Have you ever asked a patient a question only to have them mumble into the blanket or to the wall so softly that you couldn’t understand a word they said? Or worse, I’ve had patients, for whatever reason – anger at the wait, a show of control – refuse to answer my questions or say anything at all. “I don’t care if you only have a few minutes with me,” they seem to say. “Don’t bother me, I’m napping.”
My knee jerk response used to be to act out of annoyance and say something rude about how they are wasting my time – or worse, poke them. But after Greg Henry enlightened me about the kinder, gentler way to practice medicine I now take a slightly different approach. I ask my question a little louder and slower. And then I wait for a full minute. The silence and meditation is refreshing. And it gives the family member in the room time to prod or chastise the patient into responding. If they still refuse to say anything intelligible, I warn the patient that if they do not want to cooperate with me I cannot help them. Then I turn to leave and announce to everyone in the room that the nurse will be returning to discharge the patient.
Obviously they had a problem or they wouldn’t have agreed to come to the ED. So why did they come that far and fail to take the steps to really address their problem? Answer that question and you’ll also be able to tell me why so many emergency physicians are members of ACEP, come to the Scientific Assemblies year after year, and yet never really get involved in the real purpose of the College – to hear and represent our interests. Sure, it’s a great opportunity to hear some amazing lecturers. But Greg is right (read his unauthorized guide to ACEP on page 46), you can get your CME online. The real purpose of getting 20% of our entire corps of practitioners in one place at one time is to deal with the business of emergency medicine. It’s the business – and yes, the politics – of emergency medicine that effects us all. It effects our families, our communities, and patients as well. And it is the kind of business that is best conducted in person, with passion and purpose. Greg has written this month, as in months past, to try to wistfully entice the reader to get involved at ACEP. To show you the possibilities for learning and the joy of participation. Well on this score, I’m going to be the yin to Greg’s yang. I too want everyone to get involved in ACEP this year, but I want to light a fire under your ass. We are at a pivotal moment in medical history; it’s time to wake up and start to grapple with some of the problems head on.
It’s no secret. The cost of the business of medicine is breaking the bank. As the bill for medical care approaches 20% of our GDP, it is becoming a national security threat. And you and I, my friends, are the poster children for this ominous monster. We no longer have the luxury of standing on the sidelines and passively waiting for the next thing coming down the pike. Believe me when I say that it’s a freight train and we are standing on the tracks. Don’t believe me, here are just a few small examples of the giants starting to stir. Walmart has announced plans to open primary care clinics in many of their locations, accepting Medicare, Medicaid, and the co-pay of most insurance plans as their entire reimbursement for visits. And this isn’t competition with the usual ‘doc in the box’ seeing cold and flu urgent care cases. These clinics will be staffed by family doctors with potentially huge staffs of PAs and nurses. Walmart has 1.4 million employees before they even begin seeing other patients.
The drug store giant Walgreens has teamed up with Theranos, a nanotechnology mega-startup, to offer walk-in blood testing on a finger stick for a whole array of tests at a fraction of the cost and hassle of going to a commercial lab. Don’t think that’s a big deal? Theranos/Walgreens charges $5.30 for a CBC. How much does your lab charge? And the patient doesn’t need a doctor’s order to get any of the tests.
Research is under way to develop computer programs that can read most diagnostic X-rays. How many patients do you see who just want an X-ray to see if their ankle or finger or whatever is broken? Telemedicine is testing the limits of how fast legislatures can respond. My night time CTs are already read by a doctor in Australia. How long will it be before a doctor in Singapore is talking to patients and ordering tests in the US? Never, you say? Just stand there on the tracks and see what happens.
A few months ago EPM publicized a controversy about the College’s attempt at controlling access to ACEP council candidates (See ACEP Puts a Gag on Council Candidates). This wasn’t just a little spat about writing a good story for this magazine. This was about the College’s misguided efforts, in my humble opinion, to tamp down debate, control discussion, and prevent the exposure of controversial positions (or lack thereof) of potential leaders of the College. We should be about encouraging, not suppressing, vigorous, open debate on some of the most important issues of our time. I know that today’s medical students and residents are not exactly the college rabble rousers of the 1960s. But they should be storming the gates and demanding to know where the leadership of their specialty is taking them. What are their ideas? What do they want the specialty of emergency medicine to look like in 20 years?
If an EP could practice telemedicine from home – say a young mom or dad with children – would they take that opportunity and diminish their availability to do shifts at the ED? How could this effect the work force? How should the college be preparing for these potential shifts? Maybe the Telemedicine Section of ACEP is more important than we realized.
One of the unforeseen consequences of the Affordable Care Act was to force insurance policies to drastically increase their deductibles and co-pays in order to prevent drastic increases in premiums. In the past the patient was responsible for maybe $100 or $200 of the ED bill. But now, they might have a $5,000 deductible that they have to meet before the insurance pays anything. The effect is that even insured patients are now taking a much closer and more vocal look at these thousand dollar ED bills that we’ve been so blithely sending out. Maybe attendance at the Legislative Section of ACEP would be a good idea as well.
Non-physician health care providers with PhDs in physical therapy, nursing, pharmacy, and physician assistance are asking why they cannot be referred to as “doctor”, since that is their educational degree. Is that a good thing for patients? Is that a good thing for our profession? Maybe it would be a good idea to get involved in the ACEP committee or section that deals with these questions.
Surely you can see where I’m going with this. We can no longer apathetically turn our faces to the wall and take a nap. We have an emergency here! And we need to do something. Do I need to list the potential problems and/or opportunities for you? The editorial staff of EPM will be at booth 926 and we’d love to have you stop by. Tell us what problems and opportunities you see. But more importantly, come by and tell us what you are doing to change our specialty. Now there is something worth writing about.
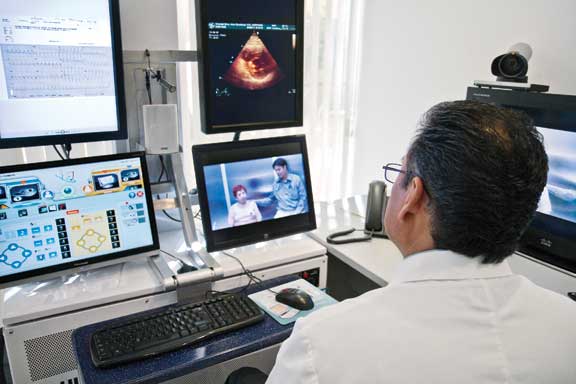
In Photo: Dr. Juan Manuel Romero engages in a pre-op consultation with his patient and her doctor, who are 400 miles away.

1 Comment
I think ACEP 14 will be awash with EBOLA (metaphorically speaking) this year, but as you point out, there are other disasters approaching that should not be ignored.
One which you mention that I think REALLY needs to be addressed emergently. And that is the lack of transparency in pricing for EP services. As the New York Times and other high visibility media have revealed, even a very prudent patient/consumer who goes to an in-network hospital for emergency care (even if this means not using EMS) can without notification be cared for by a non-participating provider and be responsible for uninsured rates, which can be substantial. This is attracting the attention of legislators, and it is going to mean that there will be more reactive legislation (possibly along the lines of EMTALA) that we need to be prepared to deal with.
Let’s hope work has already started on this coming tsunami. Sorry I won’t be at ACEP.