Which medication can cause severe inspiratory stridor followed by apnea?
You are performing procedural sedation to assist an otolaryngologist in removing a fishbone from a patient’s pharynx. Approximately one minute after the sedation medication is given; the patient develops severe inspiratory stridor followed by apnea.
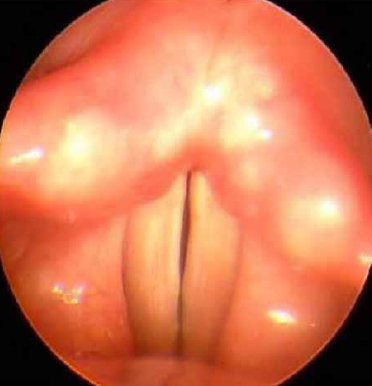
Before ENT removed the fiberoptic endoscope for airway management, the following view was obtained and is persistent through inspiration and expiration. Which medication was most likely utilized?
Question Answer Choices
- Etomidate
- Fentanyl
- Ketamine
- Midazolam
- Propofol
Question Explanation
Correct answer: C. Ketamine
The sudden onset of stridor and respiratory distress in conjunction with the visualization of fully adducted vocal cords is likely caused by laryngospasm. Of all the listed agents used for procedural sedation, ketamine is the only agent associated with laryngospasm. It is fortunately a rare adverse effect, occurring in less than 0.3% procedural sedations in a recent meta-analysis. Treatment for the laryngospasm is to perform a jaw thrust while simultaneously placing firm inward and anterior pressure on Larson’s point, also called the “laryngospasm notch.”
It is located behind the lobule of the ear just posterior to the ascending ramus of the mandible. If this is unsuccessful, deepening the sedation or giving a short-acting paralytic agent (e.g., succinylcholine) and securing the airway with intubation is another option. Some sources also mention the potential to use a supraglottic device after succinylcholine with the thought being that intubation can further irritate the cords and cause recurrent laryngospasm.
Ketamine is typically given in an initial dose of 1-2mg/kg IV, with repeat dosing of 0.5-1mg/kg every three- to five-minutes to achieve adequate sedation. Time of onset is less than one minute, and duration of action is five- to 10-minutes. Common side effects include tachycardia, hypertension, increased respiratory secretions and nausea. Less commonly, an “emergence reaction” may be seen with acute confusion, agitation and hallucinations. Administration of a low-dose benzodiazepine (midazolam 0.05mg/kg) or 5mg of haloperidol prior to awakening has been shown to greatly reduce occurrence.
Incorrect answer choices:
Etomidate (Choice A) is an ultrashort-acting, non-barbiturate hypnotic anesthetic agent. Etomidate has a minimal effect on blood pressure, making it a good choice for sedation in the setting of trauma, hypovolemia or patients with significant cardiovascular disease. For procedural sedation, it is typically given at 0.15mg/kg dosing, and duration of action of eight- to 10-minutes. Adverse reactions include myoclonus, pain at the injection site and adrenal suppression (of unlikely clinical significance in one-time dosing). It is not known to cause laryngospasm, which was the cause of this patient’s apnea.
Fentanyl (Choice B) is a short-acting synthetic opiate used for analgesia. It is often combined with a benzodiazepine for procedural sedation. Analgesic effects last 30- to 60-minutes. Side effects include respiratory depression, nausea and emesis. Chest wall rigidity, or wooden chest syndrome, is a rare, but potentially life-threatening adverse reaction, in which marked muscle rigidity of the thoracic and abdominal muscles makes spontaneous or even assisted ventilation highly difficult.
Treatment consists of reversal of the opiate with naloxone, and potentially administering a short-acting neuromuscular blocking agent and intubation. Although ventilation would be very difficult in the settings of both laryngospasm and chest wall rigidity, the visual clue showing the vocal cords fully adducted and the preceding stridor points to laryngospasm as the cause for this patient’s respiratory distress.
Midazolam (Choice D) is a short-acting benzodiazepine commonly used for procedural sedation. Duration of action is 30- to 60-minutes when given intravenously. Typical initial dose is 0.02-0.1 mg/kg IV. Side effects are respiratory depression, and when used in combination with an opiate, hypotension. Benzodiazepine overdose may be reversed with flumazenil, but is rarely utilized. It is not known to cause laryngospasm.
Propofol (Choice E) is an ultra-short acting sedative. Its time of onset is less than one minute and duration of action is three- to 10-minutes. Typical initial dose is 0.5-1 mg/kg IV loading dose with repeat doses of 0.5 mg/kg increments q3-5min to achieve sedation. Side effects are respiratory depression and hypotension. It is not known to cause laryngospasm.