Tackling a case of cholestatic hepatitis.
A 23-year-old male presented to the emergency department (ED) with the chief complaint of nausea, abdominal pain and dark urine. The patient noted one-week of congestion, sore throat, body aches and subjective fever, followed by onset of abdominal pain.
Abdominal pain was described as achy in nature localized to the bilateral upper quadrants. Other associated symptoms included nausea, decreased appetite and yellow skin. He denied a history of alcohol use, tobacco use, gastrointestinal malignancy in himself or his family, or any other pathology.
Findings
Vitals on arrival to the ED: 97.9 °F, blood pressure of 115/98 mmHg, respiratory rate of 20 breaths/min., 67.1 kg, and 97% pulse ox on room air. On physical exam the patient appeared well-developed, well-nourished and in mild distress secondary to his abdominal pain. His oral mucosa was dry. His eyes exhibited scleral icterus bilaterally and he was diffusely jaundiced. He exhibited posterior cervical lymphadenopathy and axillary lymphadenopathy. His cardiopulmonary exam was unremarkable. Abdominal exam revealed tenderness to palpation within the bilateral upper quadrants without peritoneal signs. No other acute findings were found on physical exam.
A complete blood count revealed no leukocytosis, however, lymphocyte predominant at 5.5 (1.1-4.0 bil/L). Basic metabolic panel showed a mild hyponatremia of 133 (135-145 mmol/L). Hepatic function panel showed an alkaline phosphatase (ALP) of 462 (30-110 U/L), aspartate aminotransferase (AST) of 230 (10-37 U/L), alanine aminotransferase (ALT) of 276 (9-47 U/L), total bilirubin of 8.9 (0.3-1.2 mg/dL), direct bilirubin of 5.8 (0.0-0.3 mg/dL), gamma glutamyl transpeptidase (GGTP) of 215 (13-60 U/L). Ultrasound of the right upper quadrant revealed a homogenous normal echotexture, no intrahepatic or extrahepatic biliary dilatation.
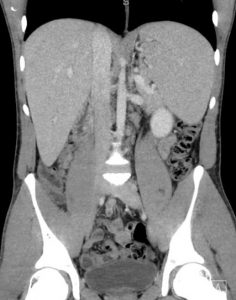
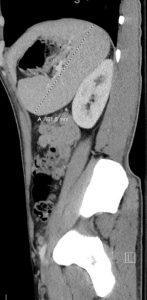
The common bile duct was slightly enlarged measuring 5.2 mm, and an unremarkable gallbladder. CT of the abdomen/pelvis with intravenous contrast, exhibited splenomegaly with an enlarged spleen measuring up to 16.2 cm in longitudinal direction. No other acute intra-abdominal or pelvic process was identified. An acute hepatitis panel was negative.
A mononuclear spot test was positive. A subsequent EBV IgM was positive at >160 (0-35.9 U/mL). The patient was admitted for clinical hepatitis and dehydration. He had an uncomplicated hospital course and continued to improve and was ultimately discharged on day 2. At his three-month gastroenterology follow-up, he continues to feel better, lymphadenopathy is improving and his liver enzymes while still elevated are continuing to down-trend.
Discussion
Infectious mononucleosis is most commonly caused by Epstein-Barr virus (EBV) and manifests as a febrile illness, pharyngitis and cervical/generalized lymphadenopathy. EBV makes up to 90% of all cases of mononucleosis, however, it can be caused by human herpes virus 6 (HHV-6), cytomegalovirus (CMV), and herpes simplex virus 1 (HSV-1).(1) It is mainly transmitted through saliva.
While cervical/generalized lymphadenopathy, pharyngitis, palatal petechiae, and fever are common presenting features, it is worth noting the other clinical features that occur with less frequency.
- Splenomegaly occurs in only 52% of all cases, begins during the first week of illness, and can lasts up to four weeks.(1)
- Hepatomegaly occurs in only 12% of cases.(1)
- Erythematous, papular, macular, or morbilliform type rash is seen in 10% of cases (up to one-third in pediatric patients).(1)
- Jaundice presents in about 9% of patients. Involvement of the liver in an EBV infection manifests as mild hepatitis (cholestatic hepatitis).(1)
A complete blood count will often reveal >50% lymphocyte predominant. A hepatic panel can reveal elevations in AST and ALT up to 5x normal. A mononuclear spot test, also referred to as a heterophile antibody test, is the best initial test for diagnosis, however, it does post a 25% false negative rate during the first week of the illness.(2)
Conclusion
The potential complications can be devastating, especially if not recognized. Splenic rupture, although rare and seen in about 0.5% of all cases, is a result of a massive lymphocyte infiltration, with a mortality up to 30%.(1) The average period between onset of symptoms and splenic rupture is 14 days.(1)
Given the dramatically enlarged spleen, it is vulnerable to not just spontaneous rupture, but rupture secondary to trauma, coughing, defecating, vomiting, or even turning over in bed.(1) As the images demonstrated in our patient, he had a significantly enlarged spleen. The greatest risk of rupture occurs during the first three weeks of illness.(2)
Other rare, but possible complications include: acute interstitial nephritis, Guillain-Barre syndrome, encephalitis, hemolytic anemia, meningitis, myocarditis, thrombocytopenia, upper airway obstruction, and cholestatic hepatitis.(2)
While hepatic involvement to some degree is seen in the majority of patients, clinical manifestations of cholestatic hepatitis is considered rare. Only a few cases in the literature have been reported of cholestatic hepatitis secondary to EBV infection. The mechanism is not well understood but thought to be associated with a mildly swollen bile duct.(4)
It can present with dark urine, scleral icterus, transaminitis, jaundice, and abdominal pain, to name a few. During the acute phase of the infection, a transaminitis is present in about 80% of cases, while jaundice is only present in about 6.6% of cases.(4) As clinicians in this particular setting, ultrasound and CT are often done to rule out extrahepatic causes of biliary obstruction. This potential complication and the potential complications listed above should be considered in any patient presenting to the ED with a history of a pharyngitis, fever, and lymphadenopathy.
References:
- BMJ Best Practice. “Infectious mononucleosis.” October 9, 2018. https://bestpractice.bmj.com/topics/en-us/123
- Womack, J, Jimenez, M. “Common questions about infectious mononucleosis.” American Family Physician. 2015 Mar 15;91(6):372-376. https://www.aafp.org/afp/2015/0315/p372.html
- Dogan, I, Ergun, M, Cindoruk, M, Unal, S. “Acute hepatitis induced by Epstein-Barr virus infection: A case report.” Turkish Journal of Gastroenterology. 2007; 18(2): 119-121. http://europepmc.org/abstract/med/17602362
- Kang, M, Kim, T, Shim, K, Jung, S, Cho, M, Yoo, K, Chung, K. “Infectious mononucleosis hepatitis in young adults: Two case reports.” Korean Journal of Internal Medicine. 2009 Dec; 24(4): 381-387. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2784984/www