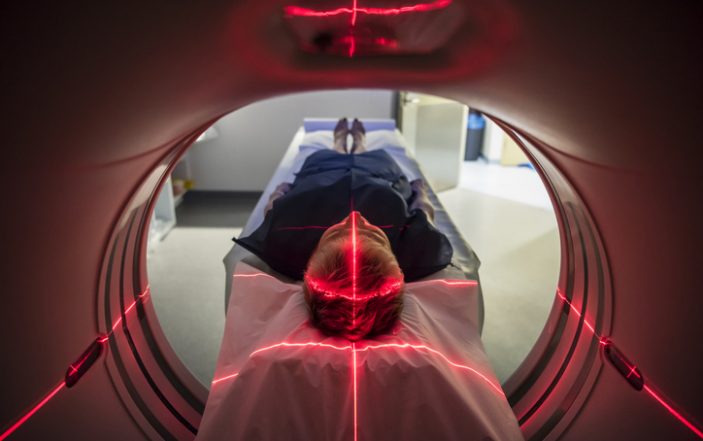
The benefits of radiation exposure from diagnostic imaging requires nuance.
I can recall as a medical student agonizing over the indications for computed tomography (CT) imaging in the emergency department.
While trying to formulate my assessment and plan, I felt that ordering a CT scan was wasteful, harmful and a failure of the skills I had worked so hard to acquire during medical school, where I was taught that history and physical examination are key to diagnosis.
The tendency of emergency physicians to over-test and over-image is a common trope espoused by our non-emergency physician colleagues — so why feed into this stereotype? I recall hearing one statistic that a CT scan of the chest was equivalent to 500 chest x-rays. Watching everyone in the trauma bay don and doff their heavy lead jackets gave me the impression that even one x-ray was risky enough to avoid.
Clarifying Risk
Fast-forward to residency and this hesitancy has quickly dissipated because of both knowledge and experience. The American College of Radiology provides a concrete framework to discuss the risks of radiation from medical imaging. The ACR categorizes the amount of radiation exposure with each imaging study from negligible to moderate risk for developing a fatal cancer.[1] A CT scan of the abdomen and pelvis with IV contrast is classified as “low” risk. So how low is “low?”
The key statistic to understand is that (morbid as it sounds) we all have a 1 in 5 chance of dying from a lethal cancer.[2] The ACR’s “low risk” category corresponds to a 1 in 1,000 to 1 in 10,000 risk in excess of this baseline. Using the high end of the low risk category, a CT of the abdomen and pelvis would increase our baseline risk from 200 in a 1,000 (1 in 5) to a 201 in a 1,000 chance of dying from a lethal cancer.
When put that way, this radiation exposure really does seem rather benign considering the risks of missing an acute and potentially lethal condition.
Translated to practice, if my differential includes any life-threatening diagnosis that can be elucidated through computed tomography and has a pre-test probability greater than 0.001 (1 in 1,000) according to my clinical gestalt, I find it perfectly reasonable to order the scan. I often use this framework to discuss workups with my patients and I find they appreciate it when I talk about it in concrete terms.
One emergency physician, both older and wiser than I, once shared a simpler rule — if he gives IV opiates to any patient presenting to the emergency department with abdominal pain, he will obtain either a right-upper-quadrant ultrasound or CTAP as clinically indicated. Two years into my residency, I’ve found few other pearls as clinically useful, and it has yet to fail me.
The Linear-No Threshold Model
What’s often not discussed when it comes to radiation exposure and medical imaging is the theoretical framework justifying the harm from radiation. The linear no-threshold (LNT) model holds that no amount of radiation exposure is safe. It describes a linear response in excess risk of developing a lethal cancer with any amount of exposure (in other words, there is no threshold dose to cause harm).
This theory is based on fruit fly studies performed in the 1940s as well as epidemiologic data from the survivors of the Hiroshima and Nagasaki atomic bombings. These studies showed an increased risk of developing cancer due to the large doses of radiation the subjects received. However, these data have been criticized as the equivalent radiation dose the subjects were exposed to far exceeds that encountered with routine medical imaging.[3]
Additionally, several animal models using low doses of radiation have actually shown a reduction in solid tumors with radiation exposure.[4] French Academies of Science and Medicine stated that the LNT model should not be extrapolated to radiation doses less than 100 millisieverts (mSv).[5] For comparison, one CT of the abdomen and pelvis gives a radiation dose of approximately 8 mSv. Iit should be noted that the United States National Academy of Sciences embraces the LNT model.[6]
A Competing Model: Therapeutic Radiation?
Given the limitations of the LNT model, a competing model of radiation “hormesis” has been developed, which postulates that very low levels of radiation exposure may actually be protective by upregulating cellular defense mechanisms that repair damaged DNA. As mentioned previously, animal models have shown reduced tumor incidence with low levels of radiation, thought to be from the body trying to compensate for a disruption in homeostasis.
Additionally, while one study of mice found a reduction in lifespan with large single dose of radiation, mice exposed to a smaller dose actually lived longer than the controls who received no radiation.[7] While we often joke about providing “therapeutic radiation” when we encounter the worried-well, it turns out this concept isn’t completely unfounded.
Conclusion
The debate over the danger posed by diagnostic radiation is complicated. Regardless of whether the LNT or hormetic model is more valid, it’s certain that balancing the risks and benefits of radiation exposure from diagnostic imaging requires nuance and understanding. Being able to appreciate this nuance and communicate it to our patients is essential to delivering high-quality care in the emergency department.
References:
- American College of Radiology. Radiation Safety. ACR.org. Accessed August 8th, 2020. Retrieved from: https://www.acr.org/Clinical-Resources/Radiology-Safety/Radiation-Safety
- Food and Drug Administration. What are the Radiation Risks from CT? fda.gov. December 5, 2017. Accessed April 8, 2021. https://www.fda.gov/radiation-emitting-products/medical-x-ray-imaging/what-are-radiation-risks-ct
- Sacks B, Meyerson G, Siegel JA. Epidemiology Without Biology: False Paradigms, Unfounded Assumptions, and Specious Statistics in Radiation Science (with Commentaries by Inge Schmitz-Feuerhake and Christopher Busby and a Reply by the Authors). Biol Theory. 2016;11:69-101. doi:10.1007/s13752-016-0244-4
- Calabrese, E. J., & Baldwin, L. A. (2003). Toxicology rethinks its central belief. Nature, 421(6924), 691–692. doi:10.1038/421691a
- Tubiana M, Aurengo A, Averbeck D, et al, eds. Dose-effect relationships and the estimation of the carcinogenic effects of low doses of ionizing radiation. Academy of Medicine (Paris) and Academy of Science (Paris) Joint Report No. 2, March 30, 2005.
- National Research Council. (2006). “Hormesis and Epidemiology”. Health Risks from Exposure to Low Levels of Ionizing Radiation: BEIR VII Phase 2. Washington, DC: The National Academies Press. p. 335. doi:17226/11340. ISBN 978-0-309-09156-5.
- Maisin JR, Gerber GB, Vankerkom J, Wambersie A. Survival and diseases in C57BL mice exposed to X rays or 3.1 MeV neutrons at an age of 7 or 21 days. Radiat Res. 1996;146(4):453-460.