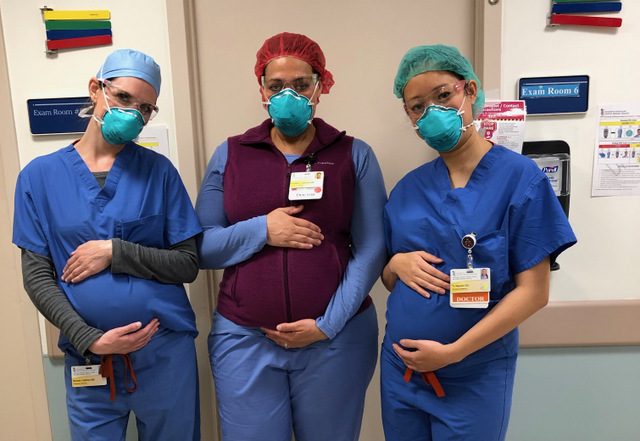
Managing emergency department shifts and the COVID crisis while preparing for motherhood.
As an emergency physician during the COVID-19 crisis, I have seen the ways in which our ideals of safety and protection have completely changed. Providing care in the historically underserved area of Prince George’s County, Maryland, the coronavirus has become an all-consuming threat dominating my work, especially considering the resounding uncertainty around how the virus will change. The hectic emergency room that I am used to is nothing compared to the chaos that has erupted now.
With tensions high and the severity of the virus ongoing, we have all had to seriously reflect on our own well-being and how this virus may impact us and our families. And as a pregnant physician, these concerns have felt even more real. Not only do I have to consider ways in which the crisis could impact my health personally, but I have to think about how this could affect my daughter to be born in June.
The constant buzz of the emergency department is not exactly conducive to being pregnant under normal circumstances. Now add the intensity of COVID-19 and it requires an introspective look on ways to practice self-care in order to maintain personal health and wellness. I am careful to be conscious of my mood, fatigue and physical needs.
Simple things such as drinking enough water on a shift are more difficult since I’m constantly wearing a mask or a respirator. I have friends and family who want me to outright stop working. But with so much need during this time of crisis, I didn’t feel like I could just sit at home if I have the ability to help people, to make this chaos even a little more bearable. I needed to take myself into account more now than before and be even more vigilant about my physical and emotional needs. After all, I will not be helpful to anyone if I become sick.
I’ve seen firsthand the ways COVID-19 is devastating to so many. Many patients are being thrown into an emergency situation and don’t know how to respond. With such uncertainties, the importance of advance care plans is more essential than ever.

Every day, I make countless phone calls to frantic family members who are scared and shocked and too often cannot answer the question, “What would your loved one want done in this emergency?” This is not just something I tell my patients. It’s something I confront myself.
COVID-19 has made me reconsider my own health care wishes. Upon realizing the magnitude of this crisis, I sat down with my husband to have a difficult conversation about what I would want for myself should I become sick and ways to best protect our baby.
During the pandemic, it is difficult to think about ourselves and our loved ones being individually impacted. However, it is important to be prepared in these situations ahead of time rather than waiting for a crisis to strike. We, as physicians, must lead by example and do for ourselves what we are asking so many of our patients and family members to do in the era of COVID-19.
We have all witnessed how quickly patients can become sick and how this virus can strike people of all ages. You can — and should — make an advance care plan outlining your healthcare wishes. I recommend going to CDC.org for more information on state-specific advance directives or an online platform, like MyDirectives.com for a convenient and easy way to keep wishes up to date and accessible to your family and medical team.
The importance of advance care planning is immeasurable should a health crisis arise particularly for us who are high risk in the emergency department and especially when we must face formidable challenges when creating protocols for scarce resources.
As a mother of an 18-month old and soon to be a mother of a newborn, the pandemic has impacted me in a unique way. The global crisis provided me — and so many mothers-to-be out there — with challenges unthinkable when we first got pregnant. Many hospitals are now preventing visitors during checkups, ultrasounds and in delivery rooms. This sense of loneliness in what should be a time of joy during pregnancy also adds to the fears that come with pregnancy.
However, it is important to remember that even if without friends and family in the delivery room, we are not alone. The medical professionals providing care to pregnant women at this time are there for support, to help combat fear, anxiety and uncertainty. In this time of crisis, pregnant women are strong and are in this together and will get through this with grace.
I made the decision to work until the risk became too great, until I could no longer wear PPE for 12 hours a day and drink enough water, use the bathroom or eat like I should. I recently went on leave after speaking to my OB/GYN and considering my previous risk of preterm labor and the new ACOG guidelines to stop clinical work at 36 weeks. This was a difficult decision. Doctors are notoriously bad patients and I feel guilty for leaving my colleagues on the front lines.
Like most emergency physicians I feel a duty to work and often put others first. My background in bioethics and health policy has provided me with an ability to think of patients in a more comprehensive context. Being an emergency physician has given me the ability to see the human in people, to be present at their lowest and most vulnerable moments and to identify with the common human experience.
The ER is often filled with people who are scared, lonely or lost. But those same people can be hopeful, courageous and optimistic. They are petrified of what is to come, but hold onto the hope that the future will be better. These people I encounter daily are what drive me to move forward. They instill hope within me, especially now during a time of fear and confusion.
Working during this crisis has reconfirmed the sense of faith I have in those in my community. Those working long hours to fight the pandemic. Those following CDC guidelines in order to prevent the spread and flatten the curve. Those making sacrifices in order to protect the vulnerable.
They remind me why I do what I do — and why I love what I do.