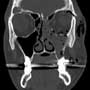
A fifty year-old male with no past medical history presented to the ED complaining of sore throat, difficulty swallowing and feeling “bubbles” on the side of his neck for one day.
Two days earlier he had been assaulted with a single closed-fist punch to the left periorbital region. He had experienced loss of consciousness followed by headache, facial pain and swelling, left periorbital ecchymosis, and transient blurry vision in his left eye. The patient had been initially evaluated and treated at Nassau University Medical Center, where a CT head and C-spine were found to be normal, but the maxillofacial CT showed the following significant findings: Comminuted and depressed fractures of the anterior and lateral walls of the left maxillary sinus, with extension to the frontal process, comminuted fracture of the medial wall of the left maxillary sinus, fractures of the left lateral, medial, and inferior orbital walls, without evidence of entrapment of the inferior rectus muscle on the left; left intraorbital emphysema; segmental fracture of the left nasal bone, as well as a segmental fracture of the left zygomatic arch. A significant amount of subcutaneous emphysema was noted in the left temporal fossa, left malar, and left periorbital regions, and blood was noted in the left maxillary sinus.
Oral-maxillofacial surgery had been consulted and he was scheduled for surgery the following week, and discharged.
Upon presenting again to the ED, the patient was found to have a large left periorbital hematoma, and moderate facial swelling on physical exam. The left eye exam showed a conjunctival hemorrhage, but was otherwise normal. Subcutaneous emphysema was present on both sides of the patient’s neck, more prominent on the left, and extended to the superior anterior chest wall. Breath sounds were equal bilaterally, and the rest of the exam was noncontributory. A soft tissue CT of the neck and chest were ordered and showed extensive subcutaneous emphysema originating from the left facial region with dissection into the retropharyngeal, paravertebral, and posterior cervical spaces with resultant pneumomediastinum and a small amount of pneumopericardium. The patient was subsequently admitted to the trauma service for observation and IV antibiotics, and subsequent surgery to repair facial fractures.
CT #1 was done on the day of the injury. CT coronal reconstruction shows fractures of left orbit, maxillary sinus, subcutaneous and intraorbital air
DISCUSSION
Pneumomediastinum after traumatic thoracic injury is not uncommon, and is often as- sociated with injury to the trachea, bronchus, esophagus, or hollow gastrointestinal viscus, or can occur after a pneumothorax tracks along the hilum into the mediastinum.

Less frequently, pneumomediastinum can occur after isolated facial injury, and has been reported in several different case reports. One article that we reviewed describes 19 cases of pneumomediastinum resulting from isolated facial trauma (1). All 19 cases were treated conservatively with IV antibiotics, and resolution of the symptoms and radiological findings were reported within a few days.
Communication between naso- and oropharyngeal fascias with cervical and mediastinal fascial planes is well documented. Descending necrotising mediastinitis, a complication of Ludwig’s angina, and retropharyngeal and peritonsillar abscess, are well documented in literature. (6, 7).
There are 3 major routes that air and pus can travel (7). The first is the pretrachal space between the trachea and strap muscles and pretracheal fascia. It communicates with the anterior mediastinum. In addition, the peritracheal fascia is fused at the level of carina with the pericardium and parietal pleura. The second is the carotid sheet, which encloses the carotid, internal jugular vein, and vagus nerve. The third is the retrovisceral or retropharyngeal space which extends to the posterior mediastinum and diaphragm. This is the most common route.
Gravity and breathing that changes intrathoracic pressure are contributing factors, and maneuvers such as the valsalva or nose blowing may cause a potential valve phenomenon.

In conclusion, pneumomediastinum is a rare but recognized complication of blunt facial trauma. Patients can present with symptoms in addition to those attributable to their facial injuries such as pleuritic chest pain, dysphagia, and reported crepitus.
In the absence of other injuries and following correct management of the facial injury, patients should be treated with rest and intravenous antibiotics, and instructed with sinus precautions. While spontaneous resolution is the course most often, possible complications include infection and airway compromise, and in the cases reported in the literature, patients were administered IV antibiotics and observed prior to surgical facial repair. Further diagnostic imaging does not appear to be warranted.
Our patient was admitted for IV antibiotics, and an esophagram as requested by the inpatient surgical service was negative. Later he underwent oromaxillofacial surgical repair and was subsequently discharged.
images 2 and 3, taken two days after the injury, show pneumopericardium and pneumomedistinum.
References
1. Monksfield P, Whiteside O, Jaffe S, Stevenson N, Milford Ch. Pneumomediastinum, an unusual complication of facial trauma. Ear, Nose and Throat Journal, May 2005
2. Abrahamian FM, Pollack CV.Traumatic pneumomediastinum caused by isolated blunt facial trauma: a case report. The Journal of Emergency Medicine Volume 19, Issue 1, pages 43-46 (July 2000)
3. Griffey RT, Ledbetter S. Pneumomediastinum and Subcutaneous Emphysema after Isolated Blunt Facial Trauma. Journal of Trauma, November 2008 66(5):1201
4. Gwenael R, Benoit V, Joel F. Massive Pneumomdiastinum and Subutaneous Emphysema Secondary to Isolated Zygomaticomaxillary Complex Fracture. Journal of Craniofacial Surgery, January 2010, (1)’;266-8
5. Roccia D, Griffa A, Nasi A, Baragiotta N. Severe Subcutaneous Emphysema and Pneumomediastinum associated with Minor Maxillofacial Trauma. Journal of Craniofacial Surgery November 2003. 14(6):880-3