Just when your evening can’t get any worse, two of your stellar EM residents come up to you and inform you that the internal medicine team is trying to “block” yet another admission. This is the 5th attempt at refusal today. The patient in question is acidotic, thrombocytopenic, altered, and bleeding from around the PICC line that was placed while he was in the hospital last week. He was recently discharged after a brief hospital admission for urosepsis, and is supposed to be receiving parenteral antibiotics and intravenous fluids through this precarious line. His wife brought him in because she was worried he looked worse, and she was concerned that the home health nurse couldn’t get his antibiotics infused through the malfunctioning PICC. After you listen to the internal medicine resident’s reasoning for refusing admission, “We just discharged him…he doesn’t look that bad to me…he can follow up as an outpatient…and the hospital is full…” you kindly show him how every blood test performed from the ED is abnormal and many of them have a “critical value” notation next to the result. In addition, the patient hasn’t been able to receive any of his IV therapy at home because the PICC isn’t working. There’s no way to argue with your logic or with the numbers in front of him, so he finally concedes to do the right thing for the patient. You marvel at just how far the paradigm has shifted. When did it become so in vogue to become an obstructionist?
 You are thankful that the next three patients presented to you seem relatively straightforward. All three patients have a chief complaint of chest pain. All three of them have enough risk factors that they deserve an evaluation for ACS in your department tonight. And with your ED’s chest pain protocol, you don’t have to use your powers of persuasion to get a consultant to care for the patients. You finish examining the first two patients, and agree with your residents that they have stories concerning for potential cardiac ischemia. When you get to the third patient, you realize he isn’t as straightforward as anticipated.
You are thankful that the next three patients presented to you seem relatively straightforward. All three patients have a chief complaint of chest pain. All three of them have enough risk factors that they deserve an evaluation for ACS in your department tonight. And with your ED’s chest pain protocol, you don’t have to use your powers of persuasion to get a consultant to care for the patients. You finish examining the first two patients, and agree with your residents that they have stories concerning for potential cardiac ischemia. When you get to the third patient, you realize he isn’t as straightforward as anticipated.
The third patient is a 65 year-old fit and muscular male, sitting upright in the stretcher. Yes, he has left sided and substernal chest pain radiating to his left shoulder. He does note that it is exacerbated by working out, and yes, he does have a history of hypertension and hypercholesterolemia. The only thing that doesn’t make sense is how he is holding his arm across his body. Instead of the typical Levine’s sign, the patient is holding his left arm across his upper abdomen with the elbow bent at 90° and his hand is resting near his right upper quadrant. When questioned about this, he notes that his chest hurts if he tries to extend or abduct his shoulder. You palpate along his chest wall and ask him some more detailed questions about what brought about his chest pain today. As you are talking, you perform a quick bedside ultrasound of his left chest.
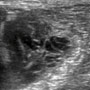
 You obtain a couple of diagnostic images from scanning his left chest wall (Figure 1 and Figure 2). What do you see? What is causing the patient’s chest pain?
You obtain a couple of diagnostic images from scanning his left chest wall (Figure 1 and Figure 2). What do you see? What is causing the patient’s chest pain?
Case conclusion in the following
 When you palpated the patient’s pectoralis muscles, they were remarkably tender. On examination, the left chest musculature appears more prominent than the right. When you delve more into the patient’s history, you discover that he has been trying to increase the amount of weight he can bench press, and has been “pushing himself” over the past two days because he has been trying to impress his new, female personal trainer.
When you palpated the patient’s pectoralis muscles, they were remarkably tender. On examination, the left chest musculature appears more prominent than the right. When you delve more into the patient’s history, you discover that he has been trying to increase the amount of weight he can bench press, and has been “pushing himself” over the past two days because he has been trying to impress his new, female personal trainer.
An ultrasound of his chest demonstrates normal muscle (Figure 1 on previous page & 3), adjacent to a torn muscle with hypoechoic edema interspersed between the injured fibers (Figure 2 on previous page & 4).
 You continue to follow the pectoralis muscle laterally towards its insertion site at the bicipital groove of the humerus. You note that a portion of the muscle is contracted and surrounded by a pool of anechoic blood. (Figure 5). This is likely where the largest muscle tear occurred and is why your patient isn’t comfortable extending, rotating, or abducting his shoulder.
You continue to follow the pectoralis muscle laterally towards its insertion site at the bicipital groove of the humerus. You note that a portion of the muscle is contracted and surrounded by a pool of anechoic blood. (Figure 5). This is likely where the largest muscle tear occurred and is why your patient isn’t comfortable extending, rotating, or abducting his shoulder.
The patient’s EKG appears normal, and you decide to cancel the rest of the blood tests and stress test that were initially ordered on him. You remind your residents about the art of medicine and the importance of a good history and physical exam. You use this case to illustrate why physicians have not been replaced by algorithmic, computer-generated treatments based on patient’s responses, and teach everyone a little bit more about how cool musculoskeletal ultrasonography can be.

As you push back the ultrasound machine into its storage area, you can’t help but laugh at the display in the consultant’s room. The end of the shift has inspired your residents to leave the internal medicine team a goalie mask, a stack of bricks, and bright orange warning cones, so that they can construct an actual physical barricade to aid in their next admission “block”.
Tips & Tricks for Musculoskeletal Ultrasound
1. Ultrasound can be used to augment clinical findings and help expedite the diagnosis in patients suspected of having a musculoskeletal injury
2. Large muscle injuries are usually easy to diagnose based on history and physical exam alone. Partial or small tears can be assessed via bedside ultrasonography.
3. Use the 7.5 to 10 MHz linear array transducer for visualization of superficial muscles. Large, deep muscles of the thigh or buttocks are best visualized using lower frequency probes.
4. The patient should be scanned in a position of comfort, allowing for full relaxation of the muscles in question.
5. The echotexture of normal skeletal muscle consists of a relatively hypoechoic background of muscle fascicles interspersed between hyperechoic strands of fibroadipose septa (Figure 1).
6.
Scan along adjacent normal tissue planes to gain a better appreciation of what the patient’s normal muscles and tendons look like. Begin the scan away from the suspected area of injury and slowly work your way towards the most painful site.
7. Look for breaks in the normal muscle fibers or areas of hypoechoic edema or hematoma formation. The myotendinous junction is the weakest point along the muscle fibers, and is therefore the most common site of partial or complete muscle injury. Scanning around this site may demonstrate obvious tears, edema, or inflammation.
8. On bedside scanning, avulsion or retraction of the muscle fibers may be noted in proximity to the tendon or aponeurosis to which they attach. Contracted muscle will appear more hyperechoic than adjacent, normal fibers.
9. Remember that the angle between the ultrasound beam and the muscle is important. If the beams are not directed exactly perpendicular to the muscle fibers on the long axis view, hypoechoic artifacts may be seen and misdiagnosed as areas of injury or edema (anisotropy).