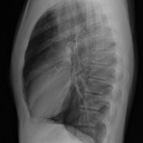
CR’s mother called her pediatrician’s office again later in the afternoon. She reported that the facial swelling was looking worse to her. She also forgot to mention earlier that she had noticed a change in CR’s voice over the past 2-3 days. The pediatrician was concerned that this could be a presentation of Mumps…but she was closing for the day, so she asked the mother to take CR to a local urgent care clinic. CR’s mother agreed and they presented at the clinic where a CXR was done. No radiologist was on hand and the CXR looked “abnormal”, so they were referred to the emergency department.
CR’s mother called her pediatrician’s office again later in the afternoon. She reported that the facial swelling was looking worse to her. She also forgot to mention earlier that she had noticed a change in CR’s voice over the past 2-3 days. The pediatrician was concerned that this could be a presentation of Mumps…but she was closing for the day, so she asked the mother to take CR to a local urgent care clinic. CR’s mother agreed and they presented at the clinic where a CXR was done. No radiologist was on hand and the CXR looked “abnormal”, so they were referred to the emergency department.
 Physical exam was significant for a notable voice change. Oropharynx was clear. CR was noted to have swollen cheeks with palpable crepitus along bilateral sides of neck and under his mandible. This crepitus extended down through the chest wall and was palpable bilaterally to the level of the 12th ribs (positive “rice-crispy sign”). Cardiac exam showed normal heart sounds with no audible “crunch” (negative Hamman sign). CR had clear breath sounds, no wheezing, no noted retractions.
Physical exam was significant for a notable voice change. Oropharynx was clear. CR was noted to have swollen cheeks with palpable crepitus along bilateral sides of neck and under his mandible. This crepitus extended down through the chest wall and was palpable bilaterally to the level of the 12th ribs (positive “rice-crispy sign”). Cardiac exam showed normal heart sounds with no audible “crunch” (negative Hamman sign). CR had clear breath sounds, no wheezing, no noted retractions.FINDING: Pneumomediastinum, also known as the “Macklin Effect” was first described in 1939. Pathophysiology: In cases not due to primary trauma or esophageal tear, alveolar wall rupture occurs secondary to high intra-alveolar pressure caused by artificial ventilation, coughing, straining, a prolonged Valsalva maneuver, retching, labor, scuba diving (barotrauma) or inhalation of alkaloidal cocaine…thus allowing leakage of air into the perivascular connective tissue. This air will then track along tissue planes. Pneumomediastinum is usually a benign self limiting condition that occurs most frequently in young healthy males. Patients should be worked-up to look for the “air leak source” and admitted for an observation period. Physicians should note that subcutaneous palpable air is the most consistent physical exam finding. In our patient, it was felt that the etiology of his pneumomediatstinum was due to his acute choking episode 5-6 days prior to his presentation.