 A simple modification in practice can protect your patients from hypoxia during emergency intubation. Imagine intubating all of your patients without the high anxiety and low tones (boop, boop, boop…) of a falling pulse oximeter reading. During pre-oxygenation, applying nasal oxygen in addition to a non-re-breather face mask can significantly boost the effective inspired oxygen.
A simple modification in practice can protect your patients from hypoxia during emergency intubation. Imagine intubating all of your patients without the high anxiety and low tones (boop, boop, boop…) of a falling pulse oximeter reading. During pre-oxygenation, applying nasal oxygen in addition to a non-re-breather face mask can significantly boost the effective inspired oxygen.
Nasal Oxygen During Efforts Securing A Tube
A simple modification in practice can protect your patients from hypoxia during emergency intubation. Imagine intubating all of your patients without the high anxiety and low tones (boop, boop, boop…) of a falling pulse oximeter reading. During pre-oxygenation, applying nasal oxygen in addition to a non-re-breather face mask can significantly boost the effective inspired oxygen. After apnea created by RSI the same high flow nasal cannula will help maintain, or even increase, oxygen saturation during efforts securing the tube (oral intubation). The use of nasal oxygen during pre-oxygenation and continued during apnea can prevent hypoxia before and during intubation, even in extreme clinical cases.

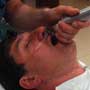
Oral intuabtion with nasal cannula running high flow oxygen
Case 1: An alcoholic, obtunded patient has a pulse ox of 70% and sonorous respirations. A nasal trumpet fails to improve saturation though airway obstruction is reduced. Applying a non-re-breather mask at 15 lpm only brings the pulse ox up to 74%. Combining nasal cannula at 15 lpm with the mask at 15 lpm raises the pulse ox to 90%. After RSI, the patient is gently bagged up to a pulse ox of 94%. Video laryngoscopy and intubation is quite difficult due to secretions and excessive tissue. Despite prolonged intubation efforts, four attempts between two operators, the pulse ox rises during apnea to 98%. The lab calls shortly after intubation; the patient has a blood alcohol level of 560.
———-
Case 2: A super-obese (680 lb.) man with a history of significant sleep apnea presents to the ED with decreased mental status and marked hypoxia. Initial pulse ox was 68%, the patient had an ashen color, and a heart rate of 150. The application of assisted bag-valve mask, bilateral nasal trumpets, and ramping ear-to-sternal notch – elevating head and shoulders until the ear and sternal notch are horizontally aligned – brought the pulse ox to 85%. Addition of high-flow nasal cannula (>15 lpm) along with bag-valve ventilation improved the pulse oximetry to 95%. The patient was orally intubated using Etomidate only, and throughout the entire process, with nasal oxygen continuously flowing, the oxygen saturation remained at 95%.
———-
Case 3: An 89-year-old emaciated woman is transferred to a trauma center for a chronic subdural hematoma. On arrival, after being transferred laying flat on a spine board with a cervical collar, she arrives tachycardic to 130, tachypneic breathing at 45 breaths per minute, and a pulse ox of 77%. Despite high flow oxygen, and upright positioning her pulse oximetry cannot be increased above the low 80’s. There is marked retractions of the ribs and clavicles and notable increased work of breathing. The patient is edentulous with poor respiratory excursion and the mask fits poorly. A blood gas is drawn and the patient’s family is informed of possible need for intubation. The ABG comes back 7.45/40/42, Bicarb 27, BE 2.7, O2 saturation 80%. She has never smoked and has no diagnosis of chronic lung disease. While preparing for possible intubation, high flow nasal cannula is added to 15 lpm mask flow, and the pulse oximetry climbs as high as 98%. Ultimately, the family and patient decide not to proceed with intubation and the patient is managed with non-invasive ventilation.

Pre-oxygenation combining high flow nasal cannula and a non-rebreather mask
While the common perception is that a non-rebreather mask is the pinnacle of oxygen adminstration, effective FiO2 from these masks may not create optimal pre-oxygenation at flow rates of 15 lpm. This is because the measured inspired oxygen in the hyopharynx with a non-rebreather at 15 lpm is only 60-70%. The reason for this is the patients expired gasses are mixing with the applied oxygen, and also because expired gasses accumulate in the nasopharynx. Quiet breathing involves flow rates as high as 30 lpm; maximal pre-oxygenation with a loose-fitting non-rebreather may require a flow rate as high as 48 lpm. High flow nasal oxygen has been shown to flush the nasopharynx with oxygen, and then when patients inspire they inhale a higher percentage of inspired oxygen. Small changes in FiO2 create dramatic changes in the availability of oxygen at the alveolus, and these increases result in marked expansion of the oxygen reservoir in the lungs prior to the induction of apnea.
After the induction of apnea, nasal cannula diffuses oxygen down the trachea to the alveolus. It is absorbed across the alveolar capillary membrane, despite the absence of respiratory movements, even as laryngoscopy is being performed. This occurs because of the difference in gas production and uptake in the alveolus, and the differences in the solubility of oxygen and carbon dioxide in the blood. Carbon dioxide excretion into the alveolus diminishes during apnea because carbon dioxide is approximately 25 times more soluble than oxygen in blood. It is estimated that during apnea CO2 is excreted into the alveolus at only 10 ml/min. Conversely, oxygen is absorbed at 250 ml/min. The resultant negative pressure gradient (-240 ml/min) creates a sub-atmospheric pressure in the alveolus. The net result is that during apnea, oxygen insufflated into the upper airway will be “drawn” down the trachea and into the alveolus. Oxygenation can be maintained in non-breathing humans for 100 minutes through apneic diffusion, even as carbon dioxide builds up in the blood.
Nasal oxygen as an adjunct for intubation has been described in a few elective anesthesia studies. In 1988 Teller demonstrated that 3 lpm nasal oxygen (through a catheter placed inside a trumpet) could maintain oxygenation at 98-99% for 10 minutes without ventilation. Without this nasal oxygen, the same patients after pre-oxygenation had an average time of safe apnea time (above 92%) of only 6.6 minutes. In 2006 Taha used 5 lpm via a nasal catheter and demonstrated pulse oximetry readings above 95% in 15 patients after 6 minutes of apnea; without the nasal oxygen the safe apnea time was only 3.65 minutes. Studying morbidly obese patients, Ramachandran used 5 lpm nasal cannula to extend the safe apnea time from 3.49 minutes to 5.29 minutes. He also demonstrated that patients with nasal cannula applied could be re-oxygenated (from 95% to 100%) in half the time (0.69 minutes vs. 1.57 minutes).
Nasal oxygen doesn’t affect the choice of oral intubation technique (direct or video laryngoscopy). The short time use of non-humidified oxygen has minimal risk of bleeding or irritation. Decreasing respiratory drive in patients with chronic hypercarbia is irrelevant after the decision to intubate. There is no risk of barotrauma, even at combined face and nasal oxygen flow rates exceeding 30 lpm. Air can leak out of a face-mask through the exhalation ports (rubber flaps) or from the pressure release valves built into a bag-mask resuscitator. The only challenge to the routine use of nasal oxygen is the availability of a second oxygen source.
NO DESAT! Once you’ve managed airways with
out the anxiety associated with critical hypoxia and a nurse narrating the declining pulse ox, you may just get used to a little less drama.
Dr. Levitan is an Associate Prof. of EM at Jefferson Medical College and has an adjunct appointment at the Univ. of Maryland; he has been researching and imaging intubation for twenty years. Dr. Levitan helps run a monthly airway management course involving specially prepared cadavers: jeffline.jefferson.edu/jeffcme/Airway

5 Comments
How do I find references for the article No DESAT
Thanks for great article. I hope it will be useful for me and my pts.
Great article. Can you provide the reference for this sentence- There is no risk of barotrauma, even at combined face and nasal oxygen flow rates exceeding 30 lpm.
Wasn’t your original NODESAT “Nasal Oxygen Delivery to Extend Safe Apneic Time”?
In the pre-oxygenation phase, is it acceptable to use only a 15L NC? In our ER we have only two outlets and one is hooked to the vent, leaving us with one outlet for the BVM. It would be a challenge to operate an NC, a bag, and an NRB. I could consider the use of an outlet splitter but just wondered if the same effects would be achieved without NRB?