhaps slightly more subjective, no significant injuries were missed, and imaging was averted in 10.7%. In 2003, a head-to-head comparison of the 2 criteria – authored by the same principle investigator as the CCR and using the same cohort of patients – was published. The CCR was more sensitive than the NEXUS (99.4% v 90.7%) and more specific (45.1% v 36.8%) and resulted in lower rates of imaging (55.9% v 66.6%) (14). There is no correct answer, but one safe approach is to combine the important aspects of both rules with your clinical gestalt.
Placing and maintaining a cervical collar seems like a no-brainer, but could be we be doing harm? Despite decreasing rates of spinal cord injury seen in the ED since the 1970s (when EMS standard C-spine immobilization protocols were formalized) there is still insufficient evidence to support its use. While a true RCT could never be done in the US, one retrospective analysis reviewed blunt trauma patients who came to two similarly equipped teaching hospitals in different countries (US and Malaysia). Suprisingly, they observed that those who came without a c-collar had less composite neurologic disability (OR=2.03) than those who came in with full immobilization. Moreover, there are documented side effects to c-collar placement, including worsened dynamics of breathing, increased risk of aspiration, pressure necrosis, and increased ICP. Finally, full c-spine immobilization itself has been shown to cause midline tenderness even in healthy volunteers, resulting in further unnecessary testing.
More and more, EPs are urged to think twice about the necessity and consequences of the tests we do and treatments we give, and this is a good thing. But are you
willing to take the chance?
References:
1. LearningRadiology.com Jefferson Fracture
2. Mark R Foster, MD, PhD, FACS. C1 Fractures. emedicine.com Updated: Nov 6, 2009
3. Trafton PG. Spinal cord injuries. Surg Clin North Am. Feb 1982;62(1):61-72
4. Tuli S, Tator CH, Fehlings MG, Mackay M. Occipital condyle fracture. Neurosurgery 1997;41:368-76
5. Anderson PA, Montesano PX. Morphology and treatment of occipital condyle fracture. Spine 1988;13:731-6.
6. Falavigna A, da Silva FM, Hennemann AS. Occipital condyle fracture associated with Jefferson’s fracture and injury of lower cranial nerves: case report. Neurologia da Universidade de Caxias do Sul, Caxias do Sul, RS, Brasil. Arq. Neuropsiquiatr. 2002 Dec;60(4):1038-41. Epub 2003 Jan 15. pubmed.org
7. Demisch S, Linder A, Beck R, Zierz S. The forgotten condyle: delayed hypoglossal nerve palsy caused by fracture of the occipital condyle. Clin Neurol Neurosurg 1998;100:44-5.
8. Orbay T, Aykol S, Seckin Z, Ergun R. Late hypoglossal nerve palsy following fracture of the occipital condyle. Surg Neurol 1989;31:402-4.
9. Spinal cord Injury Information Network http://www.spinalcord.uab.edu/ Spinal Cord Injury: Facts and Figures at a Glance – June 2006.
10. Hoffman, JR et al. Validity of a set of clinical criteria to rule out injury to the cervical spine in patients with blunt trauma. National Emergency X-Radiography Utilization Study Group. 2000. NEJM 343, 94-9.
11. Daffner, RH et al. Imaging for evaluation of suspected cervical spine trauma: a 2-year analysis. Injury 2006;37, 652-8.
12. Mathen RK et al. Prospective evaluation of multislice computed tomography versus plain radiographic cervical spine clearance in trauma patients. J of Trauma 2007;62, 1427-31.
13. Mailitz JF et al. Ct should replace three-view radiographs as the initial screening test in patients at high, moderate, and low-risk for blunt cervical spine injury: a prospective comparison. J of Trauma 2009;66, 1605-9.
14. Steill IG, et al. The Canadian C-spin Rule versus the NEXUS Low-Risk Criteria in Patients with Trauma. NEJM 2003;349:2510-8.
15. Hauswald, M, et al. Out-of-hospital Spinal Immobilization: It’s Effect on Neurologic Injury. Acad Emerg Med 1998;5(3):214-9.
16. Bauer et al. Effect of spinal immobilization devices on pulmonary function in the healthy, non-smoking man. Ann Emerg Med, 1998;17(9):915-918.
17. Chan D, et al. The effect of spinal immobilization on healthy volunteers. Ann Emerg Med, 1994;23(1):48-51.
18. Ho AM, et al. Rigid Cervical Collar and Intracranial Pressure of Patients with Severe Head Injury. J of T-I I&CC 2002;53(6):1185-8
19. March JA, et al. Changes in Physical Examination Caused by Use of Spinal Immobilization. Prehospital Emergency Care, 2006:6(4):421-4.