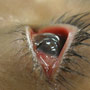
An up-close look at how to care for a potentially-ruptured globe in the emergency department.
A 26-year-old male presented to the emergency department complaining of severe left eye pain and loss of vision to that eye. He explains that while cleaning he dropped a ceramic pot, which shattered, and a piece of shrapnel stuck him in the eye. In addition to his visual complaints, he’s been nauseous, and has vomited several times.
On presentation, the patient was bradycardic with a heart rate of 38, was normotensive. Otherwise, vital signs were unremarkable. He was generally uncomfortable and in distress secondary to his pain. He was alert and mentating well. His eye exam is depicted in the image. His vision was intact only to light/dark. The rest of his physical exam was unremarkable.
 The Discussion
The Discussion
Globe rupture, whether from penetrating or blunt trauma, is an ophthalmologic emergency that requires immediate specialist consultation. In cases of penetrating trauma, rupture may be secondary to scleral or corneal lacerations and if there is injury to the cornea, the classic “teardrop” pupil may be seen on physical examination. This finding is a result of the iris plugging the wound in the cornea and disfiguring the pupil. The narrowest part or apex of the teardrop points to the site of the injury.
Rupture resulting from blunt injury occurs in 3.5% of patients with direct blunt eye trauma but can be more difficult to diagnose. A rapid increase in intraocular pressure (IOP) secondary to trauma often leads to rupture where the sclera is the thinnest, i.e. the limbus or the insertions of the intraocular muscles. Rupture may also occur directly across from the site of impact. If the rupture occurs at the limbus, the teardrop pupil may be seen.
Other physical exam findings include bloody chemosis, pronounced subconjunctival hemorrhage, vitreous hemorrhage or periauricular hemorrhage. In patients with blunt trauma, eyelid and periorbital edema can be seen and may make examination of the globe difficult. Visual acuity is often limited to light/dark differentiation or less. Patients may also demonstrate secondary, systemic findings of intraocular injury such as vomiting or bradycardia.
Any penetrating injury to the eye should be presumed as penetrating to the globe, and at the first suspicion of globe rupture care should be taken to protect the eye from further injury or manipulation with use of a Fox shield or a shield manufactured from a cup. In patients with periorbital edema, extreme care must be taken to avoid putting pressure on the globe when opening the lids. If it is unclear if perforation has occurred after initial examination, additional diagnostic tests may be performed. Seidel’s test is performed by placing a generous amount of fluorescein into the eye and then looking for a stream of dye surrounded by a pool of dye when observed under cobalt light. While ultrasound can be used to diagnose globe rupture as well as to look for foreign body, in the case of penetrating trauma, extreme care must be taken so as not to apply any pressure to the eye itself. As a result, some suggest that ultrasound is contraindicated in any case of suspected globe rupture. CT scans are also useful and should be performed in most cases of suspected penetrating trauma to evaluate for foreign bodies. While decreased IOP is indicative of rupture, tonometry is not recommended in suspected globe rupture due to concerns of further injury to the eye.
Treatment
Emergency department treatment of globe rupture is centered on preventing further injury to the eye. Additionally, patients should have their tetanus updated and should be started on broad-spectrum parenteral antibiotics. Patients should be kept nothing by mouth and provided with symptomatic care for pain and nausea. In patients that develop bradycardia, unless they become hypotensive, have changes in their mental status or become otherwise symptomatic from their bradycardia, they should only be monitored. Patients will need definitive surgical treatment and should be admitted to the hospital or operating room.
There is still some controversy surrounding the use of succinylcholine in globe rupture if patients require intubation, as there is a risk of rise in IOP. However, this theoretical concern has not played out in the literature, as studies have failed to demonstrate any adverse effects of succinylcholine on patients with globe rupture. Similarly, ketamine, while not directly studied in patients with globe rupture, does not appear to substantially raise IOP but research is limited in this area.
Case Resolution
This particular patient had a Fox shield placed over his eye, was provided pain control with IV narcotics and started on broad-spectrum antibiotics. He remained comfortable and apart from his bradycardia remained hemodynamically stable. After his CT scan, which showed suprachoriodal hemorrhage involving the anterior and lateral aspects of the globe and decreased fluid in the anterior chamber consistent with globe rupture, he was transferred to the operating room. He underwent primary repair of the corneal laceration and his iris was repositioned from where it had prolapsed and become incarcerated. He was continued on an oral fluoroquinolone and started on steroid eye drops, antibiotic eye drops and a cycloplegic. At one day follow up his vision in the affected eye was 20/400 and at 2-week follow up his vision had improved to 20/100.
References:
- Marx, JA, et al, ed. Rosen’s Emergency Medicine Concepts and Clinical Practice. 7th Edition. Philadelphia: Mosby Elsevier, 2010.
- Wolfson AB. Hardwood-Nuss’ Clinical Practice of Emergency Medicine. Philadelphia: Lippincott Williams & Wilkins, 2005.
- Drayna PC, Estrada C, Wang W et al. Ketamine sedation is not associated with clinically meaningful elevation of intraocular pressure. Am J Emerg Med. Epub 2011.
- Dunkin JM, Crum AV, Swanger RS and SA Bokhari. Globe Trauma. Semin Ultrasound CT MRI 2011;32:51-56.
- Peuler M, Glass DD, Arens JF. Ketamine and intraocular pressure. Anesthesiology 1975;43:575–578.