How can the tap look this bad when the patient looks this good?
Fever in the newborn is easy in one respect. You don’t have to think, just do. If the baby has a fever in the first four weeks of life, emergency physicians will obtain cultures, start antibiotics and admit. The lumbar puncture is a standard part of the “sepsis work-up” for neonates. Of course you perform one – you are on auto-pilot.
Between five weeks and two months, things get trickier. The infant’s ability to respond to infection has improved and their clinical condition is somewhat easier to assess. Although they have not yet received immunization against Haemophilus influenza type B and Streptococcus pneumoniae, they benefit from reduced exposure as the vast majority of the children around them have been vaccinated.
And thus we find a certain pediatrician on a recent chilly morning, facing a febrile seven-week-old. The baby was a term infant. There were no particular problems noted with pregnancy or delivery. A prenatal ultrasound had identified a multicystic kidney on the right. At five weeks of age the infant underwent a total nephrectomy on the right with placement of an epidural catheter by Anesthesia before the procedure. The procedure went well and the baby was sent home. But the parents now feel that the baby has been more fussy ever since.
 Yesterday she developed a fever. Confronted with this story, the pediatrician examined her. She was febrile to 102 but appeared vigorous and nontoxic. The pediatrician ordered a white count, urine and cultures and sent the baby home from the office with close parental observation and planned follow-up. The white count was 22,000.
Yesterday she developed a fever. Confronted with this story, the pediatrician examined her. She was febrile to 102 but appeared vigorous and nontoxic. The pediatrician ordered a white count, urine and cultures and sent the baby home from the office with close parental observation and planned follow-up. The white count was 22,000.
The next day the baby was brought back for the follow-up appointment. Still febrile, still fussy. A repeat white count was now 31,000. Clearly more of a work-up was required and she was sent to the ED.
In the ED, the infant is febrile but vigorous and nontoxic. You don’t see any focus of infection that is obvious on your exam. You decide to do a full sepsis work-up because of the persistent fever, fussiness and rising white count. An LP seems like a good idea, given that the signs and symptoms of meningitis in seven-week-olds are very nonspecific. You perform the tap and get a scant amount of what looks like pure pus. That’s not good. You call for the nurse to drop everything he’s doing and hang vancomycin and ceftriaxone.
It’s funny – the infant continues to look well. How can the tap look this bad and the patient look this good? Is there something else going on?
Some time goes by. The mother points out to the resident that there is some swelling on the infant’s back. It is higher than the LP site. The act of tapping the baby shouldn’t have produced swelling there. You wonder, did you even hit the CSF space or did your needle enter an abscess?
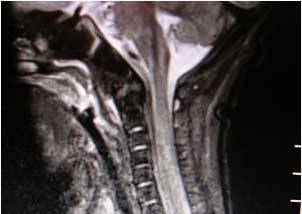
You order an ultrasound but there is no drainable fluid collection in the soft tissues of the back, just some edema. The Radiologist recommends an MRI of the spine and there it is, a large semi-loculated epidural abscess, located posteriorly and running from T11 to the coccyx. You consult Neurosurgery and the infant is taken to the OR to evacuate the abscess.
So why does this seven-week old infant have an epidural abscess? What organisms do you need to worry about? What is the prognosis?
Spinal epidural abscesses are rare in children. Bacteria can set up shop in the epidural space by hematogenous seeding, direct extension from a nearby infection or by inoculation into the spinal canal during procedures. This baby most likely got the abscess due to the epidural catheter placed for the prior surgery. The most likely organism causing this is Staphylococcus aureas, although the list of possible culprits also includes gram-negatives, coagulase-negative staphylococci, streptococci and anaerobes. The abscess can cause spinal cord compression, leading to progressive weakness and eventually paralysis. The classic triad includes back pain, fever and neurologic deficits but the majority of patients do not present with this triad and the diagnosis is often delayed. The best treatment for these abscesses is drainage plus antibiotics. Once paralysis occurs, it can be irreversible.
This baby eventually grows MRSA from the abscess site. There is no obvious neurologic deficit identified, so hopefully the abscess was evacuated in time. Her prognosis should be good.
Lots of patients come to the ED with back pain. How would you know to worry about an epidural abscess? First, it has to be on your differential. If you don’t think about it, you won’t pick it up. The classic triad is helpful, but as mentioned above, frequently incomplete. Fever is the sign most commonly absent. Patients with back pain should be assessed for risk factors associated with abscess: diabetes, IV drug abuse, chronic liver or kidney disease, history of spinal procedures or spinal fractures, indwelling lines, immunocompromise and any recent bacterial infections (cellulitis, UTIs, others). With regard to physical exam, it is always a good idea to actively note the temperature of a back pain patient (circle it on the chart, or notate the EMR, to acknowledge you have noted what the patient’s temperature is). Also, watch for thoracic back pain in patients who are verbal. Most pain in the back is in the areas that are most mobile – the cervical and lumbar spine. It is unusual to have pain in the thoracic area (a common site for epidural abscesses). Another clue to the diagnosis – pain on direct pressure on the spinous process – an unusual finding in routine musculoskeletal pain.
Most of these won’t have an abscess but at least do a careful neuro exam and provide follow-up. The lab can be helpful. White counts are frequently normal but ESRs are frequently elevated in epidural abscess and vertebral osteomyelitis. If you are concerned about an abscess, MRI is the preferred test although CT with contrast can also be utilized.
Don’t worry; trust your judgement. The next well-appearing seven-week old you see with a fever may just have a viral infection. Do a good history and examination, think about getting some screening labs, and ensure good follow-up.
Amy Levine, MD, is an associate professor of pediatric emergency medicine at UNC Chapel Hill.

2 Comments
Thank you for another super interesting and very informative case. As a first-year medical student I like to come here when I need a break from studying– this gives me something that is both interesting and educational.
You’re so awesome! I do not believe I’ve truly read anything like that before.
So good to discover another person with a few unique thoughts on this subject matter.
Really.. thanks for starting this up. This web site is one thing that’s needed
on the internet, someone with a bit of originality!
Check out my site :: cialis online pharmacy: http://edhealthnyc.com/