Look for ECG abnormalities in SAH.
Case Report:
A 60-year-old female with a significant past medical history of hypertension presented to the emergency department with the chief complaint of double vision, headache and elevated blood pressure. She stated she was cleaning her house a week prior to arrival when she felt an acute onset of a headache, described as a ‘pounding’ type sensation, reaching maximum intensity within 30-minutes. She had been using multiple ice packs, up to six at a time applied to her head and neck consistently for a week, along with acetaminophen and ibuprofen without any relief.
She presented today when she started getting double vision and multiple episodes of vomiting. Vitals on arrival to the ED: temp 97.8 °F, respiratory rate of 26 breaths/min, heart rate 70 beats/min, blood pressure of 179/81 mmHg, weight of 73.9 kg, and 97% pulse ox on room air. On physical exam she was in distress secondary to the headache. The light was turned off and she brought her ice packs from home and placed them around her head and neck. Her pupils were equal, round and reactive to light.
Extra-ocular muscles were intact bilaterally. Pupils were 3 mm and reactive bilaterally. Intraocular pressures were 27 and 28 respectively. Examination of the neck revealed the patient to have pain with flexion of the neck, however, Kernig’s sign and Brudzinski’s sign were both negative. Neurologic exam revealed no acute focal deficits and no meningeal signs. No other acute findings were found on physical exam.

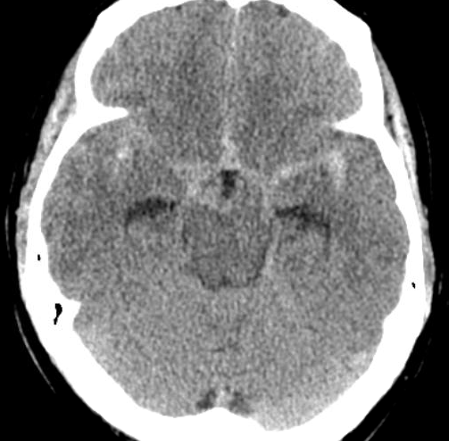
Electrocardiogram, image A, revealed sinus rhythm at 66 with T-wave inversions in lead 1, aVL, and V2, concerning for cerebral T-waves. CT Stroke Protocol of the head and brain without contrast, image B, revealing diffuse subarachnoid hemorrhage with intraventricular extension into the third ventricle.

No other acute laboratory abnormalities were noted on evaluation including cardiac enzymes. The patient was placed on a nicardipine drip starting at 5 mg/hr (goal blood pressure <140/90), analgesia given, head of the bed elevated >30 degrees, and neurosurgery was immediately consulted. The patient was taken to the angiography suite for coiling of her aneurysmal subarachnoid hemorrhage. Her hospital course was unremarkable, and she was discharged seven days later.
Discussion:
In an aneurysmal subarachnoid hemorrhage (aSAH), there is an extravasation of high-pressure arterial blood within the subarachnoid space, resulting in an increased ICP.[1] Blood most commonly collects around the circle of Willis (65%) or the Sylvian fissure (30%), with the sylvian fissure associated with the deeper hypothalamus and insular cortex, supplied by the MCA.[1,2]
An aSAH is among the neurological emergencies with a high degree of morbidity and mortality. While classical symptoms of aSAH include sudden onset severe headache (often reaching maximum intensity within an hour), nausea/vomiting, neck stiffness, positive Kernig’s sign, positive Brudzinski’s sign, and eventual altered mental status, electrocardiographic (ECG) abnormalities and cardiovascular complications have been well documented within the medical literature.
The exact mechanism behind ECG abnormalities in the setting of intracranial pathology is not well understood, with autonomic dysregulation and hypothalamic stimulation among the top suggested mechanisms. The phenomenon appears to share similarities with Takotsubo cardiomyopathy.
aSAH can result in a neurologically stunned myocardium (also called neurogenic stress cardiomyopathy), involving cardiopulmonary damage secondary to excessive catecholamine release from substantial activation of the sympathetic nervous system by a damaged insular cortex.[1,3] The overstimulation and autonomic imbalance can result in injured sub-endocardial myocytes, transient LV dysfunction, cardiogenic shock, pulmonary edema, and lethal arrhythmias.[2,4]
Research has shown that 28% of patients will present with an elevated troponin within 24 hours, 28% with wall motion abnormalities on echo, and 35% with arrhythmias (ventricular tachycardia, ventricular fibrillation, torsades de pointes, PEA (7% of all PEA arrest cases)[1], atrial fibrillation and third-degree heart block).[1,6]
In one study by Kumral et al, ECG abnormalities were observed in 90% of patients with aSAH, the remaining 10% did not have any ECG abnormalities.[7] The most common ECG abnormalities encountered in the ED in patients with a SAH include:
- QT prolongation
- T-wave inversion (referred to as cerebral T-waves)
- ST-segment depression
- Other ECG changes can include: U waves, tachycardia, bradycardia, P-wave changes, shortened PR, and ST-segment depression.[2]
Cerebral T-waves are classically described as transient deep T-wave inversion or large upright peaked T-waves.[2] In one case series, cerebral T-waves were identified in 72% of patients with aSAH and 57% of patients with an intraparenchymal hemorrhage.[6]
While the ECG did not change the clinical course of this patient (head CT was already ordered based on clinical presentation), it is important for the ED physician to be aware of the potential ECG abnormalities and cardiovascular complications associated with intracranial pathology, such as aSAH.
References:
- Murphy, D, Johnson, N. “Cardiac Complications from Subarachnoid Hemorrhage.” EMRA. 4/15/2018.
- Stone, J, Mor-Avi, V, Ardelt, A, Lang, R. “Frequency of Inverted Electrocardiographic T Waves (Cerebral T Waves) in Patients With Acute Strokes and Their Relation to Left Ventricular Wall Motion Abnormalities.” American Journal of Cardiology. 2018;121:120-124.
- Saritemur, M, Kalkan, K, Emet, M. “Case Report: Intracranial hemorrhage with electrocardiographic abnormalities and troponin elevation.” American Journal of Emergency Medicine. 2013. 31.271.e5-271.e7
- Mayer, S, Fink, M, Homma, S, Sherman, D, Lennihan, L, Solomon, R, et al. “Cardiac injury associated with neurogenic pulmonary edema following subarachnoid hemorrhage. Neurology 1994;44:815-20.
- Emergency Medicine News. “Don’t Forget The Heart after Subarachnoid Hemorrhage.” David Murphy.
- Cadogan, M. “Raised Intracranial Pressure.” Life in the Fastlane. November 18, 2018. https://litfl.com/raised-intracranial-pressure-ecg-library/
- Kumral, E, Isler, M, Terzioglu, E, Yilmaz, H. “Electrocardiographic findings in hemorrhagic stroke: subarachnoid hemorrhage.” Arch Turk Soc Cardiology 1990;18:35-8.
- Chatterjee, S. “ECG Changes in Subarachnoid Hemorrhage: A Synopsis.” Netherlands Heart Journal. 2011. Jan; 19(1): 31-34.