What’s the next step in treatment for this patient’s emergent pain?
A 53-year-old male photographer presents to the emergency department via ambulance complaining of headache, nausea and vomiting. His symptoms started after he was developing photographs and abruptly left the darkroom to use the telephone.
He states that his pain is concentrated in the right eye and radiates back into his head. He is having difficulty seeing anything other than lights from the left eye and cannot complete a visual acuity exam. His intraocular pressure is 22 mmHg in the left eye and 54 mmHg in the right eye. Which of the following treatments is most immediately indicated for his condition?
- Hypertonic saline
- Lateral canthotomy
- Morgan lens washout
- Tetracaine drops
- Timolol drops
Correct answer: E. Timolol drops
This patient is suffering from acute angle closure glaucoma and requires emergent treatment with beta blocker drops such as timolol, which will help to reduce the production of aqueous humor and concurrently lower the intraocular pressure.
Prostaglandin drops (e.g., latanoprost), acetazolamide (IV or oral) and a topical beta blocker (e.g. timolol) are often given in combination to reduce aqueous humor production. To increase outflow of aqueous humor, patients can also be given a topical alpha2-agonist (e.g. phenylephrine), topical miotic (e.g., pilocarpine) and topical steroid (e.g., prednisolone acetate). There are case reports of paradoxical angle closure with pilocarpine in specific patient populations, so it should be used with caution and in consultation with an ophthalmologist.
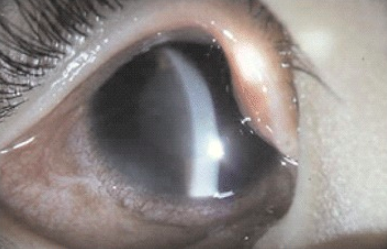
A patient’s eye may appear as in the image below, which shows a dilated, unreactive pupil with a cloudy cornea. The condition is often precipitated by rapid contraction of the iris when moving from a dark room into a light room. This blocks the outflow of aqueous humor and leads to severely increased intraocular pressure. Definitive treatment involves emergent ophthalmology consultation and peripheral iridotomy.
Incorrect answer choices:
Hypertonic saline (Choice A) is not the best choice since it does not directly lower intraocular pressure. If a patient is unable to obtain relief with topical medications such as beta-blockers, prostaglandins, miotics or steroids, then systemic osmotic agents such as hypertonic saline or mannitol can be used. These agents lower intraocular pressure by lowering the oncotic pressure that will help dehydrate the vitreous.
A lateral canthotomy (Choice B) is an emergency procedure to release pressure on the eye from a retrobulbar hematoma, which can also increase the IOP, but by a very different mechanism. The IOP is increased in this vignette because the aqueous humor is not exiting the globe and is causing a primary rise in IOP. In contrast, the IOP rises in the setting of a retrobulbar hematoma secondary to the hematoma pushing against the globe.
Thus, a lateral canthotomy will not solve the problem of acute angle closure glaucoma (just as timolol drops will not help a retrobulbar hematoma). Ophthalmology enthusiasts may point out that acute angle closure glaucoma can occur in the setting of a retrobulbar hematoma because of the resulting edema in the ciliary body. This is true, however the problem is still secondary to the retrobulbar hematoma, so drops will make little if any impact on the angle closure. Beta blocker and other drops for acute angle closure glaucoma are not considered part of the care for a retrobulbar hematoma.
Morgan lens washout (Choice C) has no role in the treatment of acute angle closure glaucoma, but can be useful for patients who sustain a chemical injury to the eye. Several liters of normal saline should be used on each affected eye, and the pH should be checked at least 30 minutes after stopping the fluids to obtain an accurate measurement.
Tetracaine drops (Choice D) can be used as a topical anesthetic for patients who require ocular diagnostics, such as a Morgan lens treatment, fluorescein staining or intraocular pressure testing. These medications have no role in the reduction of intraocular pressure or management of acute angle glaucoma. In fact they probably would have already been used to determine the IOP given in the prompt, although that is not stated and cannot be taken as truth. Remember to avoid topical anesthetics if there is concern for globe rupture.

1 Comment
Question re: IOP
When moving from the photographic developing room, which is dark (eyes in mydriasis) to go outside to answer a call, which has more ambient light (eyes snap to miosis), why would that trigger an attack of angle-closure glaucoma? After all, pilocarpine causes miosis, one of the treatment goals to free the path towards the Schlemm canal.
Thank You
Dr R Schneer,
6/13/2020